Erythropoiesis Definition
Erythropoiesis is the process of the origin, development, and maturation of erythrocytes. Hemopoiesis or hemato-poiesis is the process of origin, development, and maturation of all the blood cells.
Table of Contents
Site Of Erythropoiesis
In Fetal Life: In fetal life, erythropoiesis occurs in three stages:
- Mesoblastic Stage: During the first two months of intrauterine life, the RBCs are produced from the mesenchyme of the yolk sac.
- Hepatic Stage: From third month of intrauterine life, liver is the main organ that produces RBCs. The spleen and lymphoid organs are also involved in erythropoiesis.
- Myeloid Stage: During the last three months of Intrauterine life, the RBCs are produced from red bone marrow and liver.
Read And Learn More: Medical Physiology Notes
In Newborn Babies, Children, And Adults: In newborn babies, growing children, and adults, RBCs are produced only from the red bone marrow.
- Up to the age of 20 years: RBCs are produced from red bone marrow of all bones (long bones and all the flat bones).
- After the age of 20 years: RBCs are produced from membranous bones like vertebra, sternum, ribs, scapula, iliac bones, and skull bones and from the ends of long bones After 20 years of age, the shaft of the long bones becomes yellow bone marrow because of fat deposition and loses the erythropoietic function.
- In adults, the liver and spleen may produce the blood cells If the bone marrow is destroyed or fibrosis. Collectively bone marrow is almost equal to the liver.
- In size and weight. It is also as active as liver. Though bone marrow is the site of production of all blood cells, comparatively 75% of the bone marrow is Involved in the production of leucocytes and only 25% is involved in the production of erythrocytes.
- But still, the leucocytes are less in number than the erythrocytes, the ratio being 1:500. This is mainly because of the life span of these cells.
- Life span of erythrocytes is 120 days whereas the life span of leukocytes is very short ranging from one to ten days. So the leukocytes need larger production than erythrocytes to maintain the required number.

Process Of Erythropoiesis
Stem Cells
- Stem cells are the primary cells capable of self-renewal differentiating into specialized cells. Hemopoietic stem cells are the primitive cells in the bone marrow that give rise to the blood cells.
- The hemopoietic stem cells in the bone marrow are called uncommitted pluripotent hemopoietic stem cells (PHSC). PHSC is defined as a cell that can give rise to all types of blood cells. In the early stages, the PHSC are not designed to form a particular type of blood cell.
- And it is also not possible to determine the blood cell to be developed from these cells: hence, the name uncommitted PHSC.
- In adults only à few number of these cells are present. But the best source of these cells is the umbilical cord blood.
- When the cells are designed to form a particular type of blood cell, the uncommitted PHSCs are called committed PHSCs. Committed PHSC is defined as a cell which is restricted to give rise to one group of blood cells.
The committed PHSCs are of two types:
- Lymphoid stem cells (LSC) which give rise to lymphocytes and natural killer (NK) cells
- Colony-forming blastocytes, which give rise to myeloid cells. Myeloid cells are the blood cells other than lymphocytes. When grown in cultures, these cells form colonies hence the name colony forming blastocytes
- The different units of colony-forming cells are:
- Colony Forming Unit – Erythrocytes (CFU-E). The cells of this unit develop into erythrocytes
- iColony Forming Unit – Granulocytes/Monocytes (CFU-GM). These cells give rise to granulocytes (neutrophils, basophils, and eosinophils) and Monocytes
- Colony Forming Unit – Megakaryocytes (CFU-M). Platelets are developed from these cells.
- The different units of colony-forming cells are:
Changes During Erythropoiesis: The cells of CFU-E pass through different stages and finally become the matured RBCs. During these stages four important changes are noticed.
- Reduction in size of the cell (from the diameter of 25-7.2 μ)
- Disappearance of nucleoli and nucleus
- Appearance of hemoglobin
- Change in the staining properties of the cytoplasm.
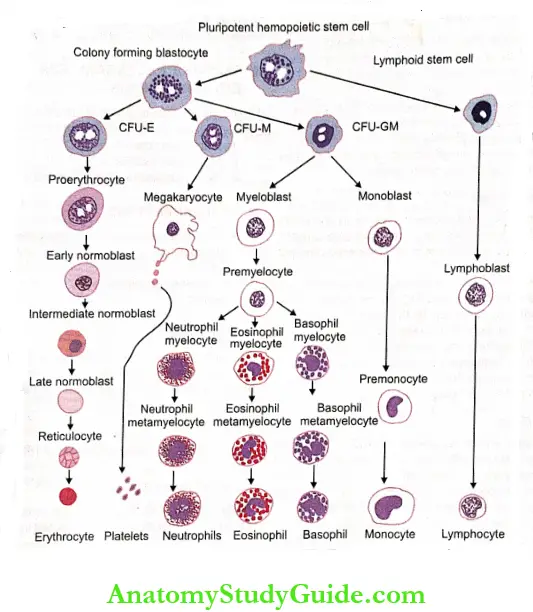
- CFU-E = Colony forming unit – Erythrocyte,
- CFU-M = Colony forming unit – Megakaryocyte,
- CFU-GM = Colony forming unit -Granulocyte/Monocyte
Stages Of Erythropoiesis: The various stages between CFU-E cells and matured RBC are:
- Proerythroblast
- Early normoblast
- Intermediate normoblast
- Late normoblast
- Reticulocyte
- Matured erythrocyte.
1. Proerythroblast (Megaloblast):
- Proerythroblast or megaloblast is the first cell derived from CFU-E. It is very large in size with a diameter of about 20 p.
- Its nucleus is large and occupies the cell almost completely. The nucleus has two or more nucleoli and a reticular network. The proerythroblast does not contain hemoglobin.
- The cytoplasm is basophilic in nature. The proerythroblast multiplies several times and finally forms the cell of next stage called early normoblast.
2. Early Normoblast
- It is little smaller than a proerythroblast with a diameter of about 15 μ. In the nucleus, the nucleoli disappear. Condensation of the chromatin network occurs.
- The condensed network becomes dense. The cytoplasm is basophilic in nature: So, this cell is also called basophilic erythroblast. This cell develops into next stage called intermediate normoblast.
3. Intermediate Normoblast
- This cell is smaller than the early normoblast with a diameter of 10 to 12μ. The nucleus is still present.
- But, the chromatin network shows further condensation. The hemoglobin starts appearing.
- The cytoplasm is already basophilic. Now, because of the presence of hemoglobin, it stains with both acidic as well as basic stains. So this cell is called polychromophilic or polychromatic erythroblast.
- This cell develops into next stage called late normoblast.
4. Late Normoblast: The diameter of the cell decreases further to about 8 to 10 μ. Nucleus becomes very small with very much condensed chromatin network and it is known as ink spot nucleus.
- Quantity of hemoglobin increases. And the cytoplasm becomes almost acidophilic. So, the cell is now called orthochromatic erythroblast. In the final stage of late normoblast just before it passes to the next stage, the nucleus disintegrates and disappears.
- The process by which nucleus disappears is called pyknosis. The final remnant is extruded from the cell. Late normoblast develops into the next stage called reticulocyte.
5. Reticulocyte
- It is otherwise known as immature RBC. It is slightly larger than matured RBC. The cytoplasm contains the reticular network or reticulum which is formed by remnants of disintegrated organelles.
- Due to the reticular network, the cell is called a reticulocyte. The reticulum of reticulocyte stains with supravital stain.
- In newborn babies, the reticulocyte count is 2-6% of RBCs, i.e. 2-6 reticulocytes are present for every 100 RBCs.
- The number of reticulocytes decreases during the first week after birth. Later, the reticulocyte count remains constant at or below 1% of RBCs. The number increases whenever the production and release of RBCs increase.
- The reticulocyte is basophilic due to the presence of remnants of disintegrated Golgi apparatus, mitochondria, and other organelles of cytoplasm.
- During this stage, the cells enter the capillaries through the capillary membrane from source of production by diapedesis.
6. Matured Erythrocyte
- The reticular network disappears and the cell becomes the matured RBC and attains the biconcave shape. The cell decreases in size to 7.2 μ diameter.
- The matured RBC is with hemoglobin and without nucleus.
- It requires seven days for the development and maturation of RBC from proerythroblast. It requires five days up to the stage of reticulocyte.
- The reticulocyte takes two more days to become the matured RBC.
Factors Necessary For Erythropoiesis
Development and maturation of erythrocytes require a variety of factors which are classified into 3 categories:
- General factors
- Maturation factors
- Factors necessary for hemoglobin formation.
1. General Factors: General factors necessary for erythropoiesis are:
- Erythropoietin
- Thyroxine
- Hemopoietic growth factors
- Vitamins.
- Erythropoietin: The most important general factor for erythropoiesis is the hormone called erythropoietin. It is also called hemopoietin or erythrocyte stimulating factor.
- Chemistry: Erythropoietin is a glycoprotein with 165 amino acids.
- Source of secretion: Major quantity of erythropoietin is secreted by peritubular capillaries of kidney. It is also secreted in liver and brain.
- Stimulant for secretion: Hypoxia is the stimulant for the secretion of erythropoietin.
- Actions of erythropoietin: Erythropoietin causes formation and release of new RBCs into circulation. After secretion, it takes 4-5 days to show the action.
Erythropoietin promotes the following processes:
- Production of proerythroblasts from CFU-E of the bone marrow
- Development of proerythroblasts into matured RBCs through the several stages – early normo- blast, intermediate normoblast, late normoblast, and reticulocyte
- Release of matured erythrocytes into blood. Even some reticulocytes (immature erythrocytes) are released along with matured RBCs. The blood level of erythropoietin increases in anemia.
- Thyroxine: Being a general metabolic hormone, thyroxine accelerates the process of erythropoiesis at many levels. So, polycythemia is common in hyperthyroidism.
- Hemopoietic Growth Factors:
- Hemopoietic growth factors or growth inducers are the interleukins and stem cell factor (steel factor). Generally, these factors induce the proliferation of PHSCs.
- Interleukins (IL) are glycoproteins that belong to the cytokines family. The interleukins involved in erythropoiesis
are:- Interleukin-3 (IL-3) secreted by T cells
- Interleukin-6 (IL-6) secreted by T cells, endothelial cells, and macrophages
- linterleukin-11 (IL-11) secreted by osteoblast.
- Vitamins: Some vitamins are also necessary for the process of erythropoiesis. The deficiency of these vitamins cause anemia associated with other disorders. The vitamins, which are necessary for erythropoiesis are:
- Vitamin B: Its deficiency causes anemia and pellagra (a disease characterized by skin lesions, diarrhea, weakness, nervousness, and dementia)
- Vitamin C: Its deficiency causes anemia and scurvy (an ancient disease characterized by impaired collagen synthesis resulting in rough skin, bleeding gum, loosening of teeth, poor wound healing, bone pain, lethargy, and emotional changes)
- Vitamin D: Its deficiency causes anemia and rickets
- Vitamin E: Its deficiency leads to anemia and malnutrition.
Maturation Factors: Vitamin B12, intrinsic factor, and folic acid are necessary for the maturation of RBCs.
1. Vitamin B12 (Cyanocobalamin): Vitamin B12 is the maturation factor necessary for erythropoiesis.
Source:
- Vitamin B12 is called extrinsic factor since it is obtained mostly from diet. Its absorption from the intestine requires the presence of the intrinsic factor of Castle.
- Vitamin B12 is stored mostly in liver and in small quantities in muscle.
- When necessary, it is transported to the bone marrow to promote maturation of RBCs.
- It is also produced in the large intestine by the intestinal flora.
Action:
- Vitamin B12 is essential for synthesis of DNA in RBCs. Its deficiency leads to failure in the maturation of the cell and reduction in the cell division.
- Also, the cells are larger with fragile and weak cell membrane resulting in macrocytic anemia.
- The deficiency of vitamin B12 causes pernicious anemia. So, Vitamin B12 is called antipernicious factor.
2. Intrinsic Factor of Castle:
- It is produced in gastric mucosa by the parietal cells of the gastric glands.
- It is essential for the absorption of vitamin B12 from intestine. In the absence of intrinsic factors, vitamin B12 is not absorbed from the intestine.
- This leads to pernicious anemia. The deficiency of intrinsic factor occurs in the:
- Severe gastritis
- Ulcer
- Gastrectomy.
The extrinsic and intrinsic factors are together called hematinic principle which is the maturation factor.
3. Folic Acid:
- Folic acid is also essential for maturation. It is required for the synthesis of DNA. In the absence of folic acid, the synthesis of DNA decreases causing failure of maturation.
- This leads to anemia in which, the cells are larger and appear in the megaloblastic (proerythroblastic) stage. And the anemia due to the folic acid deficiency is called megaloblastic anemia.
Factors Necessary For Hemoglobin Formation
Various materials are essential for the formation of hemoglobin in the RBCs. The deficiency of these substances decreases the production of hemoglobin leading to anemia. Such factors are:
- First-class proteins and amino acids: Proteins of high biological value are essential for the formation of hemoglobin. Amino acids derived from these proteins are required for the synthesis of protein part of hemoglobin, the globin.
- Iron: It is necessary for the formation of the heme part of the hemoglobin.
- Copper: It is necessary for the absorption of iron from the gastrointestinal tract.
- Cobalt and nickel: These metals are essential for the utilization of iron during hemoglobin formation.
- Vitamins: Vitamin C, riboflavin, nicotinic acid, and pyridoxine are also essential for the formation of hemoglobin.
Leave a Reply