Extrahepatic Biliary Apparatus
Question – 1: Describe Extrahepatic Biliary Apparatus under the following heads
Table of Contents
1. Extrahepatic Biliary Apparatus Gross anatomy
2. Extrahepatic Biliary Apparatus Histology of gallbladder, and
3. Extrahepatic Biliary Apparatus Applied anatomy.
Answer:
Extrahepatic Biliary Apparatus Introduction: It includes all the structures which are present outside the liver and related to biliary apparatus.
1. Extrahepatic Biliary Apparatus Gross anatomy
1. Components: It consists of
- Right and left hepatic ducts
- Common hepatic duct
- Gallbladder, (Cystic duct, Bile duct)
- Pancreatic duct
- Hepatopancreatic ampulla
- Major duodenal papilla
Read And Learn More: General Histology Question And Answers
2. Details of each part:
Cystic duct:
1. Length: 3 to 4 cm.
2. Extrahepatic Biliary Apparatus Features:
- The mucous membrane of the cystic duct forms a series of 5 to 12 crescentic folds.
- They are arranged spirally to form the spiral valve of Heister. This is not a true valve.
Bile duct: It is formed by the union and cystic and common hepatic duct.
1. Length: It is 8 cm.
2. Diameter: It is 6 mm.
3. Course: It runs downward and backward in the free margin of lesser omentum.
- It comes in contact with pancreatic duct in the middle of 2nd part of duodenum.
- The course of the duct in duodenum is oblique.
- Within the wall, the bile duct and pancreatic duct unite and form hepato¬pancreatic ampulla.
The mucous glands in the bile ducts secrete mucus at much greater pressure than that at which the liver cells can secrete bile.
Gallbladder:
1. Gallbladder Features:
Gallbladder Situation: It is situated on the inferior surface of right lobe of the liver.
Gallbladder Shape: Pear-shaped. ![]()
Gallbladder Dimensions:
- Length: 7 to 10 cm.
- Breadth is 3 cm at the widest part.
- Capacity is 30 to 50 ml.
2. Gallbladder Parts:
Fundus: The part of the gallbladder below the inferior border of the liver is the fundus.
Body: It lies in the fossa of the gallbladder of the liver.
The infundibulum: The infundibulum is the part of the organ between the body and neck.
Hartmann’s pouch: It is dilated part of the gallbladder present in the posteromedial wall of the neck.
The gallbladder: The gallbladder lies vertically in the angle between the 12th rib and 1st lumbar vertebra.
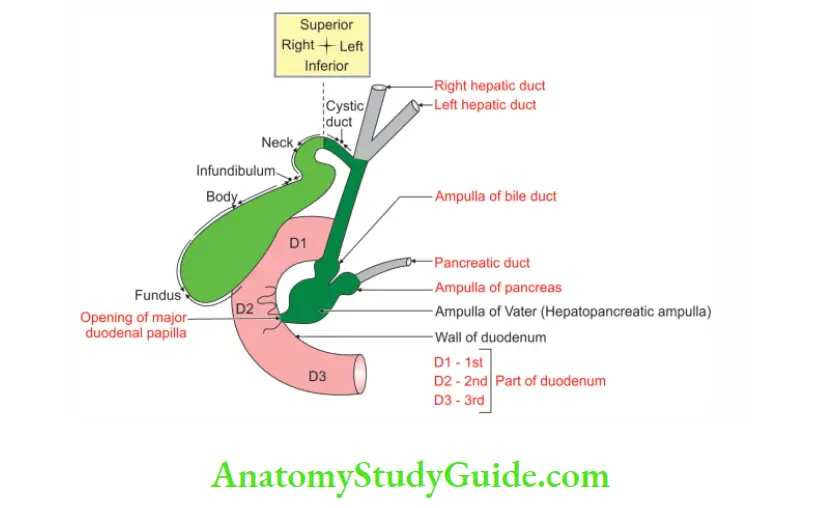
3. Relations:
Relations of the parts of gallbladder:
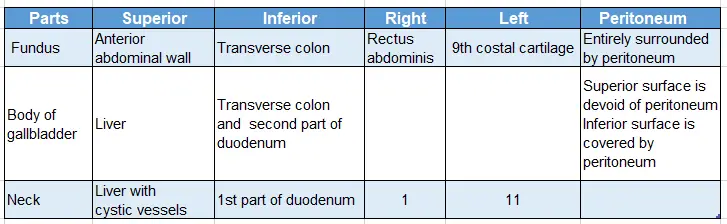
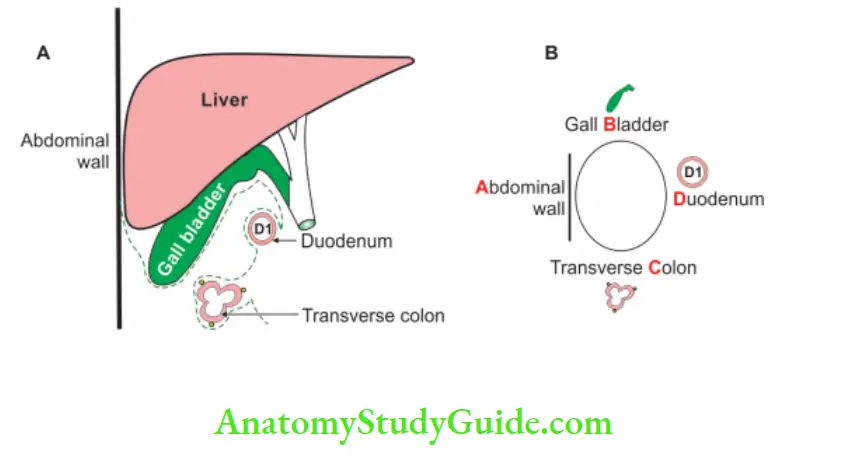
Relations of the bile duct:
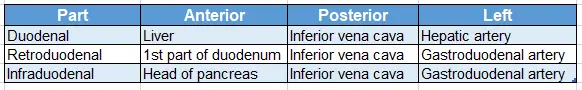
3. Blood supply:
It is divided into
Arterial supply: The blood supply to the extrahepatic bile ducts is generous. The chief artery is the posterior superior pancreaticoduodenal artery. It is assisted by the hepatic and cystic arteries. It is divided into
1. Arterial supply of biliary apparatus except the lower part of the bile duct:
- Cystic artery, a branch of the hepatic artery
- An accessory cystic artery, a branch of the common hepatic artery, and
- The artery supplying the right hepatic duct.
2. Arterial supply of a lower part of the bile duct: Several branches from the superior pancreaticoduodenal artery.
Venous Drainage:
1. Venous Drainage Features:
- There is a venous plexus on the wall of the supraduodenal portion of the common duct.
- It is an important guideline to identify the common duct while operating on the biliary system.
- This venous plexus is only visible when the overlying peritoneum has been removed. It does not extend to the cystic duct.
- The veins of the gallbladder drain into the vein of the quadrate lobe of the liver.
- They open directly or via the pericholedochal plexus.
- They ultimately enter the hepatic veins.
- They do not communicate with the portal vessels.
2. Venous drainage: Venous drainage of biliary apparatus is as follows
- The superior surface of the gallbladder drains into the hepatic vein, which drains into the inferior vena cava.
- The inferior surface of the gallbladder drains into veins of the hepatic duct, which drains into the inferior vena cava.
- The lower part of the bile duct drains into the portal vein.
4. Lymphatic drainage:
The lymphatics run in two groups. It is divided into:
1. Lymphatics of the biliary apparatus except the lower part of the bile duct drains into cystic lymph nodes.
2. Lymphatics of the lower part of the bile duct drain into
- Hepatic, and
- Upper pancreaticosplenic lymph nodes.
All these lymphatics ultimately drain into a preaortic group of lymph nodes, present in the free margin of the lesser omentum.
5. Nerve supply:
1. Part of the biliary apparatus except the lower part of the bile duct is by cystic plexus, which is formed by
- Right and left vagus
- The phrenic nerve, and
- Branch from coeliac plexus.
2. The lower part of the bile duct has a plexus over the superior pancreaticoduodenal artery.
1. Parasympathetic is
Motor to:
- The musculature of the gallbladder and
- Bile duct, and
Inhibitory: Inhibitory to the sphincters:
2. Sympathetic: Sympathetic nerve is vasomotor and inhibitory to the sphincter.
3. Pain is referred to:
- Stomach by vagi
- The right scapular region through sympathetic, and
- Right shoulder through right phrenic nerve.
2. Histology
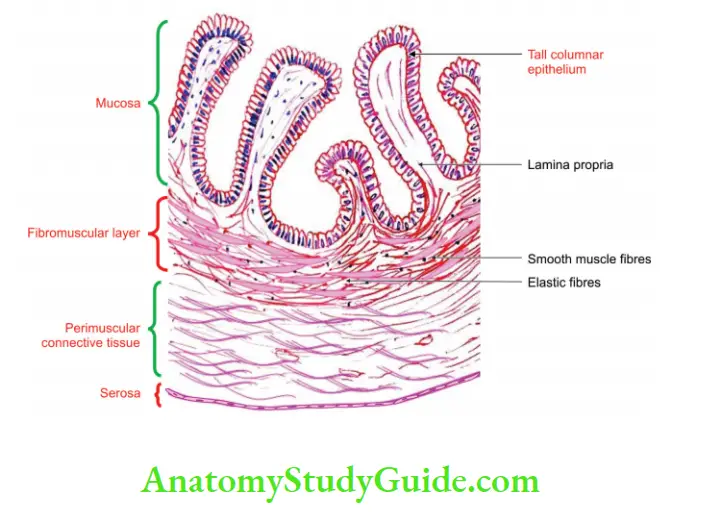
Histology of gallbladder
1. The mucous membrane of the gallbladder is lined by tall columnar epithelium with a striated border.
2. Mucosa is highly folded.
3. It is characterized by
- No goblet cells
- No muscularis mucosa, and
- No glands.
4. Muscle coat is poorly developed.
5. Serosa is lined by simple squamous epithelium.
3. Extrahepatic Biliary Apparatus Applied anatomy
1. Functions of gallbladder can be investigated by
- Ultrasonography, and
- Cholecystography
2. Inflammation of the gallbladder is called cholecystitis. This can be diagnosed by the
- History of pain in the right hypochondrium.
3. It is associated with tenderness during inspiration at the tip of the 9th costal cartilage.
- This is called Murphy’s sign.
4. The presence of gallstones in the gallbladder is called cholelithiasis.
- The operation for the removal of the gallbladder is called cholecystectomy.
5. A subcostal incision gives efficient access to the gallbladder.
6. Cystogastrocolic band: A fold may stretch from the gallbladder across the duodenum to the greater omentum or transverse colon.
7. It may produce symptoms of partial obstruction.
8. The infundibulum of the gallbladder is the 1st part usually to contract in case of adhesions of the gut.
9. Small ducts may connect the gallbladder with the liver. Usually, these become obliterated.
10. They may persist. For this reason, drainage is mandatory after cholecystectomy (cholecystohepatic duct).
11. Cancer of the gallbladder is uncommon and has a very grave prognosis.
Describe the Extrahepatic Biliary Apparatus under the following headings:
- Extrahepatic Biliary Apparatus Components
- Extrahepatic Biliary Apparatus Functions
- Extrahepatic Biliary Apparatus Gross anatomy of components
- Extrahepatic Biliary Apparatus Blood supply and
- Extrahepatic Biliary Apparatus Applied anatomy
Answer:
1. Extrahepatic biliary apparatus Components:
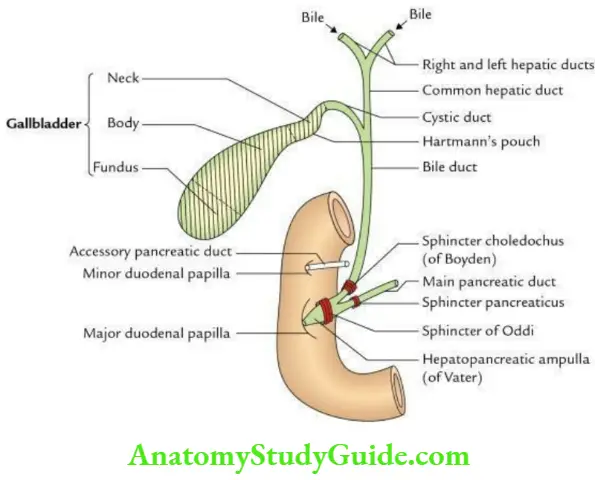
The extrahepatic biliary apparatus consists of the following components:
- Right and left hepatic ducts
- Common hepatic duct
- Gall bladder
- Cystic duct
- Bile duct
2. Extrahepatic biliary apparatus Functions:
The functions of the extrahepatic biliary apparatus are:
- Collection of bile from the liver
- Storage of bile in the gallbladder
- Transmission of bile into the second part of the duodenum
3. Extrahepatic biliary apparatus Gross anatomy of components:
- Hepatic ducts: The right and left hepatic ducts emerge from respective lobes of the liver at porta hepatis. Near the right end of porta hepatis, they join to form a common hepatic duct, which is joined by a cystic duct to form the bile duct.
- Gall bladder: It is a pear-shaped reservoir of bile situated in the fossa on the inferior surface of the right lobe of the liver.
- Size: Length 7.5–10 cm, width 3 cm, capacity 30–50 ml.
- Parts: The gall bladder consists of 4 parts:
- Fundus
- Body
- Infundibulum
- Neck
The dilatation in the posteromedial wall of the gall bladder is called Hartmann’s pouch.
4. Extrahepatic biliary apparatus Relations:
The relations of different parts of the gall bladder are given in the box below:
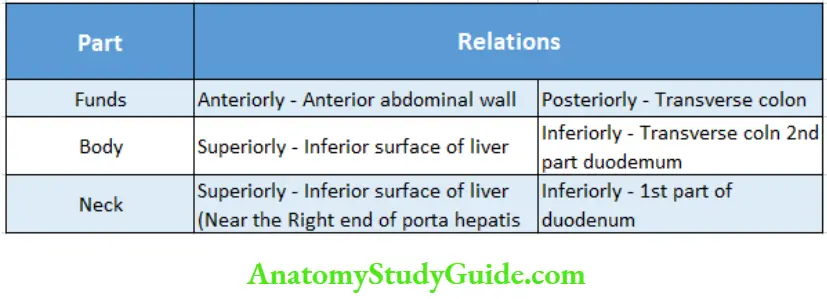
Note: The peritoneum surrounds the fundus completely and the body only on its inferior aspect.
Cystic duct:
- It is about 3–4 cm long.
- Its mucous lining presents 5–12 crescentic folds arranged spirally to form the spiral valve of Hester.
- Its dilated posteromedial wall forms a pouch called Hartmann’s pouch.
Bile duct: It is formed by the union of common hepatic and cystic ducts.
- Length: 8 cm.
- Diameter: 6 mm.
Course: It runs downward and backward in the right free margin of the lesser omentum.
- Passes behind the 1st part of the duodenum.
- Comes in contact with the pancreatic duct, near the middle of the 2nd part of the duodenum.
- Two ducts unite to form the hepatopancreatic duct which courses obliquely through the wall of the duodenum and opens on the summit of the major duodenal papilla.
Parts: It is divided into 4 parts
- The supraduodenal part is 2.5 cm long and lies in the right free margin of the lesser omentum.
- The gastroduodenal part lies in a groove on the posterior aspect of the head of the pancreas.
- The intraduodenal part lies in a groove on the posterior surface of the head of the pancreas.
- The intramural part lies in the wall of the duodenum and expands to form hepatopancreatic ampulla (ampulla of Vater).
Sphincters related to bile and pancreatic ducts:
- Sphincter choledocus (of Boyden), around the bile duct.
- Sphincter pancreatic, around the pancreatic duct.
- Sphincter ampullae/sphincter of Oddi, around hepatopancreatic ampulla.
5. Extrahepatic biliary apparatus Blood supply:
- Arterial supply: It is provided by
- The cystic artery is a branch of the right branch of the hepatic artery. It supplies all the parts of the extrahepatic biliary apparatus except the lower part of the bile duct.
- Accessory cystic artery, a branch of the common hepatic artery.
- The superior pancreaticoduodenal artery supplies the lower part of the bile duct.
- A small twig from the hepatic artery properly supplies the middle part of the bile duct.
- Few arterial twigs from the liver through the fossa for the gall bladder.
- Venous drainage: It is done by
- Cystic vein drains into the portal vein and numerous small veins from the gall bladder.
- Which enters through gall bladder fossa which drains into hepatic veins.
6. Extrahepatic biliary apparatus Applied anatomy:
Cholecystitis: The inflammation of the gall bladder is called cholecystitis.
It manifests clinically as:
- Pain over the right hypochondrium, radiating to the inferior angle of the scapula or to the tip of the right shoulder.
- Murphy’s sign is positive.
- Enlarged cystic lymph node (of Lund).
Cholelithiasis: The formation of stones in the gall bladder is called cholelithiasis. Clinically, it presents as:
- Severe spasmodic pain (biliary colic).
- Murphy’s sign was positive.
- Typically occurs in fat, fertile, flatus, females of 40 years of age.
Cholecystectomy: Surgical removal of the gall bladder is called cholecystectomy.
Leave a Reply