Functional Anatomy Of Mouth
- The mouth is otherwise known as the oral cavity or biicca cavity. It is formed by the cheeks, lips, and palate. It encloses the teeth, tongue, and salivary glands. It opens outside anteriorly through lips and posteriorly through fauces into the pharynx.
- Digestive juice present in the mouth is saliva which is secreted by the salivary glands.
Read And Learn More: Medical Physiology Notes
Table of Contents
Functions Of Mouth
The primary function of the mouth is eating. It has a few other important functions also. The functions of the mouth are:
- Ingestion of food materials
- Chewing and mixing the food with saliva
- Appreciation of the taste
- Transfer of food (bolus) to the esophagus by swallowing.
- Role in speech
- Social functions such as smiling and other expression
Salivary Glands
In humans, saliva is secreted by three pairs of major (larger) salivary glands and some minor (small) salivary glands* In the oral and pharyngeal mucous membranes.
The major glands are:
- Parotid glands
- Submaxillary or submandibular glands
- Sublingual glands.
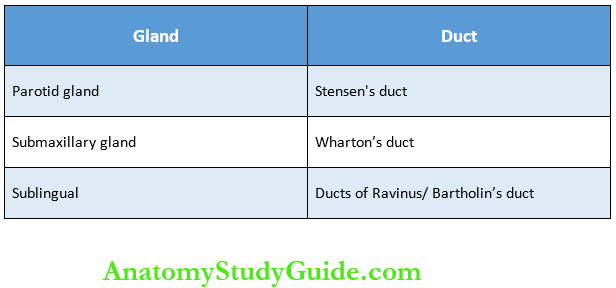
1. Parotid Glands:
- Parotid glands are the largest of the salivary glands. These glands are situated at the side of the face just below and in front of the ear. Each gland weighs about 20-30 gm in adults.
- Secretions from these glands are emptied into the oral cavity by Stensen’s duct. This duct is about 35-40 mm long and opens inside the cheek against the upper second molar tooth.
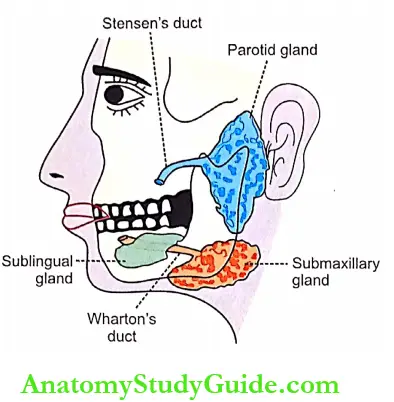
2. Submaxillary Glands:
- Submaxillary glands are otherwise known as submandibular glands. These glands are located in the submaxillary triangle medial to the mandible. Each gland weighs about 8-10 gm.
- Saliva from these glands is emptied into the oral cavity by Wharton’s duct, which is about 40 mm long. The duct opens at the side of the frenulum of the tongue by means of a small opening on the summit of the papilla called the caruncula sublingual.
3. Sublingual Glands:
- Sublingual glands are the smallest of the three pairs of major salivary glands and are situated in the mucosa at the floor of the mouth. Each gland weighs about 2-3 gm. Saliva from these glands is poured into 5-15 small ducts called ducts of Ravinus.
- These ducts open on small papillae beneath the tongue. One of the ducts is larger and it is called Bartholin’s duct. It drains the anterior part of the gland and opens on the caruncula sublingual near the opening of the submaxillary duct.
Minor Salivary Glands:
- Lingual mucus glands: Situated in the posterior 1/3 of the tongue, behind circum vallate papillae, and at the tip and margins of the tongue.
- Lingual serous glands: Located near the vicinity of taste buds namely circum vallate papillae and foliform papillae.
- Buccal glands: Present between the mucous membrane and buccinator muscle. Four to five of these are larger and situated outside the buccinator around the terminal part of the parotid duct. These glands are called molar glands.
- Labial glands: Situated beneath the mucous mem¬brane around the orifice of the mouth.
- Palatal glands: Found beneath the mucous membrane of the soft palate.
Classification Of Salivary Glands:
Salivary glands are classified into three types based on the type of secretion.
- Serous Glands: This type of gland is made up of serous cells predo-minately. These glands secrete thin and watery saliva. Parotid glands and lingual serous glands are serous glands.
- Mucus Glands: This type of gland is made up of mucus cells mainly. These glands secrete thick, viscous saliva with high mucin content. Lingual mucus glands, buccal glands, and palatal glands belong to this type.
- Mixed Glands: Mixed glands are made up of both serous and mucus cells. Submandibular, sublingual, and labial glands are the mixed glands.
Structure And Duct System Of Salivary Glands
- Salivary glands are made up of acini or alveoli. Each acinus is formed by a small group of cells that surround a central globular cavity. The central cavity of each acinus is continuous with the lumen of the duct.
- The fine duct draining each acinus is called the intercalated duct. Many intercalated ducts join together to form an intralobular duct. A few intralobular ducts join to form interlobular ducts, which unite to form the main duct of the gland. The gland with this type of structure and duct system is’ called racemose type (racemose = bunch of grapes).
Properties And Composition Of Saliva
Properties Of Saliva:
- Volume: 1000 to 1500 mL of saliva is secreted per day and, it is approximately about 1 mL/minute. Contribution by each major salivary gland is:
- Parotid glands: 25%
- Submaxillary glands: 70%
- Sublingual glands: 5%.
- Reaction: Mixed saliva from all the glands is slightly acidic with a pH of 6.35-6.85.
- Specific gravity: It ranges between 1.002 and 1.012.
- Tonicity: Saliva is hypotonic to plasma.

Composition Of Saliva: Mixed saliva contains 99.5% water and 0.5% solids. The composition of saliva is given in.
Functions Of Saliva: Saliva is a very essential digestive juice. Since it has many functions, its absence leads to many inconveniences.
1. Preparation Of Food For Swallowing: When food is taken into the mouth, it is moistened and dissolved by saliva. The mucous membrane of the mouth is also moistened by saliva. It facilitates chewing. By the movement of the tongue, the moistened and masticated food is rolled into a bolus. The mucin of saliva lubricates the bolus and facilitates the swallowing.
2. Appreciation Of Taste: Taste is a chemical sensation. Saliva by its solvent action dissolves the solid food substances so that the dissolved substances can stimulate the taste buds. The stimulated taste buds recognize the taste.
3. Digestive Function: Saliva has three digestive enzymes namely, salivary amylase, malaise, and lingual lipase. Salivary amylase and maltase are carbohydrate-digesting (amylolytic) enzymes. The lingual lipase is a fat-digesting (lipolytic) enzyme.

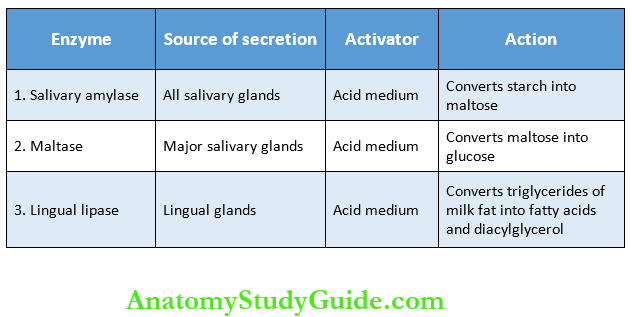
Salivary Amylase:
- Salivary amylase is a carbohydrate-digesting (amylolytic) enzyme. It acts on cooked or boiled starch and converts it into dextrin and maltose. Though starch digestion starts in the mouth, a major part of it occurs in the stomach because food stays only for a short time in the mouth.
- The optimum pH necessary for the activation of salivary amylase is 6. The salivary amylase cannot act on cellulose.
Maltase: The enzyme maltase is present only in traces in human saliva. It converts maltose into glucose.
Lingual Lipase: Lingual lipase is lipid digesting (lipolytic) enzyme U is secreted from serous glands situated on the posterior aspect of the tongue. It digests milk fats (pre-emulsified fats). It hydrolyzes triglycerides into fatty acids and diacylglycerol.
4. Cleansing And Protective Functions
- Due to the constant secretion of saliva, the mouth and teeth are rinsed and kept free of food debris, shed epithelial cells, and foreign particles. In this way, saliva prevents bacterial growth by removing materials, which may serve as culture media for the bacterial growth
- The enzyme lysozyme of saliva kills some bacteria such as staphylococcus, streptococcus, and brucella
- The proline-rich proteins present in saliva posses antimicrobial properties and play an important role in neutralizing the toxic substances tannins which are present in many food substances including fruits. These proteins also protect the teeth by stimulating enamel formation
- Lactoferrin of saliva also has antimicrobial property
- Saliva also contains secretory immunoglobulin IgA which has antibacterial and antiviral actions
- Mucin present in the saliva protects the mouth by lubricating the mucous membrane of the mouth.
5. Role In Speech: By moistening and lubricating soft parts of the mouth and lips, saliva helps in speech. If the mouth becomes dry, articulation and pronunciation become difficult.
6. Excretory Function:
- Many substances, both organic and inorganic, are excreted in saliva. It excretes substances like mercury, potassium iodide, lead, and thiocyanate. Saliva also excretes some viruses such as those causing rabies and mumps.
- Ui some pathological conditions, saliva excretes certain substances, which are not found in saliva under normal conditions such as glucose in diabetes mellitus. in certain conditions, some of the normal constituents of saliva are excreted in large quantities. For example, excess urea is excreted in saliva during nephritis, and excess calcium is excreted during hyperparathyroidism.
7. Regulation Of Body Temperature: In dogs and cattle, excessive dripping of saliva during panting helps in the loss of heat and regulation of body temperature. However, in human being sweat glands play a major role in temperature regulation and saliva does not play any role in this function.
8. Regulation Of Water Balance: When the body water content decreases, salivary secretion also decreases. This causes dryness of the mouth and induces thirst. When the water is taken, it quenches the thirst and restores the body’s water content.
Regulation Of Salivary Secretion
Salivary secretion is a continuous process. But the quantity of saliva secreted varies depending upon the activity of the mouth. For example, during mastication of food, the secretion increases, and during sleep, it decreases. The secretion of saliva is regulated by the nervous mechanism. No hormonal or chemical mechanism is involved in the regulation of salivary secretion.
- Nerve Supply To Salivary Glands: Salivary glands are under the control of an autonomic nervous system and receive efferent nerve fibers from both parasympathetic and sympathetic divisions of the autonomic nervous system.
- Parasympathetic Fibers: The parasympathetic nerve fibers supplying the salivary glands arise from the superior and the inferior salivatory nuclei, which are situated in the pons and medulla, respectively.
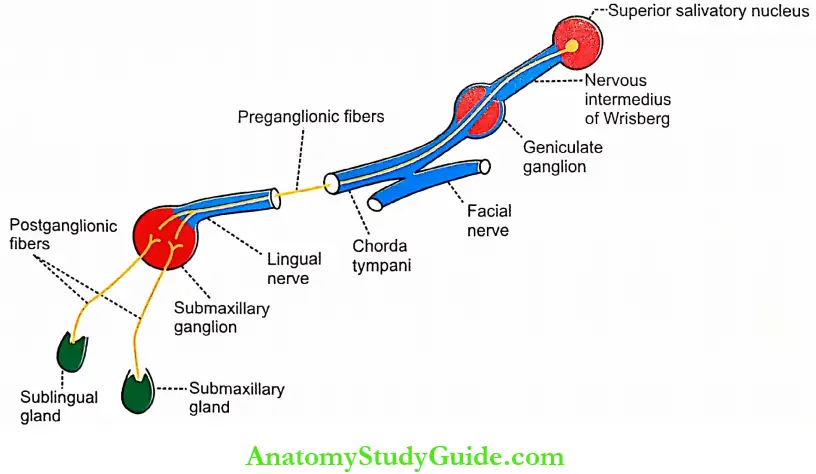
- Parasympathetic Fibers to Submandibular and Sublingual Glands:
- The parasympathetic preganglionic fibers to sub-mandibular and sublingual glands arise from the superior salivatory nucleus situated in the pons. After taking origin from this nucleus, the preganglionic fibers run through the nervous intermedius of Wrisberg, the geniculate ganglion, the motor fibers of the facial nerve, chorda tympani branch of the facial nerve, and the lingual branch of the trigeminal nerve and finally reach the submaxillary ganglion.
- The postganglionic fibers arising from this ganglion supply the submaxillary and sublingual glands.
- Parasympathetic Fibers to Parotid Gland:
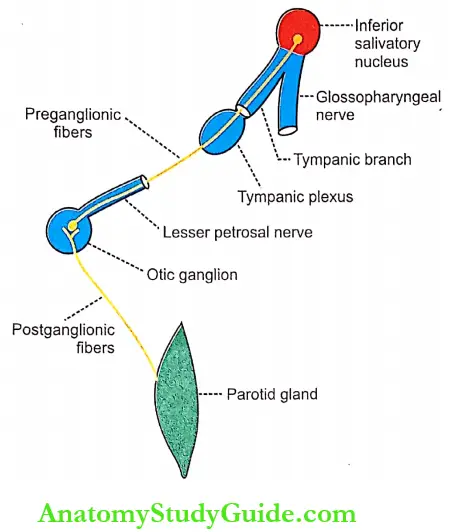
- The parasympathetic preganglionic fibers to the parotid gland arise from the inferior salivatory nucleus situated in the upper part of the medulla oblongata. From here, the fibers pass through the tympanic branch of the glossopharyngeal nerve, tympanic plexus, and lesser petrosal nerve and end in the otic ganglion.
- The postganglionic fibers from the otic ganglion reach the parotid gland by passing through the auriculotemporal branch in the mandibular division of the trigeminal nerve.
- Parasympathetic Fibers to Submandibular and Sublingual Glands:
Sympathetic Fibers:
- The sympathetic preganglionic fibers to salivary glands arise from the lateral horns of the first and second thoracic segments of the spinal cord. The fibers leave the cord through the anterior nerve roots and end in the superior cervical ganglion of the sympathetic chain.
- The postganglionic fibers from this ganglion are distributed to the salivary glands along the nerve plexus around the arteries supplying the glands.
Function Of Nerve Fibers Supplying Salivary Glands:
- Function of Parasympathetic Fibers: When the parasympathetic fibers of salivary glands are stimulated. a large quantity of watery saliva is secreted. TftCi amount of organic constituents is less. It is because like parasympathetic fibers activate the acinar cells and dilate the blood vessels of salivary glands. The neuro- transrnitier is acetylcholine.
- The function of Sympathetic Fibers: The stimulation of sympathetic fibers causes less secretion of saliva, which is thick and rich in mucus, it is because these fibers activate the acinar cells and cause vasoconstriction by secreting noradrenaline.
Reflex Regulation Of Salivary Secretion:
Salivary secretion is regulated by nervous mechanism and it is a reflex phenomenon. Salivary reflexes are of two types:
- Unconditioned Reflex
- Conditioned reflex.
1. Unconditioned Reflex: Unconditioned reflex is the inborn reflex that is present since birth. It does not need any previous experience. This reflex induces salivary secretion when any substance is placed in the mouth. It is due to the stimulation of nerve endings in the mucus membrane of the oral cavity.
2. Conditioned Reflex: Conditioned reflex is the one that is acquired by experience and it needs previous experience (Chapter 162). The presence of food in the mouth is not necessary to elicit this reflex. By this reflex, salivary secretion occurs by the sight, smell, hearing or thought of food. It is due to the impulses arising from the eyes, nose, ear, etc.
Effect Of Drugs And Chemicals On Salivary Secretion
- Substances which increase salivary secretion
- Sympathomimetic drugs like adrenaline and ephedrine stimulate salivary secretion.
- Parasympathomimetic drugs like acetylcholine, pilocarpine, muscarine, and physostigmine increase the secretion of saliva.
- Histamine stimulates the secretion of saliva.
- Substances which decrease salivary secretion
- Sympathetic depressants like ergotamine and dib enamine abolish the salivary secretion.
- Parasympathetic depressants like atropine and scopolamine inhibit the secretion of saliva.
- Anesthetics such as chloroform and ether stimulate the reflex secretion of saliva. However, deep anesthesia decreases the secretion due to central inhibition.
- Applied Physiology
Hyposalivation:
The reduction in the secretion of saliva is called hyposalivation. It is of two types, namely, temporary hyposalivation and permanent hyposalivation.
1 Temporary hyposalivation occurs in:
- Emotional conditions like fear
- Fever
- Dehydration.
2. Permanent hyposalivation occurs in:
- Sialolithiasis – Obstruction of salivary duct
- Congenital absence or hypoplasia of salivary glands
- Bell’s palsy – Paralysis of the facial nerve.
Hypersalivation:
- The excess secretion of saliva is known as hyper-salivation. The physiological condition when hyper-salivation occurs is pregnancy. Hypersalivation in pathological conditions is called ptyalism, sialorrhea, sialism or sialosis. Hypersalivation occurs in the following conditions:
- Decay of tooth or neoplasm (abnormal new growth or tumor) in mouth or tongue – Due to continuous irritation of nerve endings in the mouth
- Disease of the esophagus, stomach, and intestine
- Neurological disorders such as cerebral palsy and mental retardation
- Cerebral stroke
- Parkinsonism
- Some psychological and psychiatric conditions
- Nausea and vomiting.
Other Disorders:
In addition to hyposalivation and hypersalivation, salivary secretion is affected by other disorders also which include
- Xerostomia
- Drooling
- Chorda tympani syndrome
- Paralytic secretion of saliva
- Augmented secretion of saliva
- Mumps
- Sjogren’s syndrome.
1. Xerostomia: Xerostomia means dry mouth. It is also called pasties or cottonmouth. It is due to hyposalivation or absence of salivary secretion (aptyalism). The causes of this disease are:
- Dehydration or renal failure
- Sjogren’s syndrome (see below)
- Radiotherapy
- Trauma to the salivary gland or their ducts
- Side effects of some drugs like antihistamines, antidepressants, monoamine oxidase inhibitors, antiparkinsonian drugs, and antimuscarinic drugs
- Shock
- After smoking marijuana (a psychoactive compound from the plant cannabis).
Xerostomia causes difficulties in mastication, swallowing, and speech. It also causes halitosis (bad breath – exhalation of unpleasant odors).
2. Drooling: Uncontrolled flow of saliva outside the mouth is called drooling. It is often called ptyalism. Drooling occurs because of excess production of saliva in association with an inability to retain saliva within the mouth.
Drooling occurs in the following conditions:
- During teeth eruption in children
- Upper respiratory tract infection or nasal allergies in children
- Difficulty in swallowing
- Tonsillitis
- Peritonsillar abscess.
3. Chorda Tympani Syndrome:
- Chorda tympani syndrome is a condition characterized by sweating while eating. During trauma or surgical procedure, some of the parasympathetic nerve fibers to salivary glands may be severed. An
- nd, during the regeneration some of these nerve fibers, which run along with chorda tympani branch of the facial nerve may deviate and join with the nerve fibers supplying sweat glands. When the food is placed in the mouth, salivary secretion is associated with sweat secretion.
4. Paralytic Secretion of Saliva:
- When the parasympathetic nerve to the salivary gland is cut in experimental animals, salivary secretion increases for the first three weeks and later diminishes; finally, it stops at about the sixth week. The increased secretion of saliva after cutting the parasympathetic nerve fibers is called paralytic secretion.
- It is because of the hyperactivity of sympathetic nerve fibers to salivary glands after cutting the parasympathetic fibers. The hyperactive sympathetic fibers release of large amounts of catecholamines which induce paralytic secretion.
- More the acinar cells of the salivary glands become hypersensitive to catecholamines after denervation. The paralytic secretion does not occur after cutting the sympathetic nerve fibers to salivary glands.
5. Augmented Secretion of Saliva:
- If the nerves supplying salivary glands are stimulated twice, the amount of saliva secreted by the second stimulus is more than the amount secreted by the first stimulus.
- It Is because the first stimulus increases the excitability of acinar cells so that when the second stimulus is applied, the salivary secretion is augmented.
6. Mumps:
- Mumps is an acute viral infection affecting the parotid glands. The virus causing this disease is paramyxovirus. It is common in children who are not immunized.
- It occurs in adults also. Features of mumps are puffiness of cheeks (due to swelling of parotid glands), fever, sore throat and weakness. Mumps affects meninges, gonads and pancreas also.
7. Sjogren’s Syndrome:
- It is an autoimmune disorder in which the immune cells destroy exocrine glands such as lacrimal glands and salivary glands. It is named after Henrik Sjogren who discovered it. Common symptoms of this syndrome are dryness of the mouth due to lack of saliva (xerostomia), persistent cough, and dryness of the eyes.
- In some cases, it causes dryness of the skin, nose, and vagina. In severe conditions, the organs like kidneys, lungs, liver, pancreas, thyroid, blood vessels, and brain are affected.
Leave a Reply