Radiation Protection Essay Questions
Question 1. Describe in detail the basics of patient protection from X-ray exposure.
(or)
Mention the key rules to be followed while taking radiographs to reduce patient exposure.
Answer: Radiation protection measures should be followed before, during, and after dental X-ray exposure to reduce the adverse effects of radiation on a dental patient.
Table of Contents
Patient Protection Before Exposure:
1. Prescribing dental radiographs:
- Radio-graphic selection criteria (or) high yield (or) referral criteria states that diagnos¬tic radiographs should be advised after examining the patient clinically and confirming that the radiographic information is essential to substantiate the diagnosis, treatment, and prognosis.
- Professional judgment should be used to decide the type, number, and frequency of dental radiographs.
Read And Learn More: Oral Medicine and Radiology Question And Answers
2. Proper equipment:
Filtration: The X-ray beam is polychromatic containing both high and low-energy X-ray photons. The low-energy X-ray photons have less penetrating power and are absorbed by the patient tissue rather than carrying diagnostic information to the film. Thus low energy photons increase the patient’s exposure dose. With the use of filters, these low-energy X-ray photons are removed from reaching the patient.
- Inherent filtration: Occurs when the primary beam travels through the insulating oil, the tube head seal, and the glass window.
- Added filtration: The aluminum disc placed between the collimator and the tube head seal filters the X-ray beam.
X-ray machine requires a 1.5 mm thickness of aluminum disk when it operates at or below 70 kVp and a 2.5 mm thick disk when operates above 70 kVp. - Total filtration (Inherent and added filtration) Collimation: Collimation reduces the size of the X-ray beam so that the area of tissue exposed to the primary X-ray beam is minimal to fulfill the diagnostic requirements.
- The use of collimators should restrict the beam size to a diameter of not more than 2.75 inches or 7 cm when it reaches the patient’s skin for an X-ray machine operating above 50 kV.
- The size reduction improves the image quality by decreasing the scatter radiation and thereby film fog in addition to reducing the patient exposure dose. The use of rectangular collimation results in 71-80% dose reduction.
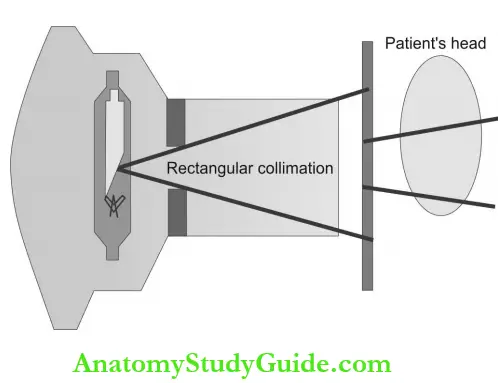
- Position indicating device(PID): PID is used to focus the X-ray beam without deviating from the path so that limiting the occurrence of scatter radiation. Precision instruments and Rinn XCP film-holding devices with rectangular collimation are examples.

Patient Protection During Exposure:
- Thyroid collar: Is an adjustable lead safeguard used to wrap around the patient’s neck for preventing the scatter radiation from reaching the thyroid gland.
- Lead apron: Is a pliable lead protector to cover the patient’s chest and abdomen for stopping the scatter radiation from reaching the reproductive and blood-forming organs.
- Fast film: F-speed film or insight and E – speed or ektaspeed film are the fastest intraoral films available.
- Beam alignment devices: Aids in the stabilization of the film intraorally and reduces the chances of slipping thereby reducing the patient’s exposure.
- Exposure factor selection: A setting of 70-90 kVp is ideal for dental X-ray units.
- Appropriate technique: Enhances the quality of images and avoids retakes.
Patient Protection After Exposure:
- Proper film handling: Artifacts caused by improper handling result in a nondiagnostic image which must be retaken and exposes patients to radiation.
- Proper film processing: Film processing is a step to convert the latent image to a visible image.
Question 2. Discuss operator protection in dental radiography. (or)
Discuss personal protection in dental radiography.
Answer: The application of standard operator protection principles can minimize the radiation dose received by a dental radiographer.
- Protection guidelines: Provide guidelines to the dental radiographer with basic safety information. It includes the following:
- Distance recommendations: Radiographer must stand at least 6 feet away from the X-ray tube head during exposure. If this distance is not possible, a protective barrier must be used.
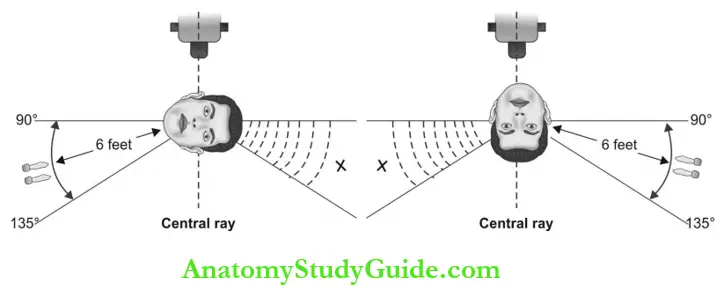
- Position recommendation: To avoid the primary beam, the radiographer should stand perpendicular to the primary X-ray beam, or at 90°-135° angle to the beam.
- Also, the dental radiographer should:
- Not keep the film in place during expo¬sure.
- Do not hold the tube head during exposure.
- Also, the dental radiographer should:
- Shielding recommendations: A protective barrier that can absorb the primary beam will protect the operator from primary and scatter radiation. Dental radiographers should stand behind the protective lead barrier or drywall during exposure.
- Radiation monitoring: Radiation moni¬toring can identify excessive occupational exposure.
- Equipment monitoring: Dental X-ray machine should be examined for any radiation leak. Any radiation other than the primary beam emitted from the tube head is known as leakage radiation. Leakage radiation should be monitored by using a film device that can be obtained through the state health sector or from dental X-ray machine manufacturers.
- Personal monitoring: The amount of radiation received by the operator is monitored by a “film badge” or radiation monitoring badge. The film badge holds an X-ray film segment or radiosensitive crystal within a plastic case.
- This should be clasped at the waist level of the operator while taking the radiographs. When the badges are not worn, they should be stored in a radiation-safe area.
- The badges should be submitted to the radiation monitoring authorities in the scheduled period (for example once in 3 months or semiannually) to detect the amount of radiation exposure.
Question 3. Discuss radiation exposure guidelines.
Answer:
Radiation exposure guidelines have been established to safeguard radiation professionals and patients. The guiding strategies include radiation safety legislation and exposure limits for the public and occupationally exposed personnel.
Radiation safety legislation: Has been established to protect the patient, radiogra¬phers, and public from the harmful effects of radiation.
These include:
- Radiation Control for Health and Safety Act: To standardize the operation of equip¬ment.
- The Federal Consumer-Patient Radiation Health and Safety Act: This rule is responsible for the education and official recognition of professionals operating radiographic equipment.
- Maximum permissible Dose (MPD): It is defined as the maximum dose equivalent that a body is permitted to receive within a specific period. MPD is the radiation dose that can be tolerated by the body with minimal or no damage.
- As per NCRP guidelines, the MPD for radiology professionals is 5 rem/year, and for nonoccupational individuals, the MPD is 0.1 rem/year.
- Maximum accumulated dose (MAD): This states that radiology workers must not exceed an accumulated lifetime radiation dose.
- MAD is calculated using a formula based on the person’s age.
- MAD = (N – 18) x 5 rems/year N = Person’s age in years.
18 = Refers to the minimum age of a person permitted to work with radiation. - ALARA Concept: ALARA = As low as reasonably achievable concept states that all exposure to radiation must be kept to a minimum.
All possible measures need to be taken in radio diagnostic centers to reduce the adverse effects of radiation.
Radiation Protection Short Notes
Question 1. What is the ALARA concept?
Answer:
- As low as reasonably achievable concept declares that all exposure to radiation must be minimum.
- ALARA concept: Every probable method of minimizing the radiation dose should be employed to avoid radiation-induced hazards. Strict adherence to this principle will protect both patients and operators.
- This concept is not specifically mentioning any radiation dose as a reasonable amount.
Question 2. Discuss different types of filtration.
Answer: The use of filtration selectively removes soft, low-energy, long-wavelength X-ray photons from the primary beam and permits photons with sufficient energy to carry diagnostic information to the film.
In dental X-ray machines, two types of filtration are used:
- Inherent filtration: Occurs when the primary beam travels through the insulating oil, tube head, and glass window. Inherent filtration of the dental X-ray machine is approximately equal to the filtering effect of 0.5 to 1 mm of aluminum.
- Added filtration: This takes place when the X-ray beam travels through an aluminum disk placed between the collimator and tube head. 1.5 mm aluminum filters are used in dental X-ray machines operating at or below 70 kVp and 2.5 mm aluminium is required when above 70 kVp is used.
- The use of rare earth elements like samarium, erbium, etc. in combination with aluminum filtration reduces overall patient exposure by 20-80%.
- Total filtration: Inherent plus added filtration. The X-ray machine operating at 70 kVp requires a minimum total of 1.5 mm aluminum filtration and the machine operating above 70 kVp requires a minimum total of 2.5 mm aluminum filtration.
Question 3. Describe collimator.
(or)
What is collimation?
Answer:
- Collimation is the process of reducing the X-ray beam size and shape before reaching the patient’s skin to reduce the exposure dose. The collimator is an apparatus that restricts the size and shape of the X-ray beam as it leaves the tube head.
- These devices are made up of a lead diaphragm with a circular aperture.
- Collimation Principle: The amount of scatter radiation produced is proportional to the area exposed.
Purpose of Collimation:
- Significant reduction in patient exposure
- Decreased amount of scatter radiation reduces film fog and increases image quality
- A decrease in beam size reduces penumbra and increases image sharpness.
- For intraoral radiographs, the beam size is reduced to match with film size. The beam is collimated to a circle having a diameter of 7 cm at the patient’s skin surface when the tube is operating above 50 kVp.
Types of Collimators:
- The round position indicating the device
- The rectangular position indicating device
- Use of rectangular collimation results in 71-80% dose reduction
- Film holders with rectangular collimators and round position indicating device (PID)
- A precision instrument with rectangular collimation
- XCP with rectangular collimation.
Question 4. Define the half-value layer.
Answer:
- Half-value layer (HVL) is the thickness of the specified material required to reduce the beam intensity by half when placed on the path of the X-ray beam.
- Aluminum filters are used to remove the low energy, less penetrating, long wavelength X-ray photons and increase the mean penetrating quality of the beam by reducing its intensity. HVL determines the penetrating ability of the beam.
- For example, if a dental X-ray beam has a half-value layer of 2 mm, it requires 2 mm thickness of aluminum to reduce its intensity by half (50%).
- Measurement of HVL requires a dosimeter. The HVL should be at least 1.5 mm aluminum at 70 kVp and 2.5 mm aluminum at 90 kVp.
Question 5. What is a pocket dosimeter?
Answer:
- A pocket dosimeter is a device used to check the quantity of X-ray beams to verify whether the machine output is changed over time.
- The number of X-ray photons is determined by the mA and exposure time. So, to determine the machine output, the exposure parameters need to be standardized, for example, 0.25 seconds, 7 or 10 mA, and 65 or 70 kVp, and the quantity of radiation is measured using a pocket dosimeter.
- For this setup, the baseline reading is always 180 milliroentgen.
- When a new reading is taken to check the machine output it should be the same as the baseline value, then no further testing of beam quantity is necessary.
Question 6. Describe the source to the film distance concept.
(or)
Describe the effect of the focal spot to film distance in exposure dose.
Answer:
- Film distance concept Principle: Extended radiation source—patient distance (focal spot to film distance) will reduce the amount of radiation to the patient.
- Film distance concept Inverse square law: States that the beam intensity is inversely proportional to the square of the Source to film distance (SFD).
- The distance between the focal spot and the film should be as great as is technically acceptable.
- Two standard focal spot-to-film distances (FSFDs) used in intraoral radiography are 20 cm (8 inches) and 41 cm (16 inches).
- When an X-ray tube operates above 50 kVp, the X-ray source-skin distance should not be less than 18 cm.
- Film distance concept Application: The use of longer FSFD (or) SFD results in a 32% dose reduction in exposed tissue volume. This is because at a great distance, the beam is less divergent. Smaller focal spot size thereby increases the radiographic resolution.
Question 7. Source of radiation exposure in daily life.
Answer:
Radiation from a natural source is composed of radon, cosmic radiation, terrestrial radiation, and internal radiation. The decay process of natural radon produces radon gas which is taken into the lungs. It remains as same until it undergoes a subsequent decay process and in this way leads to chronic radiation exposure.
- Cosmic radiation: Originates in outer space. Altitude, latitude, and solar activity modify the cosmic rays reaching Earth.
- Terrestrial radiation: Originates from soil nuclides of radium, uranium, thorium, and their decay products. The internal source of radiation is dependent on inhalation and ingestion of radionuclides.
Question 8. Describe radiation risk estimation for dental radiography.
Answer:
Risk estimates can be explained as two types:
1. Absolute risk: It is defined as the difference between risk in an irradiated population compared to that in a normal population. Absolute risk is calculated as a probability for a cancer-free person to develop cancer after getting exposure to a risk factor.
2. Relative risk (r): It is the ratio of the risks in irradiated and nonirradiated populations.
When r is:
- ≤1, there is no cancer risk after exposure.
- ≥1, there is increased cancer risk after exposure.
- In dental radiology, risk estimation is measured by absolute risk.
Question 9. Discuss patient education regarding radiation protection.
Answer:
- The dental radiographer should explain how patients are protected from radiation exposure during the entire procedure:
- Before getting started the procedure, all possible protective measures were taken to reduce unnecessary exposure.
- The X-ray equipment we use is frequently tested for its integrity to follow the safety guidelines.
- During X-ray exposure, we use a thyroid collar and a lead apron to protect your body from X-ray radiation.
- We use the fastest film available.
- We use effective techniques to avoid making mistakes that require re-exposure.
Radiation Protection Viva Voce
Question 1. What is the deterministic effect?
Answer:
- Any somatic effect that increases in severity in direct proportion to radiation dose after reaching the threshold limit is defined as a deterministic effect.
- These effects occur soon after or months to a year later from relatively large exposure. Examples: Skin or mucosal erythema, cataracts, fibrosis, abnormal growth and development following uterine exposure.
Question 2. What is the stochastic effect?
Answer: The probability of radiation effects and not its severity is dose-dependent. There is no threshold limit below which cancer will not occur. The probability for developing cancer increases as the exposure increases.
Question 3. What is MP
Answer: Maximum permissible dose is the highest amount of radiation approved to receive by an individual in a specific period.
Question 4. What is filtration?
Answer:
- X-rays are polychromatic beams containing both low and high-energy photons, but only photons having energies between 35 and 55 keV are more efficient in producing diagnostic images.
- Filtration is the process by which selective removal of both low and high-energy photons from the beam thereby allowing only photons with sufficient penetrating energy to reach the patient. Thus the use of a filter reduces the patient’s exposure dose.
Question 5. Name the filter material used in the dental X-ray machine.
Answer:
- About 1.5 mm thick aluminum is commonly used as a filter in dental radiographic machines operating at or below 70 kVp, whereas 2.3 mm aluminum is used when above 70 kVp is used.
- Selective filtration: Rare earth elements like samarium, erbium, niobium, gadolinium, terbium-activated gadolinium oxysulfide, and thulium-activated lanthanum oxy bromide are used with aluminum to further reduce the patient exposure by selectively removing both extremely low and high energy photons.
- The use of rare earth filters increases the exposure time (and hence increases the X-ray machine workload. and reduces the image quality by decreasing contrast, sharpness, and resolution).
Question 6. What are the benefits of using a collimator?
Answer:
- Significant reduction in patient exposure
- Decreased amount of scatter radiation reduces film fog and increases image quality
- The decrease in beam size reduces penu¬mbra and increases image sharpness.
Question 7. What is the distance-position rule?
Answer:
- The radiographer should stand 6 feet away from the tube head at an angle of 90-135 ° to the primary beam direction during film exposure.
- This rule will protect the dental radiographer from occupational radiation exposure by avoiding the primary beam from reaching him.
Question 8. What is ALARA stands for?
Answer: As low as reasonably achievable.
Question 9. What is the function of NCRP?
Answer: National Council on Radiation Protection and Measurement: Identifies the adverse effects of radiation and the risk associated with its use.
Question 10. What is the role of ICRP?
Answer: International Commission on Radiology Protection: Establishes the guidelines to restrict the radiation dose received by Public and occupationally exposed individuals.
Radiation Protection Highlights
- Radiation protection describes all measures that need to be applied in radiology centers to protect patients from the harmful effects of radiation without compromising the quality of diagnostic images.
- The protective measures are applicable both to the patients and the professionals. This chapter deals with radiation safety measures before, during, and after exposure to dental X-rays.
Leave a Reply