Male External Genital Organs
Histology of testis
Histology:
Table of Contents
Mediastinum:
- It is a posterior thickened part of the tunica albuginea.
- It sends fibrous septa to divide the interior into pyramid structures called testicular lobules.
Read And Learn More: General Histology Questions and Answers
Testicular lobule contains:
1. Seminiferous tubules: They are tightly coiled and blind-ended. They are 1 to 3 in each lobule.
2. Leydig cells: They are present between seminiferous tubules.
3. Germ cells: The details of the germ cell are shown in
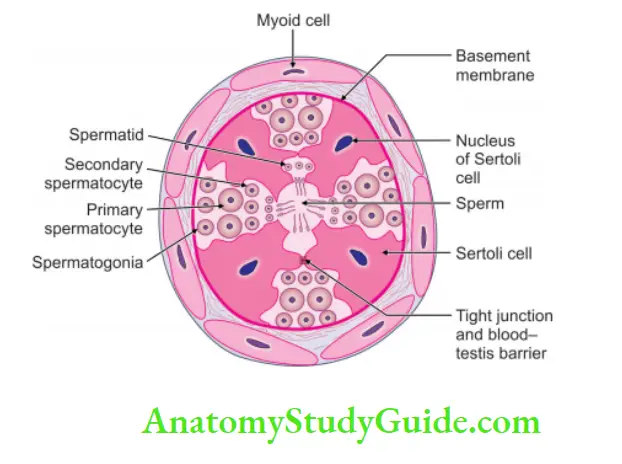
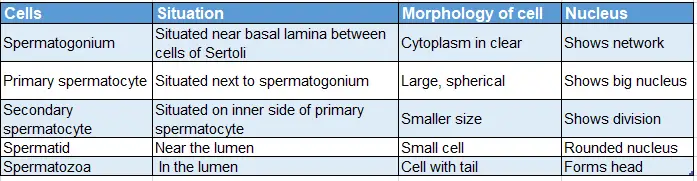
Details of the germ cell:
4. Cells of Sertoli (sustentacular cells or supporting cells).
- They are pyramidal in shape.
- They have oval
 nucleus with prominent nucleolus.
nucleus with prominent nucleolus. - Outlines of cells are faint and irregular owing to pressure by neighbouring cells.
Descent of testis
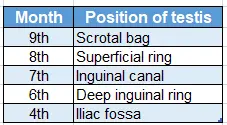
1. Chronological descent of the testes:
- One needs to know that at birth (9th month), the testes are in a scrotal bag
- Go on reducing one month for each milestone.
- In 4th month, it is at the iliac fossa.
At 9th month—scrotal bag:
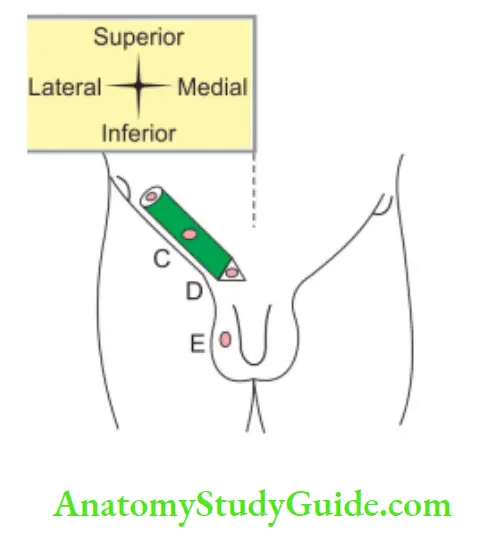
Digital memory:
How to calculate the descent of the testis
- One needs to know that at birth, the testes (9th month) are in the scrotal bag.
- Go on reducing one month for each milestone.
- In 4th month, it is at the iliac fossa.
2. Factors responsible for the descent of testis: Gonads develop behind peritoneum. They develop from the urogenital ridge in the region of the development of kidneys. The exact cause for the descent of the testis is not known. However, the factors can be grouped as
Factors which initiate the descent of testis:
1. Abdominal temperature: It is not suitable for spermatogenesis. Hence, it descends in the scrotal bag where the temperature is lower.
2. Testicular hormone: It is the most important force and is the stimulus for the descent of the testis.
3. Gubernaculum testis: It is a fibrous band, which extends from the testis to the scrotum. It helps in the following ways
- The gubernaculum and the dody wall do not grow in the same proportion.
- It helps to dilate the inguinal bursa.
- It provides a continuous pathway for the descent of the testis.
4. Formation of inguinal bursa: It is formed by the outpouching of various layers of the abdominal wall into the scrotum. The pouch progressively increases and various layers form the covering of the testis.
5. Processus vaginalis: This is a diverticulum of the peritoneal cavity. It actively grows into the peritoneal cavity. After the descent of the testis, the processus vaginalis loses all its connections with the peritoneal cavity and becomes the tunica vaginalis.
Factors which accelerate the descent of testis:
- Intra-abdominal pressure.
- Squeezing action of inguinal muscles when testis enters the inguinal canal.
3. Anomalies of descent of testis: The testis may become arrested at any point along its normal journey from the lumbar region to the base of the scrotum. Depending upon its location, it is classified into the following types.
- Lumbar, i.e. located in the abdomen (entire failure to descent).
- Iliac, i.e. situated at the entrance of the inguinal canal.
- Inguinal, i.e. situated within the inguinal canal.
- Pubic, i.e. situated at the superficial inguinal ring.
- Scrotal, i.e. situated high up in the scrotum.
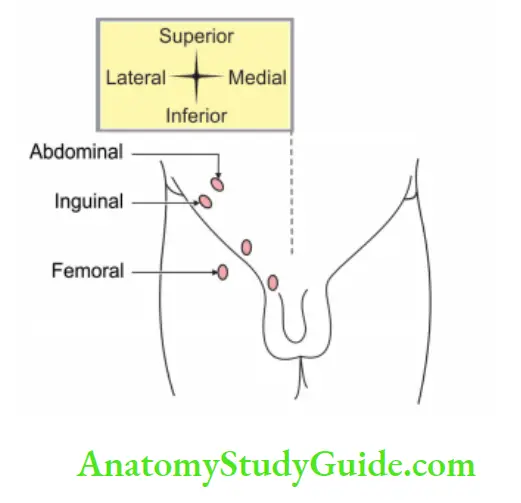
4. Ectopic testis (mal descent of testis): The testis has successfully completed its intra-abdominal descent but failed to reach the scrotum.
Following are the sites of ectopic testis:
- In the superficial fascia of the abdominal wall, above the superficial inguinal ring.
- At the root of the penis (pubopenile)
- In the perineum
- Femoral
- Gluteal
Thermoregulation of testis
It is done by:
1. Veins of pampiniform plexus: It acts as a counter-current heat exchange mechanism. It maintains the temperature of the testis a few degrees below the body temperature.
2. Cremaster muscle: It pulls the testis towards the superficial inguinal ring and plays an important role in the thermoregulation of the testis.
3. Fibromuscular ligament: It extends from the dartos muscle to the testicular pole. It may play a role in the thermoregulation of the testis.
Blood supply of testis
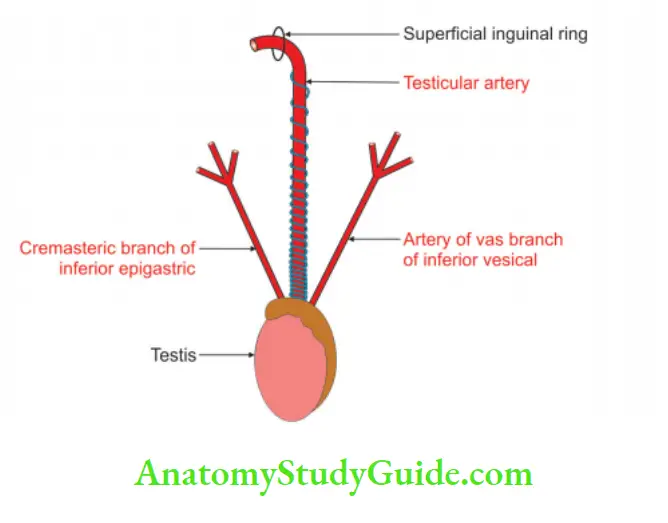
1. Arterial supply:
Testicular artery:
- It is the main artery of the testis.
- It is a lateral branch of the abdominal aorta arising at the level of the body of the L2 vertebra.
Artery to the vas: It is a branch of the superior or inferior vesical artery and sometimes it supplies the testis.
2. Venous drainage:
Veins emerging from the testis form the pampiniform plexus (Pampinus—tendril).
They are arranged into three parts :
1. Anterior part is present around the testicular artery.
2. The middle part is present around the ductus deferens.
3.posterior part is isolated
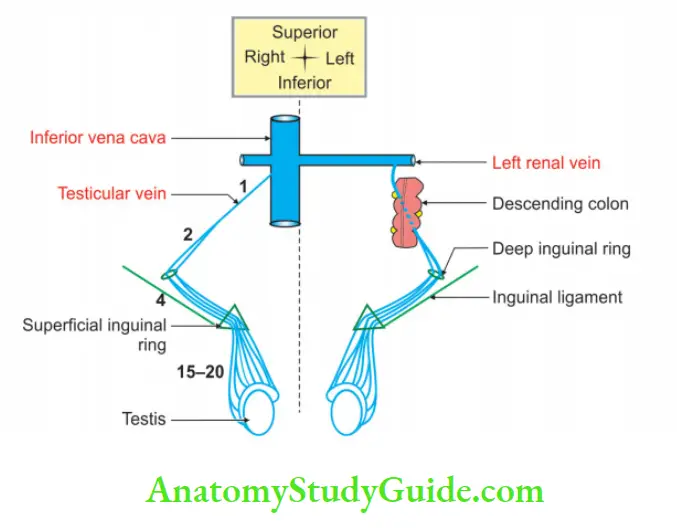
4. Plexus condenses into
- Four veins at the superficial inguinal ring.
- Two veins at the deep inguinal ring.
- One vein at the posterior abdominal wall.
- These veins accompany the testicular artery.
- The right testicular vein drains into the inferior vena cava, and
- The left testicular vein opens into the left renal vein.
I know why:
Note: The Pampiniform plexus of testicular veins acts as a counter-current heat exchange mechanism. By this, the blood in the testes is maintained at a temperature 3-4°C below body temperature.
Development of testis
1. Development
Chronological age: It develops in the 7th week of intrauterine life.
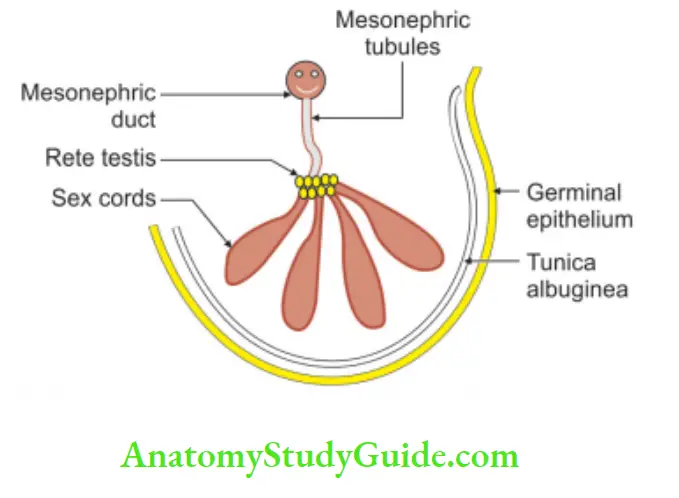
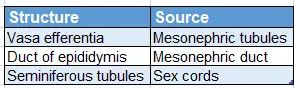
Structures, their germ layer and source of development of testis
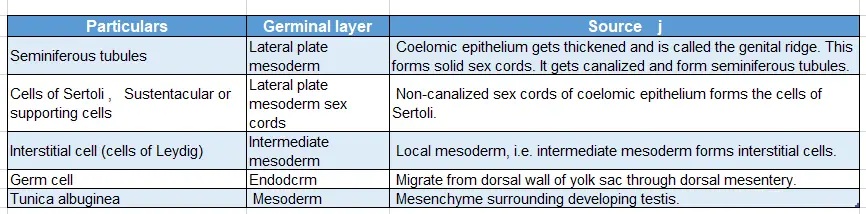
Site: In the intermediate mesoderm at the level of the 10th thoracic vertebra.
Anomalies:
1. Anomalies in number:
- Monarchism
- Anorchism: Congenital absence of testis. It may be unilateral or bilateral.
2. Anomalies of descent (cryptorchidism)
3. Abnormal positions (ectopia): The testis may lie.
1. Under the skin of the
- Lower part of the abdomen.
- Front of the thigh.
- Penis.
2. In the femoral canal.
3. In the perineum behind the scrotum.
4. The test may be duplicated.
5. The two testes may be fused together.
2. Applied anatomy
Hydrocele: Hydrocele is a condition in which the fluid accumulates in the processus vaginalis.
The following are different types of hydrocele:
Congenital:
- Vaginal: There is an accumulation of fluid in tunica vaginalis.
- Infantile: The processus vaginalis closes at the deep inguinal ring.
- Hydrocele of cord or encysted: The middle part of processus vaginalis is patent.
Epididymis
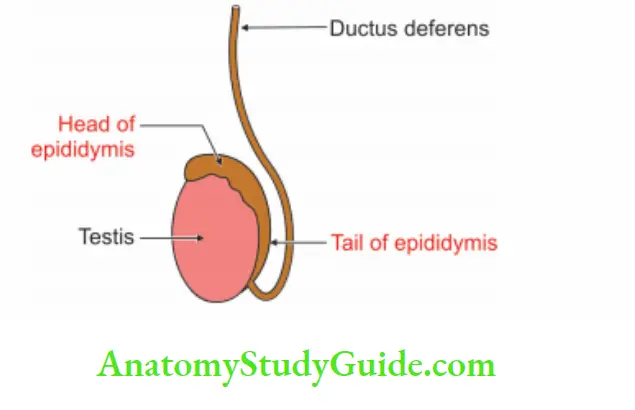
It is a comma-shaped body. It is situated along the lateral part of the posterior border of the testis. It is formed by the convolution of the tube. It has a head, body and tail.
1. Head: It is attached to the upper pole of the testis and is composed of 10 to 15 efferent tubules.
2. Body: It is composed of a single tubule coiled upon itself and lies on the posterior border of the testis.
3. Tail: It is attached by fibrous tissue to the lower pole of the testis. It continues as “vas deferens”.
4. Appendix of epididymis: The sessile or pedunculated body arising from the head is called the appendix of the epididymis. It is a remnant of the degenerated part of mesonephros.
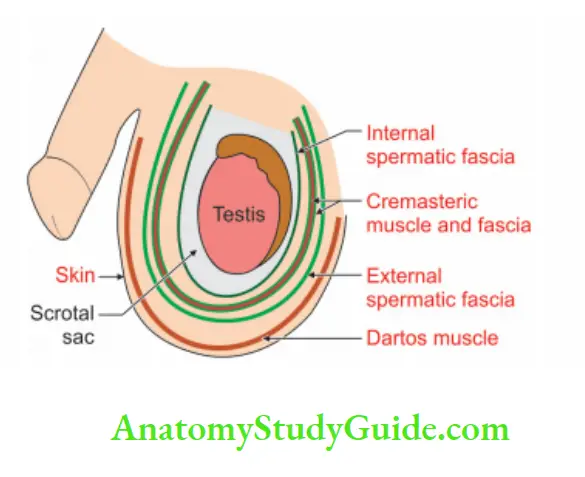
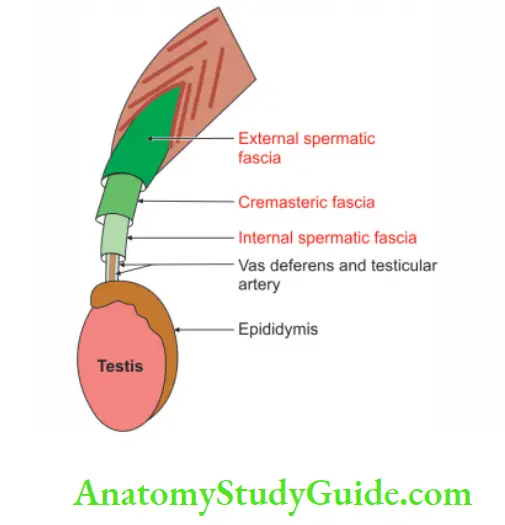
Layers of scrotum
1. Skin: The skin of the scrotum is a continuation of abdominal skin.
2. Dartos: Dartos muscle is the replacement of superficial fascia.
3. External spermatic fascia: External spermatic fascia is derived from the external oblique muscle.
4. Cremasteric fascia:
1. It consists of:
- Cremasteric muscle, and
- Areolar tissue.
2. It is derived from:
- Internal oblique, and
- Transversus abdominis.
5. Internal spermatic fascia: Internal spermatic fascia is derived from fascia transversalis.
Question – 1: Describe the testis under the following heads
Answer:
1. Gross anatomy
2. Histology
3. Development and
4. Applied anatomy.
Introduction: Testes are a pair of reproductive glands in male ♂ , present in the scrotal bag. They are homologous to the ovary in females ♀
1. Gross anatomy
1. Shape: Ellipsoid ![]()
2. Dimension:
- Length: 5 cm.
- Breadth: 2.5 cm.
- Anteroposterior dimension: 3 cm.
- Weight: 10 to 14 g
3. External features:
1. Poles: It has upper and lower poles.
- The upper pole is directed upwards and laterally and is connected to the head of the epididymis by efferent ductules of the testis.
- The lower pole is directed downwards and medially. The tail of the epididymis is connected by fibrous tissue.
2. Borders: It has two borders.
- The anterior border is convex and free.
- The posterior border is separated by a pouch of the tunica vaginalis called the sinus of the epididymis.
- Testicular vessels and nerves enter through the posterior border.
3. Surfaces: It has two surfaces
- Lateral, and
- Medial.
4. Position: It is suspended by the spermatic cord. The left testis is at a lower level as compared to the right testis.
5. Side determination: Sinus of epididymis is present on the posterior border of the lateral surface.
6. Appendix of testis: It is fibrofatty tissue present on the upper end of the testis. It is a remnant of the cephalic part of the Mullerian duct.
7. Coverings of testis: The testis is covered by three coats.
Tunica vaginalis (tunica—coat, vaginalis—sheath): It represents the lower persistent portion of processus vaginalis. It has
- The parietal layer is lined by serous epithelium.
- Visceral layer, which allows free gliding movement of the testis. It is deficient at its posterior border.
Tunica albuginea (albuginea—white): It is a white, dense fibrous coat covering the testis. It is covered by the visceral layer of tunica vaginalis. It is deficient posteriorly through which testicular vessels and nerves enter.
Tunica vasculosa (vasculosa—vessel): It is the innermost, vascular coat of the testis lining its lobules.
4. Blood supply:
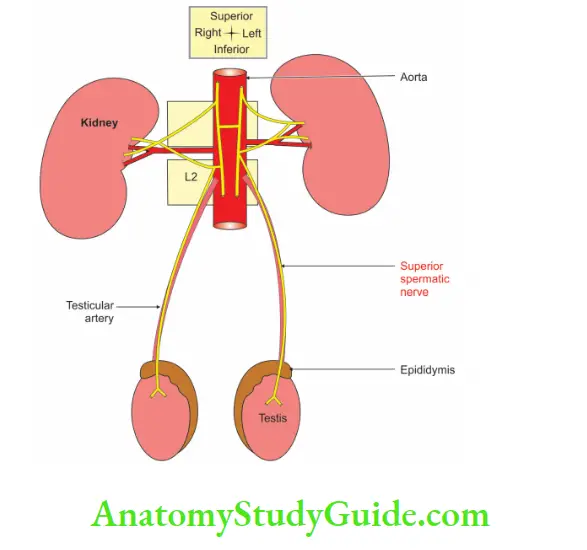
Arterial supply:
1. Testicular artery:
- It is the main artery of the testis.
- It is a lateral branch of the abdominal aorta arising at the level of the body of the L2 vertebra.
2. Artery to the vas: It is a branch of the superior or inferior vesical artery and sometimes it supplies the testis.

Venous drainage:
Veins emerging from the testis form the pampiniform plexus (Pampinus—tendril).
They are arranged into three parts :
1. Anterior part is present around the testicular artery.
2. The middle part is present around ductus deferens.
3. osterior part is isolated

4. Plexus condenses into
- Four veins at the superficial inguinal ring.
- Two veins at the deep inguinal ring.
- One vein at the posterior abdominal wall.
- These veins accompany the testicular artery.
- The right testicular vein drains into the inferior vena cava, and
- The left testicular vein opens into the left renal vein.
I know why:
Note: The Pampiniform plexus of testicular veins acts as a counter-current heat exchange mechanism. By this, the blood in the testes is maintained at a temperature 3-4°C below body temperature.
5. Nerve supply: Sympathetic
- The fibres arise from the T10 segment of the spinal cord.
- They pass through the renal and aortic plexuses.
- The fibres carry testicular sensation and are vasomotor in
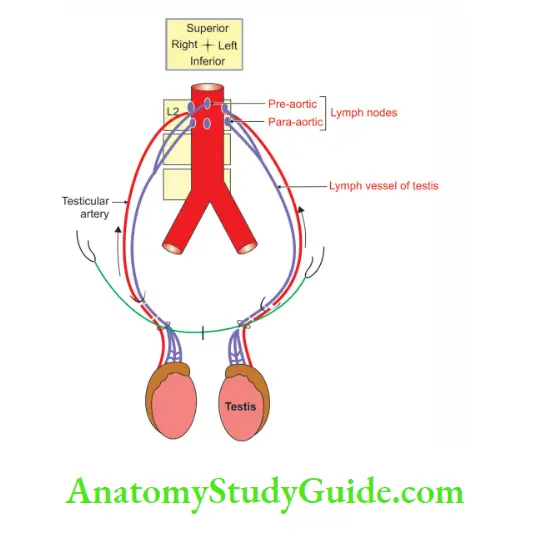
6. Lymphatic drainage:
- Lymph vessels draining the testis run along the testicular artery.
- They end in the lateral aortic group of the lymph nodes.
- They are situated at the level of 1st lumbar vertebra, i.e. at the transpyloric plane.
- Since the testis is developed in the lumbar region, this pathway explains why testicular seminoma disseminates widely and rapidly behind the peritoneum
2. Histology
Mediastinum:
- It is a posterior thickened part of the tunica albuginea.
- It sends fibrous septa to divide the interior into pyramid structures called testicular lobules.
Testicular lobule contains:
1. Seminiferous tubules: They are tightly coiled and blind-ended. They are 1 to 3 in each lobule.
2. Leydig cells: They are present between seminiferous tubules.
3. Germ cells: The details of the germ cell are shown in

Details of the germ cell:
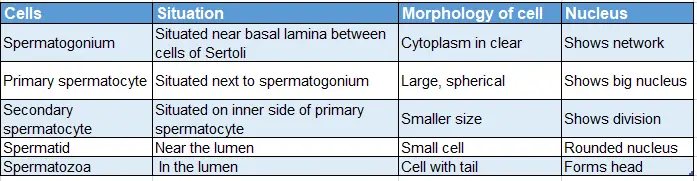
4. Cells of Sertoli (sustentacular cells or supporting cells).
- They are pyramidal
 in shape.
in shape. - They have oval
 nucleus with prominent nucleolus.
nucleus with prominent nucleolus. - Outlines of cells are faint and irregular owing to pressure by neighbouring cells.
3. Development
1. Chronological age: It develops in the 7th week of intrauterine life.
Structures, their germ layer and source of development of testis:

2. Site: In the intermediate mesoderm at the level of 10th thoracic vertebra.
3. Anomalies:
1. Anomalies in number:
- Monarchism
- Anorchism: Congenital absence of testis. It may be unilateral or bilateral.
2. Anomalies of descent (cryptorchidism)
3. Abnormal positions (ectopia): The testis may lie.
1. Under the skin of the
- Lower part of the abdomen.
- Front of the thigh.
- Penis.
2. In the femoral canal.
3. In the perineum behind the scrotum.
4. The test may be duplicated.
5. The two testes may be fused together.


4. Applied anatomy
1. Hydrocele: Hydrocele is a condition in which the fluid accumulates in the processus vaginalis.
The following are different types of hydrocele:
2. Congenital:
- Vaginal: There is an accumulation of fluid in tunica vaginalis.
- Infantile: The processus vaginalis closes at the deep inguinal ring.
- Hydrocele of cord or encysted: The middle part of processus vaginalis is patent.
Leave a Reply