Describe the Uterus under the following headings:
- Uterus Introduction
- Uterus Parts and cavities
- Uterus Relations Axis
- Uterus Supports
- Uterus Arterial supply
- Uterus Lymphatic drainage and
- Uterus Applied anatomy.
Answer:
1. Uterus Introduction:
- The uterus is a childbearing thick-walled hollow muscular organ.
- It is situated in the lesser pelvis between the urinary bladder in front and the rectum behind.
2. Uterus Parts:
Read And Learn More: Anatomy Question And Answers
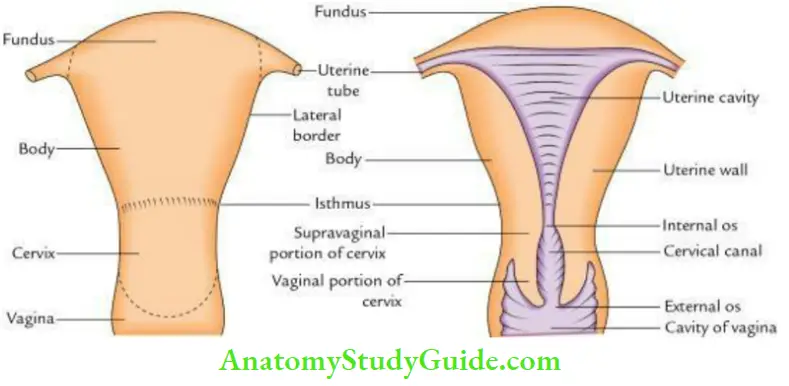
It is piriform in shape (i.e., looks like an upside-down pear) and subdivided into 3 parts.
- Fundus: Upper dome-shaped part above the openings of uterine tubes.
- Body: Part of the uterus, which extends from the fundus to the isthmus. It has a triangular cavity.
- Cervix: Part of the uterus below the isthmus having a spindle-shaped cavity called a cervical canal.
3. Uterus Relations:
- Fundus: Covered by the peritoneum.
- Body:
- The anterior surface is separated from the urinary bladder by a ureterovesical pouch.
- The posterior surface is separated from the rectum by a rectouterine pouch containing the sigmoid colon and coils of the terminal part of the ileum.
- Cervix:
- Supravaginal part:
- Anterior: Urinary bladder
- Posterior: Rectouterine pouch and rectum
- On each side: Ureter and uterine artery
- Vaginal part:
- Anterior: Base of urinary bladder
- Posterior: Rectouterine pouch
- On each side: Ureter crossed by the uterine artery
- Supravaginal part:
Axis: The axis of the uterus is defined by two terms: anteversion and anteflexion.
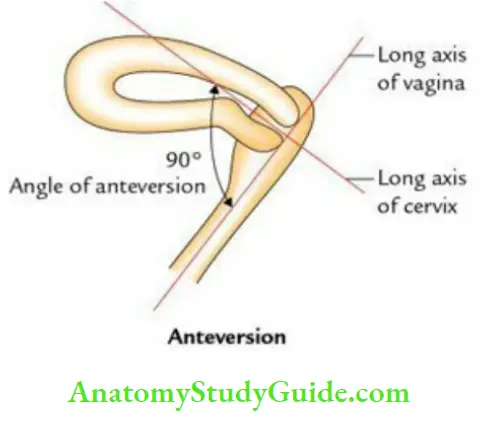
- Anteversion: It is a forward angle between the long axis of the cervix and the long axis of the vagina. It measures about 90°.
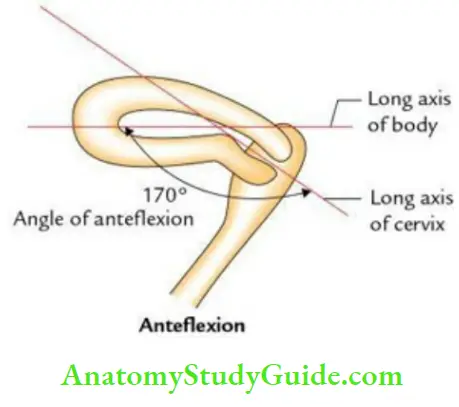
- Anteflexion: It is a forward angle between the long axis of the body and the long axis of the cervix. It measures about 120–170°.
4. Uterus Supports: The uterus undergoes extensive changes in size and shape during the reproductive period of life of the women. It is supported and prevented from sagging down by a number of factors called supports.
The supports are classified into two types: primary and secondary:
1. Primary supports:
- Muscular or active supports:
- Pelvic diaphragm
- Urogenital diaphragm
- Perineal body
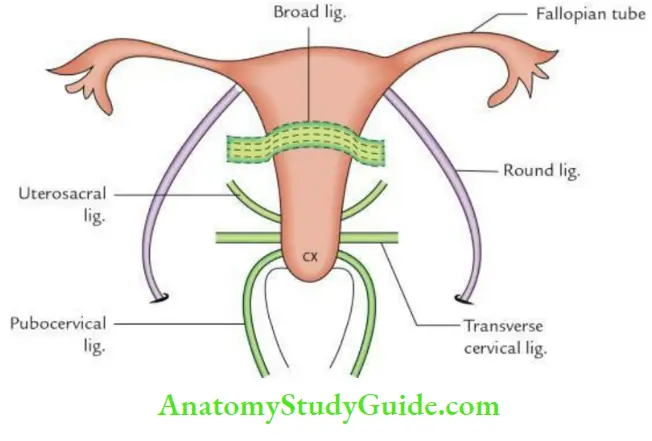
- Ligamentous/fibromuscular/mechanical supports:
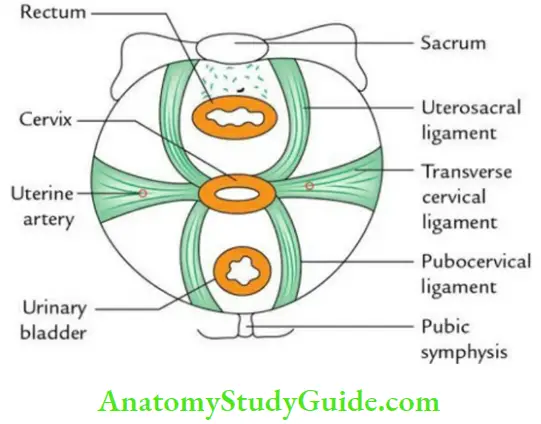
- Transverse cervical ligaments of Mackenrodt (most important)
- Round ligament of uterus
- Uterosacral ligament
- Pubocervical ligament
- Visceral:
- Urinary bladder
- Vagina
- Uterine axis
2. Secondary supports (formed by peritoneal ligaments):
- Broad ligaments
- Uterovesical fold peritoneum
- Rectovaginal fold ofperitoneum
The details of important supports are as follows:
- Pelvic diaphragm: It supports the pelvic viscera and resists any rise in intraabdominal pressure.
- Urogenital diaphragm: It is formed by sphincter urethrae and deep transverse perineal muscles and is enclosed between the superior and inferior fasciae of the urogenital diaphragm.
- Perineal body: It is a fibromuscular node situated in the midline at the center of the perineum. It provides attachment to nine muscles. It acts as an anchor to pelvic diaphragm and maintains the integrity of the pelvic diaphragm.
- Transverse cervical ligaments (Mackenrodt’s ligaments): These are formed by the condensation of the pelvic fascia on each side of the cervix above the levator ani around the uterine vessels. They are fan-shaped and connect the lateral aspects of the cervix and upper part of the vaginal wall to the lateral pelvic wall.
- They keep the cervix in the midline and prevent the downward displacement of the uterus through the vagina.
- Round ligaments of the uterus: These are two 10–12 long, flat fibromuscular bands lying between the two layers of the broad ligament, anteroinferior to the uterine tube. Each ligament begins at the lateral angle of the uterus, runs forward, and laterally, and passes through the deep inguinal ring.
- Uterosacral ligaments: These are the condensation of the pelvic fascia, which connect the cervix to the periosteum of the sacrum and are enclosed within the rectouterine folds of peritoneum.
- Pubocervical ligaments: These are a pair of fibrous bands derived from the pelvic fascia and connect the cervix to the posterior surface of the pubis. They keep the cervix in position by counteracting the pull of uterosacral ligaments.
The ligament of the uterus keeps the uterus in position.
These are: Provide primary support to uterus
- Transerve cervical ligaments
- Round ligaments
- Uterosacral Ligaments
- Pubocervical ligaments
- Broad ligaments – Provide secondary support to the uterus
The first four ligaments are described on P. 180 while the last ligaments (i.e. broad ligaments) are described on Pp. 182–183.
5. Uterus Arterial supply:
- Chiefly by the uterine arteries
- Partly by the ovarian arteries
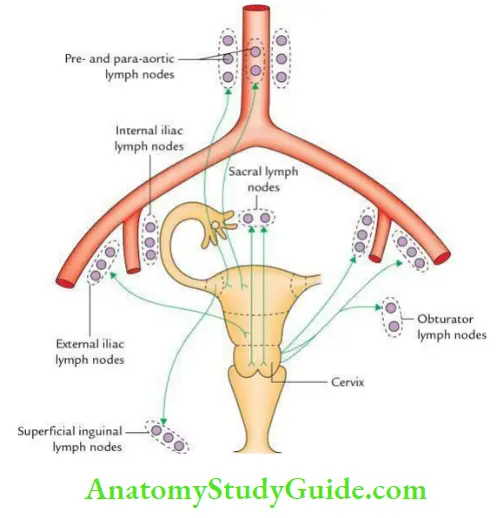
6. Uterus Lymphatic drainage:
The lymph from the uterus is drained as follows:
- From the fundus and upper part of the body:
- Most of the lymph vessels pass along the ovarian vessels to drain into para-aortic and pre-aortic lymph nodes.
- However, some lymph vessels from the region of the lateral angle of the uterus pass along the round ligament to drain into superficial inguinal lymph nodes.
- From the lower part of the body, lymph: Vessels travel via broad ligament to drain into the external iliac lymph nodes.
- From the cervix: Lymph vessels pass:
- Laterally into broad ligament drains into external iliac lymph nodes.
- Posterolaterally along the uterine vessels to drain into internal iliac lymph nodes.
- Posteriorly along the uterosacral ligaments to drain into sacral lymph nodes.
7. Uterus Applied anatomy:
- Carcinoma cervix: It is the second commonest cancer in females and often occurs in the age group between 40 to 45 years. It is squamous cell carcinoma and spreads directly to adjacent structures.
- Prolapse of the uterus: In this condition, the uterus descends into the vagina. It occurs due to the weakness of various supports of the uterus.
- Hysterectomy: It is the surgical removal of the uterus.
- Cesarean section: It is the surgical procedure to deliver the baby by incising the uterus in cases where vaginal delivery is difficult or not possible.
Leave a Reply