Herpesviruses And Other DNA Viruses
Herpesviruses
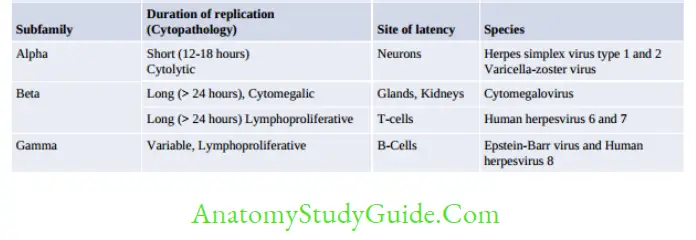
The members of Herpesviridae possess the following properties:
Table of Contents
- Large (150–200 nm size), spherical in shape with icosahedral symmetry.
- Tegument: It is an amorphous, asymmetric structure present between the capsid and envelope
- Establish latent or persistent infections in their hosts and undergo periodic reactivation
- Possess dsDNA and replicates by rolling circle mechanism.
Read And Learn More: Micro Biology And Immunology Notes
Herpes Simplex Virus


Clinical Manifestations
The incubation period ranges from 1 to 26 days (median, 6–8 days).
Orofacial mucosal lesions: They are the most common manifestations of HSV.
- Most common affected site is buccal mucosa
- Most frequent primary lesions are gingivostomatitis and pharyngitis.
- Most frequent recurrent lesion is herpes labialis (painful vesicles near lips).
Nervous system
- Encephalitis: HSV is the MC cause of acute sporadic viral encephalitis (MC site temporal lobe), HSV-1 causes > 95% of cases.
- Children get primary infection: HSV is acquired exogenously and invades CNS via the olfactory bulb
- Adults get recurrent infections due to reactivation of HSV in trigeminal nerve.
- Meningitis: HSV can cause recurrent lymphocytic meningitis called as Mollaret’s meningitis
- Other manifestations:
- Autonomous nervous system involvement (sacral region)
- Transverse myelitis
- Guillain-Barré syndrome
- Peripheral nervous system involvement (for example., Bell’s palsy)
- Cutaneous lesions: HSV usually infects through abraded skin and causes various lesions.
- Herpetic whitlow: Lesions present on the fingers of dentists and hospital personnel.
- Febrile blisters:
- Herpes gladiatorum: Mucocutaneous lesions present on the body of wrestlers.
- Eczema herpeticum: Caused by HSV-1 in patients with chronic eczema. Similar lesions are also produced by vaccinia virus infection; both conditions together are designated as Kaposi’s varicelliform eruptions.
- Erythema multiforme: HSV is the most common to be associated.
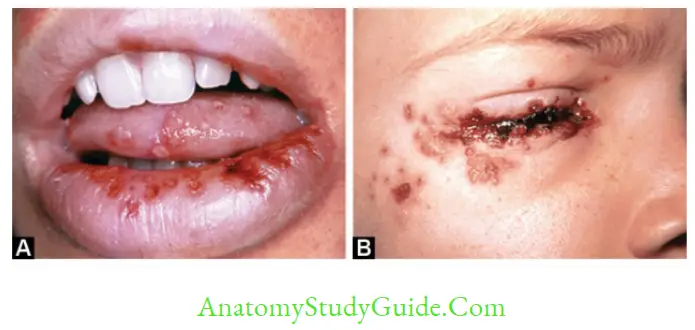
Ocular lesions: HSV-1 is more common than HSV-2 to infect eyes.
- Severe conjunctivitis is the most common manifestations
- Recurrent lesions develop in to dendritic ulcers of cornea or vesicles on the eyelids.
- Corneal blindness:
Genital lesions: HSV-2 is more common than HSV-1 to cause primary as well as recurrent genital lesions.
- Genital lesions are described as bilateral, painful multiple, tiny vesicular ulcers
- This may be associated with fever and inguinal lymphadenopathy.
Visceral and disseminated herpes
- Risk factors: Immunocompromised patients, underlying malnutrition or AIDS, pregnancy.
- Common manifestations include: Pneumonitis, tracheobronchitis and hepatitis.
Neonatal Herpes: HSV is one of the common causes of congenital infections, along with the other TORCH agents.
- Transmission: Can also occur in utero or after birth; but MC being during birth.
- Risk of developing neonatal herpes is maximum (10 times more) if the mother recently acquires the virus (primary infection).
- HSV-2 is more common to cause neonatal herpes (75% of total cases) than HSV-1.
- Have a higher tendency to develop visceral infections.
Laboratory Diagnosis
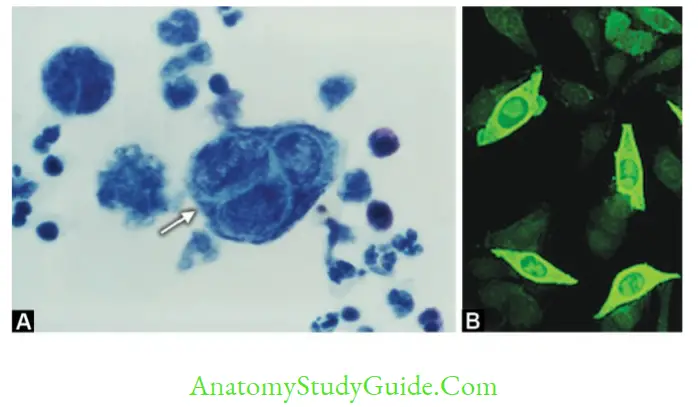
Cytopathology: Tzanck smear preparation by Wright’s or Giemsa stain:
-
- Detects inclusion bodies (Lipschultz body) and formation of multinucleated giant cells, ballooning of infected cells
- It cannot differentiate between HSV-1, HSV-2, and VZV
- Sensitivity of staining is low (< 30% for mucosal swabs).
- Virus isolation: Remains the most definitive tool for HSV diagnosis
- Conventional cell lines: Detects diffuse rounding and ballooning of cell lines.
- Viral antigen detection: in specimen by direct IF. It is sensitive, specific, and can differentiate HSV-1 from HSV-2.
- HSV DNA detection by PCR the most sensitive test and can differentiate HSV-1 and HSV-2.
- Antibody detection by ELISA or other formats
- Most available tests usually detect IgG or total antibodies, hence cannot differentiate recent and past infections.
- Serologic assays based on the type-specific antigens can differentiate between HSV-1 and HSV-2.
Treatment
- Acyclovir is the drug of choice for HSV encephalitis and neonatal herpes. It acts by inhibiting viral DNA polymerase.
Famciclovir and valacyclovir have been used. Topical idoxuridine,trifluorothymidine, topical vidarabine, and cidofovir are used for ocular infections. - Foscarnet is the DOC for acyclovir resistance cases.
Varicella Zoster Virus
VZV produces vesicular rashes on the skin and mucous membranes in two forms:
- Chickenpox: Diffuse bilateral vesicular rashes, occur following primary infection, usually affecting children.
- Zoster or Shingles: Occur following reactivation of latent VZV in the ophthalmic branch of trigeminal ganglia (which is also the site of latency of VZV).
It occurs mainly in adult life.
Vesicular rashes are unilateral and segmental.
Chickenpox
Clinical Manifestations
- Incubation period is about 10–21 days (2–3 weeks).
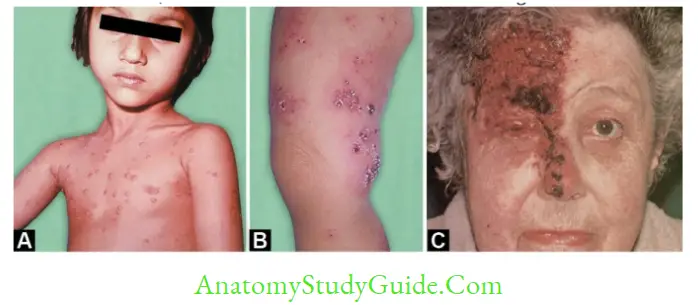
- Typical description of chickenpox rashes
- Vesicular, bilateral, diffuse and centripetal (start on the face and trunk, spread rapidly to involve flexor surfaces).
- Rashes appear in multiple crops, fever appears with each crop of rashes
- Chickenpox is a disease of childhood.
- When occurs in adults, it is more severe with bullous and hemorrhagic rash.
Complications
Complications are more common in adults and in immunocompromised individuals.
- MC infectious complication is: Secondary bacterial infection of the skin.
- MC extracutaneous complication: CNS involvement (cerebellar ataxia, encephalitis and aseptic meningitis): Usually occurs in children.
- Most serious complication is: Varicella pneumonia, develops commonly in pregnant women.
- Reye’s syndrome: Fatty degeneration of liver following salicylate (aspirin) intake.
Chickenpox in pregnancy affects both mother and the fetus.
Mothers are at high risk of developing varicella pneumonia - Fetal or congenital varicella syndrome: VZV is highly teratogenic.
- Risk is maximum when mother acquires a primary infection during early pregnancy (risk of transmission is 25%. However, the risk of developing into disease is 0.4% and 2% in infants whose mothers get chickenpox in <13 weeks and 13–20 weeks of gestation respectively).
- Late first trimester/early second trimester: Congenital malformation in fetusis more frequent, characterized by cicatricial skin lesions, limb hypoplasia and microcephaly.
- Infection near delivery
- If mother gets infection > 5 days before delivery: Then baby is mostly asymptomatic due to protective maternal Ab
- If mother gets infection before 5 days to after 2 days of delivery: Maternal Ab would not have produced in such a short time. This leads to dissemination of virus in the baby to cause neonatal varicella (a severe form of chickenpox).
Epidemiology
Chickenpox is a highly contagious disease.
- Period of infectivity: 2 days before the onset of rash to 5 days after thereafter, until the vesicles are crusted.
- One attack gives lifelong immunity
- Reservoir: Humans are the only known reservoir hosts.
- Source of infection: Patients are the only source, there are no carriers.
- Secondary attack rate is about 70–90%.
Zoster or Shingles
Zoster usually occurs due to reactivation of latent VZV in old age (> 60 year age), in ↓ immunity or rarely in healthy adults.
- Rashes: There are unilateral and segmental, confined to the area of skin supplied by the affected nerves.
- Complications
- Post-herpetic neuralgia (pain at local site): MC complication in elderly patients.
- Zoster ophthalmicus: Unilateral painful crops of skin rashes surrounding the eye.
- Ramsay Hunt syndrome develops when geniculate ganglion of facial nerve is involved.
It is characterized by tetrad of facial nerve palsy plus vesicle on tympanic membrane,external auditory meatus and the tongue.
Vaccine
- Live attenuated vaccine using Oka strain of VZV is available.
It is given to children after 1 year of age; 2 doses, first dose is given at 12–15 months and second dose at 4–6 yrs.
Treatment
Acyclovir, famciclovir or valacyclovir are the antiviral agents of choice. They can prevent the complications of chickenpox and can also halt the progression of zoster in adults, but cannot prevent post-herpetic neuralgia.
- VZIG (Varicella zoster immunoglobulin)
- It is recommended for postexposure prophylaxis. It is given within 96 hrs (preferably within 72 hrs) of exposure.
- It is also indicated for neonates born to mothers suffering from chickenpox if the onset of chickenpox in the mother is between < 5 days before delivery till 48 hrs after delivery.
VZIG not indicated if the mother has zoster.
Infection Control Measures
- Patients infected with VZV should be kept in isolation.
- Airborne precautions (for example., negative air-flow rooms) plus contact precautions must be followed until lesions are dry and crusted. For localized zoster in an immunocompetent host, contact precaution alone can be followed.
Cytomegalovirus (Cmv)
CMV is the largest virus in Herpesviridae family. It is so named because it causes massive enlargement of infected host cells.
- Host specificity: CMV are strictly species-specific.
- Cell type specificity: CMV infects kidney and salivary glands.
- Cell–to–cell spread: CMV is almost always closely associated with the cells and spread primarily cell-to-cell, so that very little virus may be cell-free.
Clinical Manifestations
Congenital CMV Infection
CMV is probably the MC intrauterine infection associated with congenital defects, affecting near 1% of infants born.
- Cytomegalic inclusion disease develops in about 5% of the infected fetus. The remaining are although asymptomatic at birth, 5–25% of them may develop significant psychomotor,hearing, ocular, or dental defects within 2 years.
- Congenital defects include:
- MC defects are petechiae, hepatosplenomegaly, and jaundice.
- Less common: Microcephaly, cerebral calcifications, IUGR, and prematurity.
- Risk is maximum if the infection occurs in early pregnancy and if the mother is primarily infected during pregnancy.
Perinatal CMV Infection
- Transmission to newborn occurs during (1) Delivery, (2) Postnatal—through infected breast
- Mostly asymptomatic, but shed virus in urine up to several years.
- Few infants, especially premature babies develop interstitial pneumonitis.
Immunocompetent Adults
Mononucleosis-like syndrome develops in healthy adults following blood transfusion.
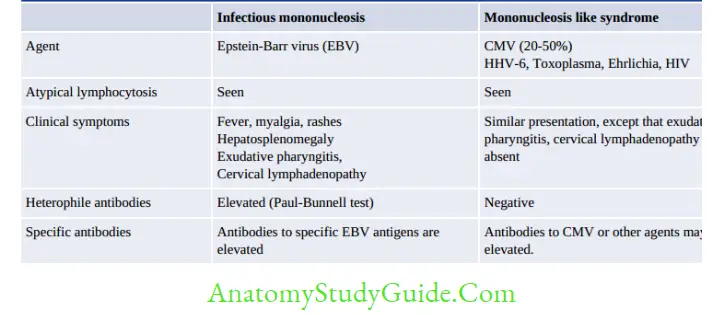
In the Immunocompromised Host
CMV produces severe infection in immunosuppressed individuals; due to reactivation of latent CMV viruses.
In untreated AIDS patients with CD4 T-cell count < 50/µl—CMV may cause Chorioretinitis (MC presentation), gastroenteritis and dementia.
Organ transplant recipients: CMV is probably the MC viral infection in transplant recipients.
- CMV infection occurs usually between 1 to 4 months following transplantation.
- Bilateral interstitial pneumonia in bone marrow transplant recipients.
Epidemiology
- Transmission: In contrast to HSV, CMV transmission requires close contact
- Oral and respiratory contact is the predominant mode
- Others—Transplacental, blood transfusion (risk is 0.1–10%), and sexual
- Reservoir: Humans are the only known host for CMV.
- Prevalence: In underdeveloped nations, 90% of people being seropositive in contrast to 40–70% in developed nations.
Laboratory Diagnosis
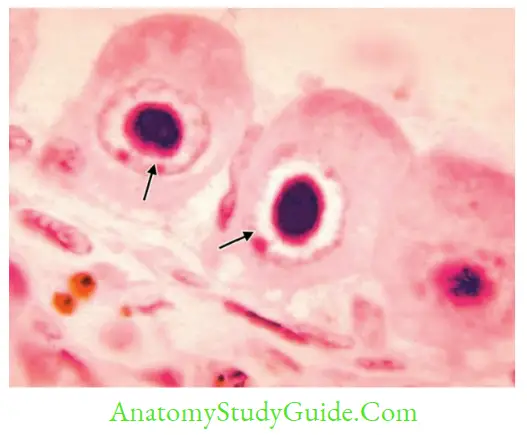
- Detection of inclusion bodies in urine: CMV produces both perinuclear cytoplasmic and intranuclear inclusions (describe as Owl’s eye appearance)
- Virus Isolation: CMV can be isolated from throat washings and urine.
- Human fibroblasts are the most ideal cell lines, growth occurs in 2–3 weeks.
- Shell vial technique: Used to detect growth in 4–5 days.
- Antibody detection:
- IgM antibodies are indicative of active infection.
- Four-fold rise of IgG indicates recurrent infection.
- Antibodies are often undetectable in immunocompromised patients.
- Antigen detection: CMV-specific pp65 antigens. It is highly specific and reliable method
- PCR and real-time PCR targeting UL54, UL55 and UL83 genes detection in blood or body fluids such as CSF.
Treatment
CMV does not respond to acyclovir.
- Ganciclovir is the DOC for cytomegalic inclusion disease or retinitis or transplant infections.
- Others: Valganciclovir (given orally), foscarnet (DOC in ganciclovir-resistant cases), cidofovir and CMV Ig.
- Epstein-Barr Virus
Pathogenesis
EBV is transmitted by oropharyngeal contact through infected salivary secretions
- Binds to EBV receptors: Complement receptors (CD21 or CR2) on B-cell and pharyngeal epithelial cells.
- Primary infection occurs in the oropharynx. EBV replicates in epithelial cells or Blymphocytes of the pharynx and salivary glands.
- Inside B-cells, EBV directly enters into latent phase.
- Pathogenesis in children, developing infectious mononucleosis:
- Infected B-cells become immortalized by the virus and synthesize large number of
variety of immunoglobulins (polyclonal), many of those are autoantibodies - In response to this, the bystander CD8 T-lymphocytes are stimulated and appear atypical.
- Infected B-cells become immortalized by the virus and synthesize large number of
- Pathogenesis in people developing EBV-induced cancers (Mechanism of oncogenesis):
EBV can induce malignant transformation of infected B-cells and epithelial cells by expressing latent EBV antigens such as LMP and EBNA. - LMP-1 (latent membrane protein-1) is the most important viral oncogene.
- Viral EBNA-2 (EBV nuclear antigen-2) activates host cell cyclin-D, thus promotes cell proliferation.
Clinical Manifestations
Infectious Mononucleosis
It is also called as kissing disease (salivary contact) or glandular disease
- Age-Young adults of developed countries are usually affected.
- It is characterized by:
- Headache, fever, malaise and Exudative pharyngitis
- Cervical lymphadenopathy and Hepatosplenomegaly
- Rashes following ampicillin therapy
- Atypical lymphocytosis (CD8 T-cells)
- Autoantibodies reactive to sheep RBC antigens (detected by Paul-Bunnell test).
- EBV Associated Malignancies
EBV is associated with several malignancies: - Burkitt’s lymphoma (tumor of the jaw seen in children and young adults): EBV is associated with 90% of African and 20% of non-African cases of Burkitt’s lymphoma.
- Most of the cases have pre-existing mutation [t(8;14)] that in turn activates the growth-promoting MYC oncogene
- Falciparum malaria may impair host CMI and stimulates the EBV-infected B-cells
- Nasopharyngeal carcinoma: Seen among Chinese having h/o intake of salted fish (nitrosamine) and herbal snuff (phorbol ester)
- Hodgkin’s lymphoma (especially the mixed-cellularity type).
- NHL (Non-Hodgkin’s lymphoma): All central nervous system non-Hodgkin’s lymphomas and 50% of systemic non-Hodgkin’s lymphomas are EBV positive.
Other Conditions Associated with EBV
- Lymphoproliferative disorder such as Duncan syndrome, an X-linked recessive disease affecting young boys.
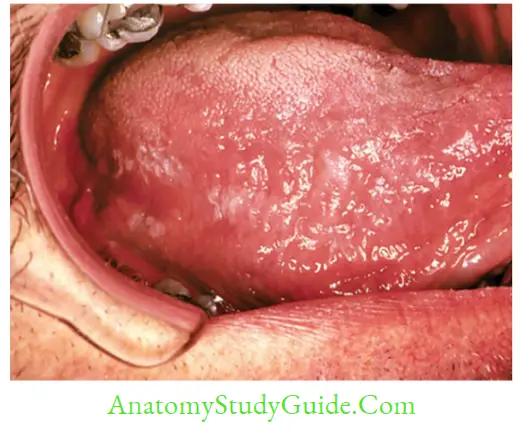
- Hairy cell leukoplakia: Wart-like growth of epithelial cells of the tongue developed in some HIV-infected patients and transplant recipients
- Chronic fatigue syndrome
Laboratory Diagnosis
Heterophile Antibody Detection by Paul-Bunnell Test
- It is a heterophile agglutination test that uses sheep RBCs to detect heterophile antibodies in patient’s serum
- Differential absorption test and Monospot test are done for confirmation.
EBV-Specific Antibody Detection
- Antibody to viral capsid antigen (VCA):
- IgM type: It indicates current infection.
- IgG type: It is a marker of past infection and indicates immunity.
- Antibodies to early antigen also indicate current viral infection.
- EA-D antibody (antibody to early antigen that occurs in diffuse pattern in nucleus and cytoplasm of the infected cells): It is elevated in acute infection and Burkitt’s lymphoma
- EA-R antibody, antibody to early antigen restricted to the cytoplasm: It is elevated in nasopharyngeal carcinoma
- Antibodies to EBNA (EBV nuclear antigen) reveal past infection, but four fold rise of titer suggest current infection.
Treatment
- Acyclovir is useful in the treatment of oral hairy leukoplakia, but not effective for infectious mononucleosis and other m alignancies.
- Antibody to CD20 (rituximab) has been effective in some cases.
Human Herpesvirus-6
HHV-6 infects the T-cells by binding to CD46 receptor. It has two variants 6A and 6B.
- Sixth disease: In children, HHV-6 (usually the 6B variant) causes sixth disease, also called as exanthema subitum or roseola infantum.
- In older age groups, HHV-6 has been associated with mononucleosis-like syndrome.
Human Herpesvirus-8
HHV-8 is also called as Kaposi’s sarcoma-associated herpesvirus (KSHV)
- Epidemiology
- In high prevalence area: HHV-8 is endemic in Africa where it is transmitted by oral secretion.
- In low-prevalence areas such as North America, Asia, northern Europe, it affects homosexual
- Less common mode: Organ transplantation, IV drug abuse, and blood transfusion
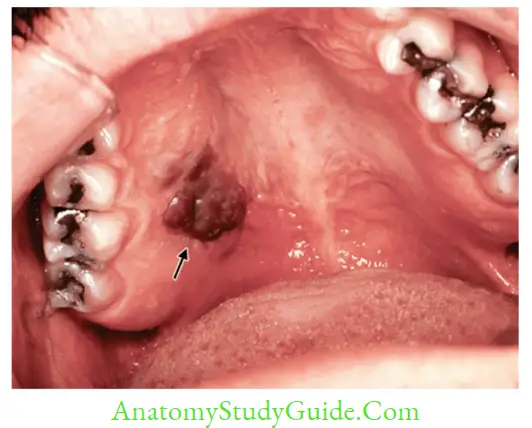
- Manifestations: In immunocompromised individuals (for example., HIV), HHV-8 causes:
- Kaposi sarcoma
- Primary effusion lymphoma (body cavity-based lymphomas)
- Castleman’s disease (lymphoproliferative disorder of B-cells)
- However, in immunocompetent host, HHV-8 produces fever and rash
- Treatment: HHV-8 infections respond well to foscarnet, ganciclovir, and cidofovir
Other DNA Viruses
Parvoviruses
- Parvoviruses are the smallest viruses (18–26 nm size).
- Nonenveloped with icosahedral symmetry
- Possess linear single-stranded DNA, (the only DNA virus to have ssDNA).
- Transmission: Parvovirus B19 exclusively infects humans, most commonly by the respiratory route, followed by blood transfusion and transplacental transmission (occurs in 30% of cases with maximum risk is in the second trimester).
- Tropism for RBCs: It infects RBC precursors by using P blood group Ag as receptor.
- Genotyping: Parvovirus B19 has three genotypes but single serotype. Genotype 1 is the MC in world and genotype 3 is MC in western Africa.
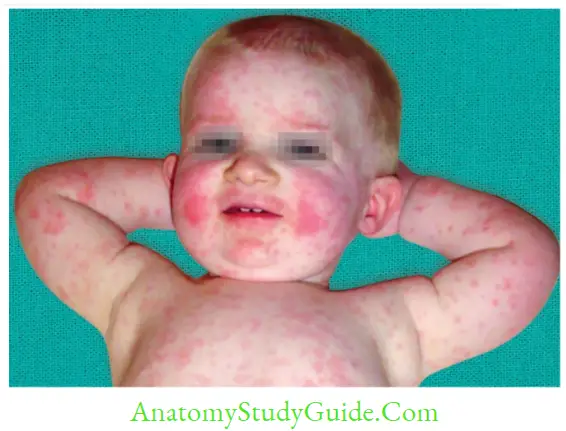
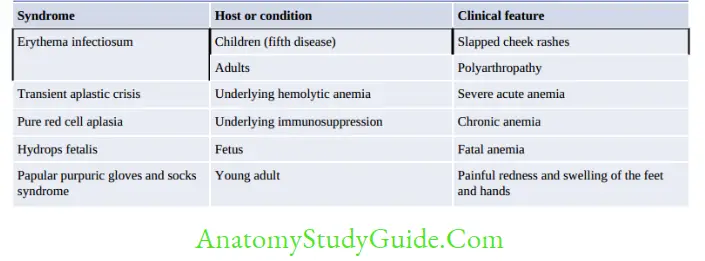
Papillomaviridae And Polyomaviridae
The formerly known Papovaviridae family are currently separated into two different families
- Family Papillomaviridae has 16 genera, out of which Human papillomavirus infects man.
- Family Polyomaviridae has several genera infecting animals. Human infections are associated with:
- JC virus causes Progressive Multifocal Leukoencephalopathy (PML)
- BK virus causes nephropathy in transplant recipients. It differs from JC virus, by its ability to grow in a wide range of cell lines and is less oncogenic.
- Merkel cell virus causes Merkel cell carcinoma of skin
- SV40 virus (Simian vacuolating 40 virus) is nonpathogen to man.
- Human Papillomavirus (HPV)
- HPV has selective tropism for epithelium of skin and mucous membranes and produces an array of infections.
Products of early genes E6 and E7 have oncogenic potential by following ways: - E6 protein facilitates the degradation of the p53 tumor-suppressor protein
- E7 protein binds to the retinoblastoma gene product and related proteins.
Pathogenesis
HPV has tropism for skin (squamous epithelium) and mucous membranes and produce various benign and malignant lesions
Benign warts
- Common warts (verruca vulgaris) and flat warts (verruca plana) in children.
- Plantar warts (verruca plantaris) in young adults
- Anogenital warts (condyloma acuminatum) seen among adults.
- Epidermodysplasia verruciformis:
- Rare autosomal recessive benign condition
- Rarely progresses to squamous cell malignancy (seen with HPV serotypes 5 and 8)
- Affects the sun-exposed areas.
- Cervix lesions
- CIN (Cervical Intraepithelial Neoplasia) is a benign condition, associated with low-risk
HPV types 6 and 11 - Carcinoma cervix (squamous cell) is associated with high-risk HPV types such as 16 and 18 (most common); followed by 31, 33, 35, 39, 45, 51–53, 56, 58, 59, 66, 68, 73 and 82.
- High-risk serotypes are associated with squamous cell carcinoma involving other genital regions such as penis, anus, vagina, and vulva.
- Head and neck lesions
- Benign: Recurrent laryngeal papillomas in children are associated with low-risk serotypes 6 and 11.
- Malignant: Laryngeal and esophageal carcinomas (associated with high-risk serotypes 16 and 18).
- Pityriasis versicolor–like lesions
- HPV Vaccine
- HPV vaccine is recommended to adolescent and young adult females.
- Subunit vaccine consists of virus-like particles composed of HPV L1 proteins which are produced in yeast by DNA recombinant technology
- Both nine valent and bivalent vaccines are licensed
- Nine valent vaccine (Gardasil 9, Merck): Includes seven common cancer-causing serotypes (16, 18, 31, 33, 45, 52 and 58) and two noncancer-causing serotypes (6 and 11), given IM;either as 2 doses (6 months gap) between 9–14 years or 3 doses (0, 2 and 6 months) between 14–26 years age.
- Its earlier version was a quadrivalent vaccine which included type 6, 11, 16 and 18.
- Bivalent vaccine (Cervarix, GSK) includes only the high-risk serotypes 16 and 18. It is given as single dose, IM.
Barrier methods of contraception can block sexual transmission thus prevent anogenital
HPV infections.
Poxviridae
Poxviruses are the largest (400 nm) viruses- large enough to be seen under light microscope.
- Most complex symmetry.
- Brick-shaped or ellipsoid
- Nucleocapsid consists of: Biconcave dumbbell-shaped DNA core.
- It is the only DNA virus that replicates in the cytoplasm
Important members include: Variola, Vaccinia, Molluscum contageosum.
Smallpox (Variola)
Smallpox, a highly contagious severe exanthematus (rashes) disease, was the first disease to be eradicated from the world.
Timeline
- Last natural case of variola major was seen in a Bangladeshi women in Assam in May 1975
- Last natural case of variola minor was seen in Merca, Somalia, 26th October 1977
- Eradication was declared by WHO nearly after three years, i.e. on 8th May 1980
- Agent of bioterrorism: As vaccination was stopped following eradication people borne after 1980 are not immunized. Hence smallpox virus can be a potential agent of bioterrorism.
Reasons that Made Eradication Successful
- Variola was an exclusively human pathogen, no animal reservoir
- Source: Patients were the only source, there was no carrier state
- Case detection was easy due to characteristic appearance of rashes
- Subclinical disease were not transmitting the disease
- Global smallpox eradication programme
- Highly affective live vaccinia vaccine:
- Freeze-dried form was used (↑ stability)
- Multiple puncture technique was followed to administer the vaccine by using abifurcated
needle, which was simple, effective and economical.
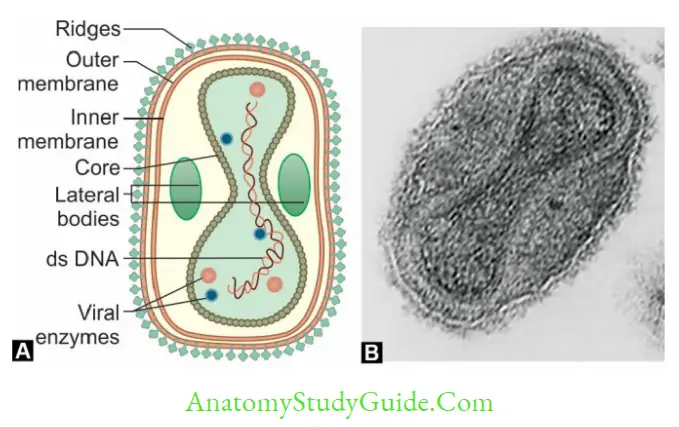
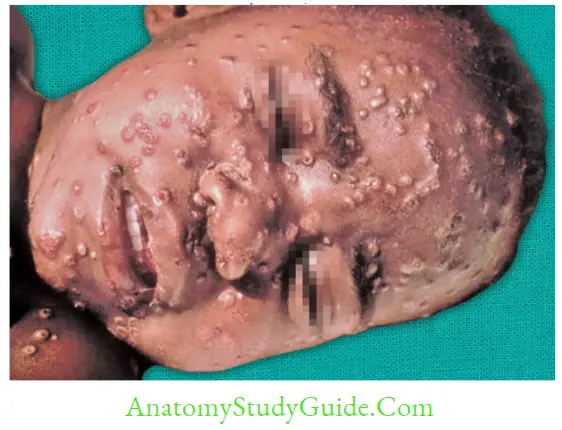

Vaccination
- Live vaccinia vaccine was highly effective.
- It was given as single dose between 1-2 years of age.
- As un-attenuated live virus was used, adverse reactions were common.
- Cowpox vaccine discovered by Edward Jenner (the father of vaccination)
Variolation (Healthy people were inoculated with the skin scraping of a smallpox patient).
Vaccinia
Vaccinia differs from variola by:
- It is nonpathogenic to humans or produces milder skin lesions.
- Produces an inclusion body called as Guarnieri body (variola produces Paschen body)
- On CAM vaccinia virus produces larger and hemorrhagic and necrotic pock lesions.
- Ceiling temperature is the highest temperature beyond which the pock formation is inhibited on CAM. It is higher for vaccinia virus (41 °C) than variola virus (38 °C).
- Vaccinia but not variola can produce plaques on chick embryo tissue cultures.
Molluscum Contagiosum Virus
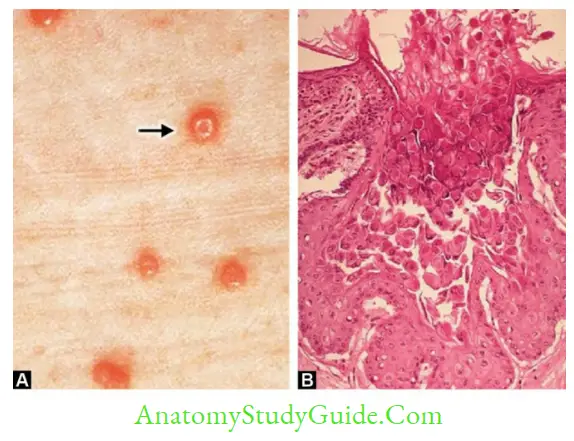
- Lesions: It produces pink pearly wart-like lesions with a characteristic dimple at the center (umbilicated).
- Lack of associated inflammation and necrosis
- Lesion are found anywhere on the body except on the palms and soles. Genital lesions are seen in adults.
- Transmission:
- Children (MC): Spread by direct and indirect contact.
- Rarely sexual transmission has been reported in young adults.
- Laboratory diagnosis:
- Molluscum bodies are the intracytoplasmic eosinophilic inclusions seen in skin scrapings (histopathological stains)
- Not cultivable: It cannot be propagated in tissue culture, egg or in animals.
- Treatment: Surgical removal of the lesions by ablation.
- Prognosis: Self-limiting, except in HIV.
Adenoviridae
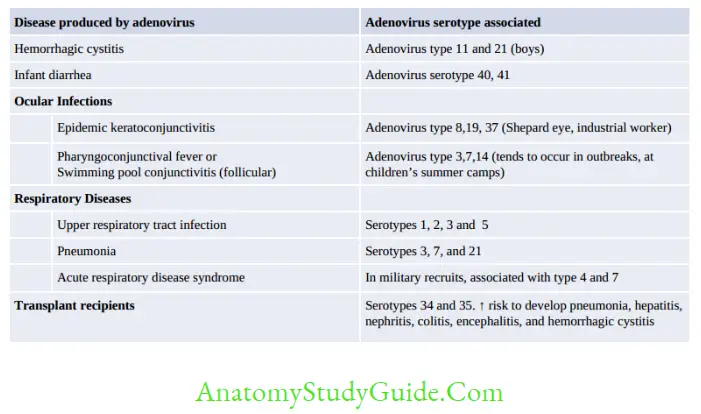
- It is nonenveloped DNA virus, space vehicle shaped
Bacteriophages
Bacteriophages are viruses that attack bacteria
- Bacteriophages are typically tadpole-shaped possessing a hexagonal head and a tail attached with tail fibers.
- Hexagonal head contains tightly coiled dsDNA, enclosed by capsid (protein coat)
Altered morphology may be seen in some phages: - Shape: Spherical or filamentous instead of hexagonal.
- Nucleic acid: May contain ssDNA or RNA instead of dsDNA.
Life Cycle of Bacteriophage
Based on two types of life cycle bacteriophages are classified into: Lytic and lysogenic or temperate phage
- Lytic phase: Phage replicates in the cytoplasm and lyses the host bacterium to come out. It resembles the replication of other DNA viruses; except that:
- In penetration step: Phages are attached to bacterial cell wall as ‘ghosts’.
- There is no uncoating step as seen with other viruses.
- Release of the daughter phages occur by lysis of the host bacterium.
- Duration of Eclipse phase is about 15 to 30 minutes; in contrast to 15-30 hours for most of the animal viruses.
- Lysogenic or Temperate phage: Phage DNA is incorporated within host DNA and remains dormant as prophage.
Lysogenic to lytic interconversion: When the temperate phages want to come out, they get excised from bacterial chromosome, then transform to lytic phages, multiply in the cytoplasm and are released by lysis.
Uses of Bacteriophage
- Phage typing: Phage typing is employed for typing the following bacteria:
- Staphylococcus aureus
- Vi antigen typing of Salmonella Typhi,
- Vibrio cholerae (Basu Mukherjee phage typing)
- Brucella (Tbilisi phage typing)
- Corynebacterium diphtheriae
- Phage assay: To estimate the no. of viable phages in preparations.
- Used in treatment (Phage therapy): Lytic phages can kill the bacteria, hence may be used for treatment of bacterial infection, such as post-burn and wound infections.
- Used in diagnosis: Mycobacteriophages are used for the identification of M. tuberculosis.
- Used as a cloning vector.
- Transduction: In S.aureus, the plasmids coding for β-lactamases are transferred between the strains by transduction.
- Codes for toxins: The phage genomes code for the following bacterial toxins
- A, and C of Streptococcal pyrogenic toxin
- Botulinum toxin C, D
- Cholera toxin
- Diphtheria toxin
- EHEC (Enterohemorrhagic E.coli) (Verocytotoin)
- Alter antigenic property of bacteria: for example., in Salmonella.
Leave a Reply