Classify/name antithyroid drugs. Describe briefly their uses. Add a note on the treatment of thyroid storm.
Answer:
Hyperthyroidism is due to an excess of circulating thyroid hormones and could be due to various causes. Graves’ disease, an autoimmune disorder, is the most common cause. It is characterized by hyperthyroidism, diffuse goiter, and IgG antibodies that activate TSH receptors. Antithyroid drugs may act by interfering with the synthesis, release or actions of thyroid hormones.
Read And Learn More: Pharmacology Question And Answers

Antithyroid drugs:
- Inhibit hormone synthesis
- Thioureylenes: Propylthiouracil, methimazole, carbimazole
- Inhibit hormone release
- Iodine, iodides, iodinated radiocontrast media.
- Ionic inhibitors
- Thiocyanate, perchlorate.
- Destroy thyroid tissue
- Radioactive iodine
- Others: Lithium, cholestyramine
Thioureylenes/Thionamides:
- Actions: Thioureylenes reduce the synthesis of thyroid hormones by inhibiting the iodination of tyrosine residues and the coupling of iodotyrosine residues.
- They bring about these effects by inhibiting the peroxidase enzyme. Propylthiouracil also inhibits peripheral conversion of T4 to T3.
- T3 and T4 levels gradually fall. Large doses may stimulate the release of TSH resulting in thyroid enlargement.
- Over 3 – 4 weeks of treatment, the signs and symptoms of hyperthyroidism subside (see Compare and contrast of propylthiouracil and methimazole).

Propylthiouracil and methimazole:

Thioureylenes Pharmacokinetics:
- Thioureylenes are effective orally and well absorbed; about 75% propylthiouracil is firmly bound to plasma proteins hence very little crosses the placenta and a negligible fraction reaches the milk; but carbimazole and methimazole cross the placenta and are secreted in the milk.
- Thioureylenes are concentrated in the thyroid and, therefore, their effects persist even when plasma levels fall (their plasma t½ is short). They are metabolized in the liver.
Thioureylenes Adverse effects:
- Allergic reactions like skin rashes, urticaria, dermatitis
- Hepatitis, cholestatic jaundice, headaches can occur
- Agranulocytosis is a rare but serious adverse effect and is reversible on stopping the antithyroid drug but the patient should be monitored with frequent WBC counts.
- Thioureylenes can also cause arthralgia, myalgia, lymphadenopathy, and rarely, psychosis.
Question. Write briefly the uses of antithyroid drugs/propylthiouracil. What is a thyroid storm? How is it treated?
Answer:
Thyroid Storm Uses:
- Graves’ disease: Graves’ disease or diffuse toxic goiter needs long-term (1–15 years) treatment with antithyroid drugs. Thyroid hormone levels return to normal in about 12 weeks but treatment should be continued. Smaller maintenance doses are then sufficient. Radioactive iodine therapy is now considered the definitive therapy in most patients with Graves’ disease.
- Toxic nodular goiter: Used when surgery cannot be done as in the elderly.
- Preoperatively: Hyperthyroid patients are made euthyroid and then operated.
- Hyperthyroidism in pregnancy: Propylthiouracil is the preferred drug in 1st trimester as it poorly crosses the placental barrier. During 2nd and 3rd trimester, patient is switched to carbimazole. In lactating mothers, though only a negligible amount of propylthiouracil is
secreted in the milk, due to toxicity, methimazole (10–30 mg/day) is used. - With radioiodine: Radioiodine treatment requires about 3 months for the response. Antithyroid drugs may be employed till then to control hyperthyroidism.
- Thyroid storm: A thyroid storm or thyrotoxic crisis is a sudden, severe exacerbation of thyrotoxicosis and can be life-threatening.
Trigger factors:
- Stress, infections, trauma, surgery, and inadequately treated thyrotoxic patients may go into thyroid storm.
- Symptoms include fever, tachycardia, nausea, vomiting, diarrhea, profuse sweating, confusion, restlessness, pulmonary edema, CCF and may lead on to coma and death.
Treatment of thyroid storm:
- Propylthiouracil 400–600 mg stat orally or rectally enema to block the hormone synthesis (alternative carbimazole 20 mg).
- 6–10 drops of oral/rectal potassium iodide or Lugol’s iodine inhibit the release of hormones from the thyroid gland.
- IV hydrocortisone 50 mg repeated every 6 hours helps to combat shock and also blocks the conversion of T4 to T3.
- Propranolol (1–2 mg slow IV or 40–60 mg oral QID) is used to rapidly control the symptoms, particularly cardiovascular symptoms. It also impairs the conversion of T4 to T3.
- If propranolol is contraindicated, diltiazem 60–120 mg TDS may be used to control hypertension and tachycardia.
- Inhibit thyroid hormone release and peripheral conversion of T4 to T3.
- Tepid sponging, sedation, IV fluids, and supportive therapy.
- Peritoneal dialysis may be required to clear the plasma thyroxine.
Iodides
Question. Write a short essay on iodides.
Answer:
Iodides:
Administration of iodides inhibits the synthesis and release of thyroid hormones.
WolffChaikoff effect: It is an autoregulatory effect, T3 and T4 levels fall and in thyrotoxic patients, the symptoms subside in 1–2 days.
- The gland becomes firm, less vascular, and shrinks in size over a period of 10–14 days.
- These effects may be used to quickly reduce thyroid hormone levels as in thyroid storm but the effect decreases after 14–15 days (known as thyroid escape).
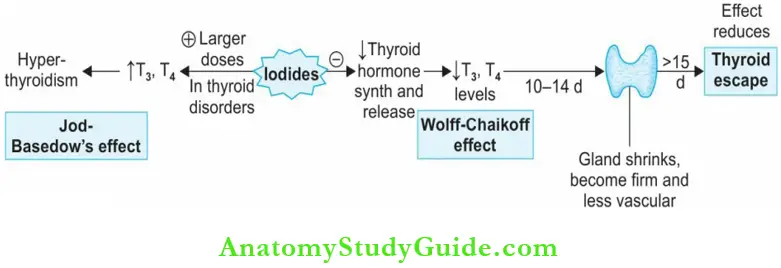
Jod-Basedow effect:
- Jod-Basedow effect is iodine-induced hyperthyroidism seen in patients with thyroid abnormalities. It may also be produced by iodine-containing drugs like amiodarone.
- Iodides are administered orally as Lugol’s iodine or as potassium iodide solution—3 drops 3 times a day. Iodine is converted into iodides in the intestine which is then absorbed.
Iodides Uses:
- Preoperative preparation for thyroidectomy: Iodine is started 10 days prior to surgery to make the thyroid gland firm and less vascular.
- Thyroid storm: Iodides act rapidly to reduce the release of thyroid hormones.
- Prophylaxis: Iodide or iodate is added to common salt to prevent endemic goiter.
- Protection against radioactivity: Potassium iodide given prophylactically following a nuclear accident protects the thyroid from radioactive iodine (by Wolff-Chaikoff effect)
- Antiseptic: Iodine has antimicrobial properties including antifungal effects.
- Expectorant: Potassium iodide is used in cough.

Iodides Preparations:
Lugol’s iodine (5% iodine in 10% potassium iodide solution).
- For topical use: Povidone-iodine (5–10% solution).
- Tincture of iodine: Tincture of iodine(2% iodine with 2.4% sodium iodide).
Iodides Adverse effects:
- Including allergic reactions like skin rashes, conjunctivitis, rhinitis, vasculitis, swelling of the lips and salivary glands, fever, and lymphadenopathy.
- Chronic overdose can cause iodism with a metallic taste, excessive salivation, lacrimation, burning sensation in the oral cavity and throat, running nose, sore throat, cough, headache, and rashes.
Iodine overdose: Acute toxicity with iodine can be fatal (3–4 g—fatal dose).
Signs and symptoms: Iodine is a powerful irritant and vesicant.
- Nausea, vomiting, diarrhea, and an unpleasant metallic taste.
- Vesication, desquamation, and corrosion of skin and mucous membrane with brownish-yellow stains.
- Corrosion and perforation of mouth, throat, and GI tract.
- Nephritis and renal failure.
- Delirium, stupor.
- Inhalation produces edema of the glottis and pulmonary edema.
- Anaphylactic reactions can occur.
Iodides Treatment:
- Starch or flour solution was given orally (30 g per liter of water). Milk is also helpful.
- Sodium thiosulphate the antidote is given orally (1–5% solution). This will convert iodine to iodide which is relatively harmless.
- Skin lesions—treated with 20% alcohol.
- Supportive therapy.
- Induction of vomiting or stomach wash is contraindicated.
Iodism:
- Iodism is chronic poisoning with iodide salts and is characterized by erythema, urticaria, acne, stomatitis, conjunctivitis, rhinorrhea, parotid swelling, lymphadenopathy, anorexia, and insomnia.
- Treatment—intake of sodium chloride → chloride competes with iodide for excretion at the level of the renal tubules and promotes excretion of iodides.
Radioactive Iodine
Question. Write briefly on radioactive iodine.
Answer:
Radioactive Iodine:
- 131Igiven orally as a solution is rapidly absorbed and is concentrated by the thyroid in the follicles. It emits both γ and β rays.
- The γ rays pass through the thyroid tissue, while β particles penetrate only 0.5–2 mm of the tissue due to which it destroys only the thyroid tissue without damaging the surrounding structures.
- 131Ihas a half-life of 8 days but the radioactivity is present up to 2 months. It is given as a single dose; clinically the effect is seen after 1–2 months but the peak effect seen in 3–6 months.

Radioactive iodine Uses:
- Hyperthyroidism (3–10 millicuries)
- Toxic nodular goiter
- Thyroid carcinoma—when surgery is not possible.
- Diagnostic tests—small doses used (in microcurie doses).
- Patients should be instructed to dispose of the urine carefully in the toilet and flush it with enough water.
- Patients should be kept away from children and pregnant women for 2–3 days.
Radioactive iodine131I Advantages:
- Administration is simple
- Convenient—given as an outpatient.
- Surgery and its associated risks and morbidity can be avoided.
- Less expensive when compared to surgery.
Radioactive iodine131I Disadvantages:
- Long time (3 months) taken for maximum response.
- Risk of hypothyroidism—after months → needs follow-up and replacement therapy with hormones.
- Risk of thyroid carcinoma—since radiation can be carcinogenic, there is a risk of secondary carcinoma (though uncommon). Hence, its use is restricted to adults.
Leave a Reply