Antigen, Antibody, Antigen-Antibody Reaction, And Complement
Antigen
Antigen is defined as any substance that satisfies two distinct immunologic properties:
Table of Contents
- Immunogenicity: Ability of an antigen to induce immune response in the body (both humoral and/or cell mediated).
B-cells + antigen → effector B-cells (plasma cell) + memory B-cells
T-cells + antigen → effector T-cells (helper or cytotoxic T-cell) + memory T-cells - Antigenicity (immunological reactivity): Ability of an antigen to combine specifically with the final products of the above two responses (i.e., antibodies and/or T-cell-surface receptors).
Read And Learn More: Micro Biology And Immunology Notes
All molecules having immunogenicity property, also show antigenicity, but the reverse is not true (e.g. haptens– which are antigenic, but not immunogenic).
Epitope
Epitope or antigenic determinant is the smallest unit of antigenicity:
- It is defined as a small area present on the antigen that is capable of sensitizing T- and B-cells and reacting with specific site of T-cell receptor or an antibody.
- The specific site of an antibody that reacts with the corresponding epitope of an antigen is called as paratope.
Epitopes may be grouped into two types:
- Sequential or linear epitope: Present as a single linear sequence of few amino acid.
- Conformational or nonsequential epitopes are found on the flexible region of complex antigens having tertiary structures.
In general, T-cells recognize sequential epitopes, while B-cells bind to the conformational.
Haptens
Haptens are low molecular weight molecules that:
- Lack immunogenicity (cannot induce immune response), but:
- Retain antigenicity or immunological reactivity (i.e. can bind to their specific antibody or Tcell receptor).
- However, Haptens can become immunogenic when combined with a larger protein molecule called ‘carrier’.
It is observed that hapten-carrier conjugate induces antibodies specific for: - Epitopes of hapten
- Unaltered epitopes on the carrier protein and epitopes formed by combined parts of both the hapten and carrier
- Haptens may be classified as complex or simple:
- Complex haptens contain two or more epitopes; they can react with specific antibodies and the hapten-antibody complex can be visualized by various methods such as precipitation reaction.
- Simple haptens usually contain only one epitope (univalent). Such haptens can bind to the antibodies but the hapten antibody complex cannot be not visualized as it is believed that precipitation to happen, it requires the antigen to have at least two or more epitopes.
- Factors Influencing Immunogenicity
There are various factors that influence immunogenicity of an antigen:
- Size of the antigen: Larger is the size (e.g. hemoglobin), and more is the immunogenicity.
- Chemical nature: Proteins are stronger immunogens than carbohydrates followed by lipid and nucleic acids.
- Susceptibility of antigen to tissue enzymes—It increases immunogenicity by exposing more epitopes of the Ag.
- The structural complexity of the antigen increases immunogenicity.
- Foreignness to the host: The more is the foreignness of Ag, the more is the immunogenicity.
- Genetic factor
- Optimal doses of antigen can only induce immune response. A too-little dose fails to elicit immune response and a too large dose causes immunological paralysis.
- Route of antigen administration
- Repeated doses of antigens over a while
- Multiple antigens: One antigen may diminish (due to antigenic competition) or enhance (due to adjuvant-like action) the immunogenicity of another antigen.
- Heterophile nature of the antigens (explained below).
- Adjuvant (explained below)
Adjuvant
The term adjuvant refers to any substance that enhances the immunogenicity of an antigen.
They are usually added to vaccines to increase the immunogenicity of the vaccine antigen. Examples of adjuvant include:
Heterophile Antigens
Heterophile antigens share epitopes with each other. Antibody produced against antigen of one species can react with the other and vice versa:
Biological Classes of Antigens
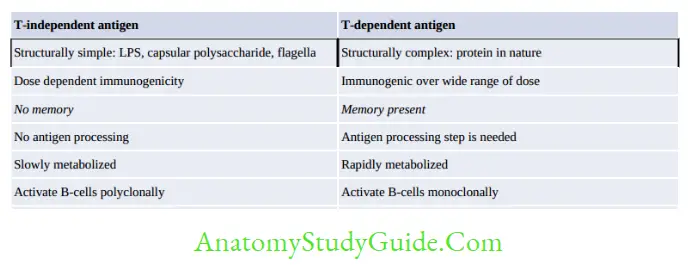
Depending on the mechanisms of inducing antibody formation, antigens are classified as T-cell dependent (TD) and T-cell independent (TI) antigens.
T-dependent (TD) Antigens
Most normal antigens are T-cell dependent, they are processed and presented by antigen-presenting cells (APCs) to T-cells.
The activated T-cells secrete cytokines that in turn stimulate the B-cells to produce antibodies.
T-independent (TI) Antigens
There are a few antigens such as bacterial capsule, flagella and LPS that do not need the help of
T-cells and APCs. They directly bind to Ig receptors present on B-cells and stimulate B-cells polyclonally leading to hypergammaglobulinemia.

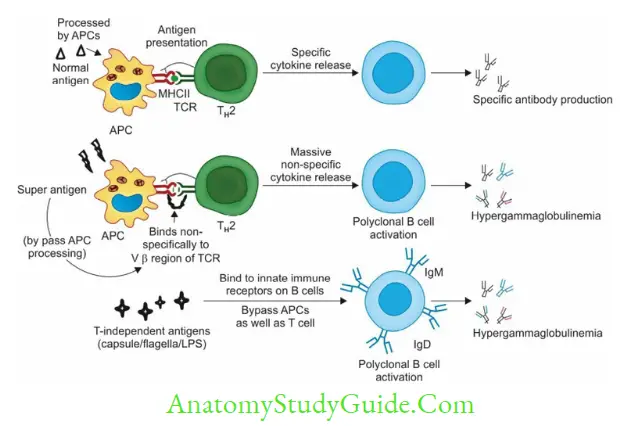
Superantigens
Superantigens are the third variety of biological class of antigens, recently described in the last decade.
The unique feature of superantigens is, they can activate T-cells directly without being processed by antigen-presenting cells (APCs).
- The variable β region of T-cell receptor (vβ of TCR) appears to be the receptor for superantigens.
- They directly bridge non-specifically between MHC-II of APCs and T-cells.
Examples of Superantigens
- Bacterial superantigen:
- Staphylococcal toxin: TSST, Exfoliative toxin, Enterotoxins
- Streptococcal toxin: Streptococcal pyrogenic exotoxin (SPE)-A and C
- Mycoplasma arthritidis mitogen-I
- Yersinia enterocolitica
- Yersinia pseudotuberculosis
- Viral: EBV, CMV, Rabies nucleocapsid, HIV encoded nef (negative regulatory factor)
- Fungal superantigen: Malassezia furfur.
Antibody
Structure of Immunoglobulins
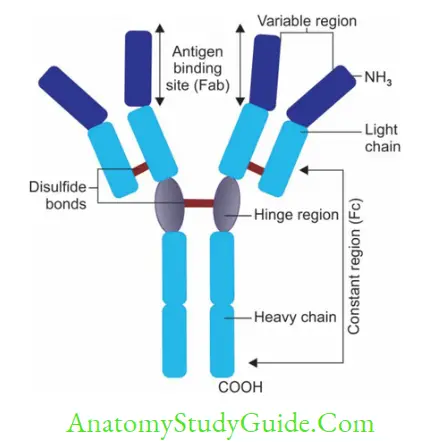
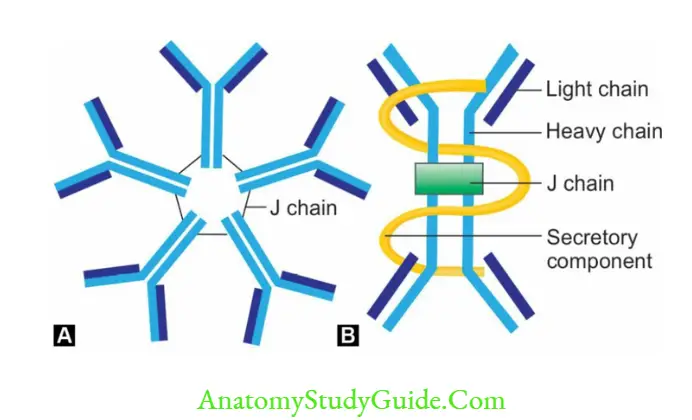
Antibody or immunoglobulin is a ‘Y- shaped’ heterodimer; composed of four polypeptide chains: two light (L) chains and two heavy (H) chains:
- All four H and L chains are bound to each other by disulfide bonds, and by noncovalent interactions such as salt linkages, hydrogen bonds, and hydrophobic bonds.
- Chains have two ends: An aminoterminal end (NH3) and a carboxylterminal end (COOH).
- There are five classes of H chains (γ, α,µ,δ and ε) and two classes of light chains (κ and λ).
- Any antibody contains only one type of light chain and one type of heavy chain.
- Based on the constant region of the heavy chains (γ, α,µ,δ and ε); Ig has been classified into five types; lgG, IgA, IgM, IgD, and IgE respectively.
- Each H and L chain comprises of two regions: Variable region and constant region
- Within the variable region, there are some zones or hot spots called as hypervariable regions or complementarity-determining regions that show higher variability. There are three hot spots in the L and four in the H chain.
- Paratope is the site on the hypervariable regions that make actual contact with the epitope of an antigen.
- Hinge region:
- It is the junction formed between constant region of heavy chains of IgG, IgA, and IgD. It is absent in IgE and IgM.
- This region is rich in proline and cysteine. The hinge region is quite flexible, thus helps the antibody in reaching towards the antigen.
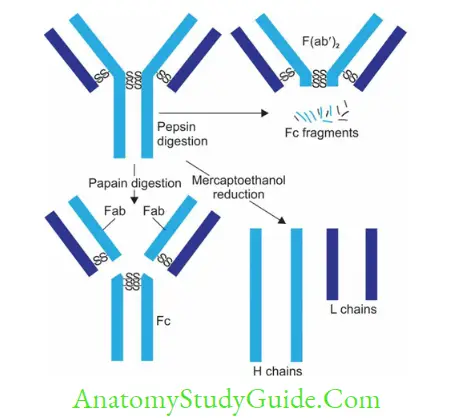
Enzymatic digestion: - Papain digestion: Papain cleaves the Ig molecule at a point above the hinge region;resulting in three fragments: Two Fab fragments (Ag binding fragment) and one Fc fragment (crystallisable fragment)
- Pepsin digestion: Pepsin cleaves the Ig molecule at a point below the hinge region; resulting in formation of-One F(ab’)2 fragment and Many smaller fragments
- Mercaptoethanol digestion: Generates four fragments (two H and 2 L chains) as it cleaves only disulphide bonds sparing the peptide bonds.
- This region is rich in proline and cysteine. The hinge region is quite flexible, thus helps the antibody in reaching towards the antigen.
Functions of Immunoglobulins
- Antigen binding (by Fab region)
- Effector functions (by Fc region)
- Fixation of complement: Antibody coating the target cell binds to complement through its Fc receptor which leads to complement-mediated target cell lysis
- Binding to various cell types: Phagocytic cells, lymphocytes, platelets, mast cells, NK cell, eosinophils and basophils bear Fc receptors (FcR) that bind to Fc region of immunoglobulins.
Abnormal Immunoglobulin
- Bence Jones Proteins: They are produced in multiple myeloma (light chain disease).
- The cancerous plasma cells produce excess of light chain (Bence Jones proteins) which are accumulated in patient’s serum and excreted in urine.
- Such proteins have a unique property of getting coagulated at 50°C and redissolving again at 70°C.
- Waldenstrom’s Macroglobulinemia: It is lymphoma affecting B-cells producing excess IgM. It has been seen in multiple myeloma. Somatic mutations in MYD 88 gene occur in over 90% of patients.
- Heavy Chain Disease: It is characterized by an excessive production of heavy chains that are short and truncated. Four types of heavy chain disease have been recognized based on H chain involved—alpha (Seligmann’s disease), gamma (Franklin’s disease), mu, and delta chain disease.
- Cryoglobulinemia: It is a condition where the blood contains cryoglobulins; a type of Ig that becomes insoluble (precipitate) at low temperatures but redissolves again if the blood is heated:
- Cryoglobulins usually consist of IgM directed against the Fc region of IgG.
- They have been associated with multiple myeloma and hepatitis C infection.
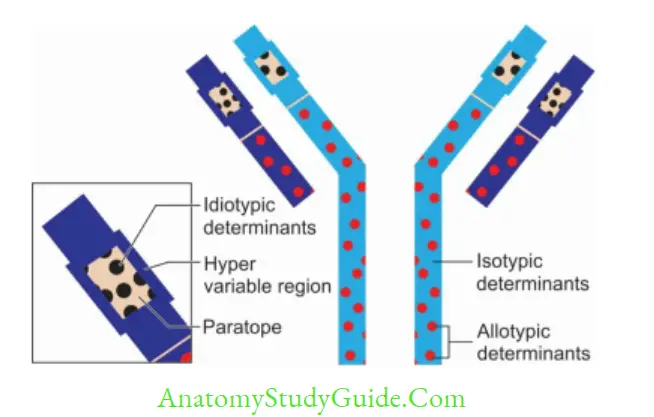
Ig Specificity or Antigenic Determinants of Ig
Isotypes
The five classes of Igs (lgG, IgA, IgM, IgD and IgE) and their subclasses are called as isotypes,they vary from each other in the amino acid sequences of the constant region of their heavy chains. Such variation is called as isotypic variation.
Idiotypes
The unique amino acid sequence present in paratope region (in VH and VL regions) of one member of a species acts as antigenic determinant to other members of the same species:
Such antigenic determinants are called as idiotopes. Immunoglobulins vary from each other in their idiotopes present in variable region, which is called as idiotypic variation.
Idiotypes in an individual arise continuously from mutations (somatic hypermutations) in the genes of variable region. Hence, idiotypes may act as foreign to the host itself; however do not evoke autoimmune response because they are present in small numbers.
Allotypes
The antigenic determinants present in the isotype genes in the constant region of H and L chains,encoded by multiple alleles are called as allotypes:
- Although all members of a species inherit the same set of isotype genes, multiple alleles exist for some of the allele genes. Hence, allotypes are present in the constant region of Ig molecules of the same class, in some, but not all, members of a species.
- They have been characterized—kappa light chain, γ and α heavy chains.
- Anti-allotype-specific antibodies may also be developed following blood transfusion or by maternal passage of IgG into the fetus.
Monoclonal Antibody
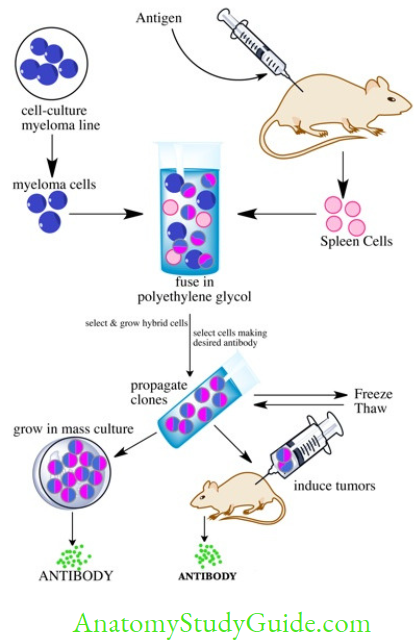
Monoclonal antibodies (mAb) are defined as the antibodies derived from a single clone of plasma cell; all having the same antigen specificity— i.e. produced against a single epitope of an antigen.
Hybridoma technique is used to produce mAb (Nobel prize Gwardee Kohler and Milstein):
- A clone of mouse splenic B-cell stimulated against a single epitope of antigen is fused with an immortal cell, e.g. myeloma cell (capable of multiplying indefinitely) to produce a hybridoma cell. This hybridoma cell has two unique properties:
- Produces mAb of the same antigen specificity (due to B-cell component)
- Multiplies indefinitely produce clone of identical cells (due to myeloma cells)
- However, in the reaction chamber, along with hybridoma cells, there will be some unfused mouse B-cell and unfused myeloma cells which are removed by sub-culturing the fluid on a special medium called HAT media.
- HAT medium contains hypoxanthine, aminopterin, and thymidine.
- Purine synthesis in mammalian cells (e.g. splenic B-cell) occurs by either de novo or salvage pathways.
- Aminopterin blocks the de novo pathway so that the cell has to perform the salvage pathway to synthesize purines for its survival.
- The salvage pathway requires two important enzymes: HGPRT (hypoxanthine-guanine phosphoribosyl transferase) and thymidine kinase.
- So any cell (e.g. myeloma cell) that lacks HGPRT cannot grow on HAT medium.
- Selection of individual hybridoma cells: By radioimmunoassay or ELISA using the specific antigen fragments
Antigen-Antibody Reaction
Antigen (Ag): Antibody(Ab) reactions are characterized by the following general properties:
- Specific: Involves specific interaction of epitope of an antigen with the corresponding paratope of its homologous antibody.
- Non-covalent interactions exist between antigen and its antibody such as:
- Hydrogen bonds
- Electrostatic interactions
- Hydrophobic interactions
- van der Waal forces
- Strength: The strength or the firmness is influenced by the affinity and avidity
- Affinity: It refers to sum total of non-covalent interactions between a single epitope of an antigen with its corresponding paratope present on antibody. It can be measured by:
(1) by equilibrium dialysis and (2) by surface plasmon resonance method - Avidity: It is a term used to describe the affinities of all the binding sites when a multivalent antibody reacts with a complex antigen carrying multiple epitopes.
- Affinity: It refers to sum total of non-covalent interactions between a single epitope of an antigen with its corresponding paratope present on antibody. It can be measured by:
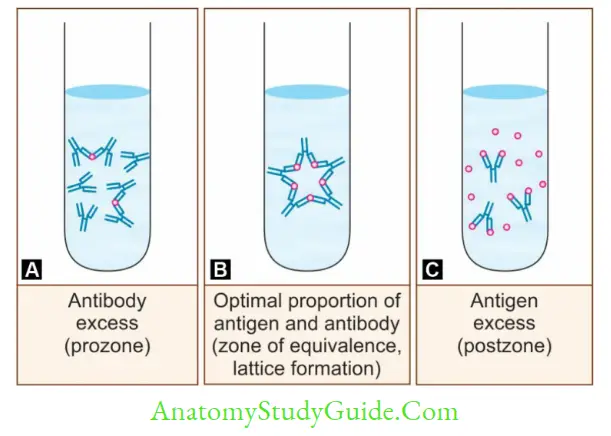
Marrack’s Lattice Hypothesis
When the sera-containing antibody is serially diluted (in normal saline), gradually the antibody level decreases. To such a set of test tubes containing serially diluted sera, when a fixed quantity of antigen is added, then:
- In the middle tubes, Ag-Ab reaction occurs at its best, because the amount of antigen and antibody are equivalent to each other (zone of equivalence).
- In the earlier test tubes, antibodies are excess, hence the Ag-Ab reaction does not occur: This
is called as prozone phenomenon. - In the later test tubes, antigen is excess, hence the Ag-Ab reaction fails to occur: This is called
as postZone phenomenon.
This lattice hypothesis holds true for any Ag-Ab reactions.
Types of Antigen-Antibody Reaction
- Conventional techniques: Precipitation, Agglutination reaction, Complement fixation test and Neutralization test
- Newer techniques: ELIS, IFA, RIA, CLIA, Immunohistochemistry, Rapid tests (Lateral flow assay or ICT and Flow through assay), Western blot and Immunoassays using electron microscope.
Precipitation Reaction
When a soluble antigen reacts with its antibody in the presence of optimal temperature, pH and electrolytes (NaCl), it leads to formation of the antigen-antibody complex in the form of:
- Insoluble precipitate band when gel-containing medium is used or
- Insoluble floccules when liquid medium is used.
Precipitation in Liquid Medium
- Ring test: Streptococcal grouping by Lancefield technique, and Ascoli’s thermoprecipitation test done for anthrax.
- Slide flocculation test: VDRL and RPR tests used for diagnosis of syphilis.
- Tube flocculation test: Kahn test used previously for syphilis.
Precipitation in Gel (Immunodiffusion)
It has many advantages over liquid medium: (1) Clear visible bands are formed, which can be preserved for longer time, (2) Individual antigens from a mixture can be differentiated, e.g.
- Single diffusion in one dimension (Oudin procedure)
- Double diffusions in one dimension (Oakley–Fulthorpe procedure)
- Single diffusion in two dimensions (Radial immunodiffusion)
- Double diffusions in two dimensions (Ouchterlony procedure), e.g. Elek’s test (diphtheria toxin) and Eiken test (E.coli toxin).
Precipitation in Gel in the Presence of Electric Current
The movement of Ag and Ab can be made faster if immunodiffusion in gel is carried out in the presence of an electric current. Examples include:
- Electroimmunodiffusion (EID)
- CIEP (Countercurrent immunoelectrophoresis)
- Rocket electrophoresis.
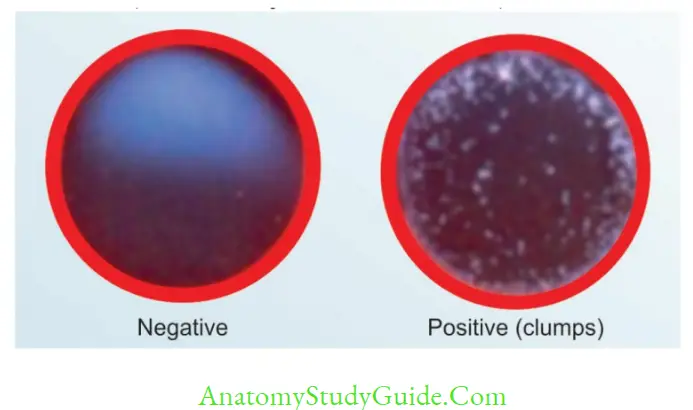
Agglutination Reaction
When a particulate or insoluble antigen is mixed with its antibody in the presence of electrolytes at a suitable temperature and pH, the particles are clumped or agglutinated.
Agglutination is more sensitive than precipitation test and the clumps are better visualized and interpreted.
Diagnostic Applications of Agglutination Tests
Slide agglutination: To confirm the identification and serotyping of bacterial colonies grown in culture.
Tube agglutination is routinely used for:
- Typhoid fever (Widal test): Detects Ab against both H (flagellar) and O (somatic) Ag
- Acute brucellosis (Standard agglutination test)
- Blood grouping (ABO and Rh grouping)
- Coombs test or Antiglobulin test: Detects incomplete Rh antibodies:
- Direct Coombs test: Detects bound Rh antibodies in fetus/baby’s serum
- Indirect Coombs test: Detects free Rh antibodies present in maternal serum.
- Heterophile agglutination tests:
- Typhus fever (Weil–Felix reaction)
- Infectious mononucleosis (Paul Bunnell test)
- Mycoplasma pneumonia (Cold agglutination test).
Microscopic agglutination test (MAT) for leptospirosis
Indirect or passive agglutination test: Antigen is coated on carriers such as Latex or RBCs to detect Ab in serum. Examples:
- Indirect hemagglutination test (IHA)
- Latex agglutination test (LAT) for antibody detection’ e.g. ASO.
Reverse passive agglutination test: Antibody is coated on carriers such as Latex or RBCs to detect Ag in serum. Examples: - RPHA (Reverse passive hemagglutination assay), e.g. HBsAg detection
- Latex agglutination test for antigen detection, e.g. CRP, RA factor, capsular antigen in CSF and streptococcal grouping.
- Coagglutination test (here, S. aureus protein A is used as carrier).
Complement Fixation Test
CFT detects complement-fixing antibodies in the patient’s serum. It is now almost obsolete:
- Wasserman test was the most popular CFT, used for the diagnosis of syphilis.
- CFT was also widely used for the detection of antibodies in Rickettsia, Chlamydia, Brucella,Mycoplasma infections and some viral infections such as arboviruses, rabies, etc.
- Indirect complement fixation test: Detects certain avian (e.g. duck, parrot) and mammalian (e.g. horse, cat) serum antibodies which cannot fix guinea pig complement.
- Conglutination test: To perform CFT using nonhemolytic complements, e.g. horse complements.
Complements are also used for various serological tests, other than CFT such as:
- Treponema pallidum immobilization test (for detecting antibodies to T. pallidum)
- Sabin-Feldman dye test for detecting Toxoplasma antibodies.
- Vibriocidal antibody test for V. cholerae.
Neutralization Test
Neutralization tests are also less commonly used in modern days. Examples include:
Newer Techniques Of Antigen-Antibody Reaction
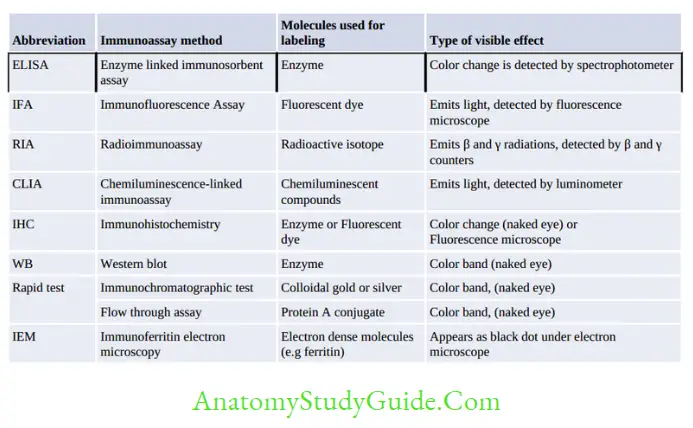
The newer techniques use a detector molecule to label antibody or antigen which in turn detects the corresponding antigen or the antibody in the sample by producing a visible effect. Most of the newer techniques use the same principle, but they differ from each other by the type of labeled molecule used and the type of visible effect produced.
ELISA (Enzyme-Linked Immunosorbent Assay)
ELISA is so named because of two of its components:
- Immunosorbent: It is an absorbing material used (e.g. polystyrene, polyvinyl), that specifically absorbs the antigen or antibody present in serum.
- Enzyme is used to label one of the components of immunoassay (i.e. antigen or antibody).
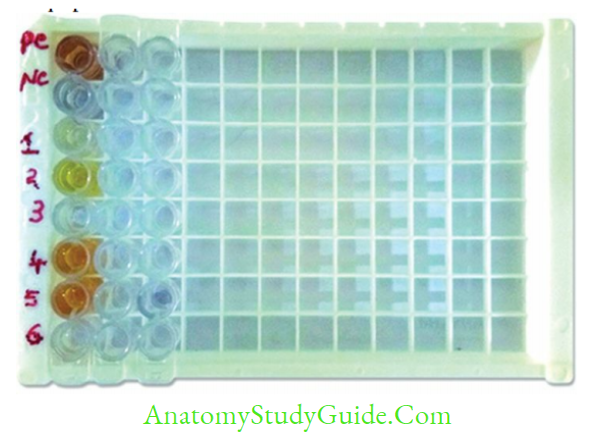
- ELISA is the method of choice in big laboratories as large number of samples can be tested together using the 96-well microtiter plate. But it is not preferred in small laboratories:
- It is economical, takes 2-3 hours (rapid tests take 10–20 min)
- ELISA is the most sensitive immunoassay, thus is the preferred screening test at blood banks and tertiary care sites.
- Its specificity used to be low. But now, with use of more purified recombinant and synthetic
antigens, and monoclonal antibodies, ELISA has become more specific. - It needs expensive equipments such as an ELISA washer and reader.
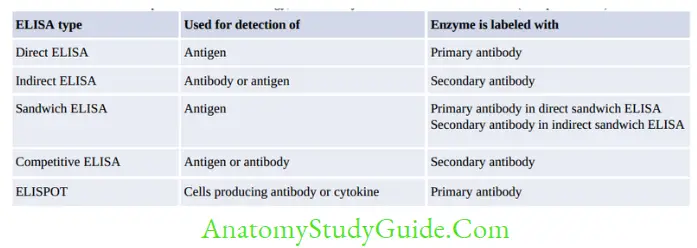
Note: Primary antibody is directed against the antigen, Secondary antibody is an anti-human (or other species) Ig directed against
Fc region of any human/other species Ig.
IgG Avidity ELISA
- Principle: Avidity of IgG indicates how firmly the IgG antibody is bound with its antigen.
Avidity reflects the maturity of the antibodies; which usually increases with time. - Low-avidity antibodies are synthesized during the primary infection. It also occurs in immunosuppression
- High avidity antibodies are produced by memory B-cells during the secondary infection, or reactivation, recovery or in vaccinated people.
- Uses IgG avidity ELISA is useful in:
- Differentiating recent and past infection
- Diagnosing atypical or subclinical course of the disease
- For diagnosing congenital infection.
- Applications: IgG avidity test is available for the following infections: rubella, CMV, VZV,toxoplasmosis, EBV, HIV, viral hepatitis and West Nile virus infection.
Immunofluorescence Assay
It is a technique similar to ELISA, but differs by some important features:
- Fluorescent dye is used instead of enzyme for labeling
- Detects cell surface antigens or antibodies bound to cell surface antigens, unlike ELISA which detects free Ag or Ab.
Types of Immunofluorescence Assays
- Direct Immunofluorescence Assay: Detects cells carrying surface antigens
- Indirect Immunofluorescence Assay: This detects antibodies bound to cell surface Ag
- Flow cytometry: This is a laser-based fluorescence technology detects 4 properties:
Western Blot
Western blot detects specific proteins (antibodies) in a sample containing mixture of antibodies each targeted against different antigens of same microbe:
- It is so named for its similarity to Southern blot (detects DNA fragments) and Northern blot (detects mRNAs).
- The Eastern blot is the latest addition to the list; it is a modification of Western blot, which detects the carbohydrate epitopes present on proteins or lipids.
Western blot comprises of three basic components:
Rapid Test
Rapid tests are revolutionary in the diagnosis of infectious diseases:
- They are very simple to perform (one step method), rapid (result obtained in 10–20 min),require minimal training, does not need any sophisticated instruments.
- These tests are also called Point of care (POC) tests, because unlike ELISA and other immunoassays, the Point of Care tests can be performed independently of laboratory equipment and deliver instant results.
Two principles of rapid tests are available:
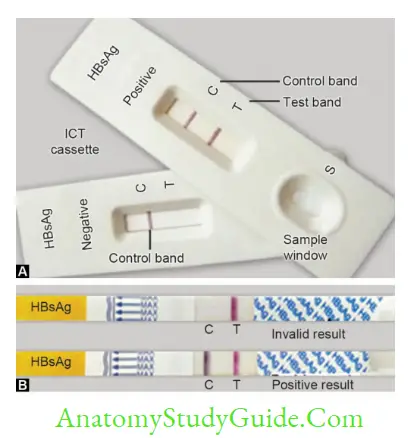
- Lateral flow assay or Immunochromatographic test (ICT): (1) colloidal gold or silver is used for labelling, (2) the sample flows laterally through the NCM. Example includes antigen detection in malaria
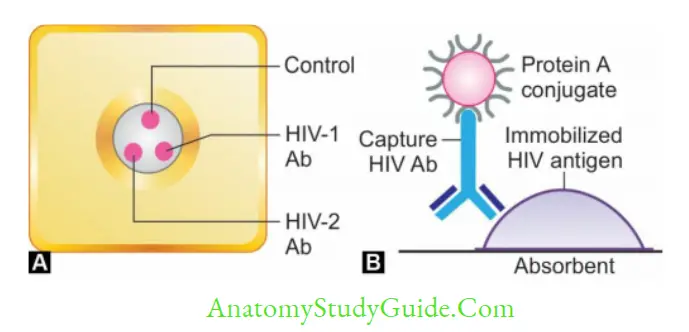
- Flow through assay: (1) Protein A is used for labelling, instead of gold conjugate and (2) the sample flows vertically through the NCM as compared to lateral flow in ICT. Example includes HIV tridot test.
Complement
Complement are a group of proteins normally found in serum in inactive form, but when activated they augment the immune responses:
- Constitute about 5% of normal serum proteins
- Antigen nonspecific: Their level does not increase following either infection or vaccination.
- Species nonspecific
- Heat labile: 56°C for 30 minutes
- Binds to Fc region of antibody: IgM (binds strongly) followed by IgG3 → 1 → 2
Site of Synthesis of Complements: Mainly by liver (C3, C6, C9), also by GIT (C1), macrophage (C2, C4) and spleen (C5, C8).
Complement Pathways
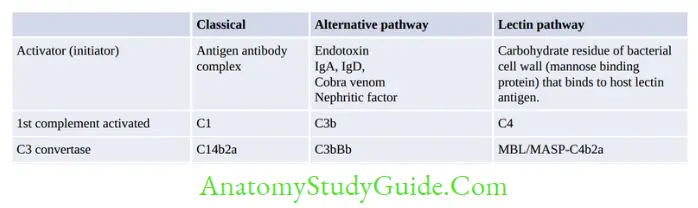
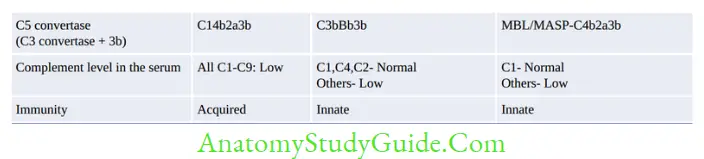
There are three pathways of complement activation (Refer figure 2.2.2):
- Classical pathway: This is an Ab-dependent pathway, triggered by the Ag-Ab complex.
- Alternative pathway: This is an Ab-independent pathway, triggered by the antigen directly.
- Lectin pathway resembles classical pathway, but it is Ab independent.
Stages of Complement Activation
There are four main stages in the activation of any of the complement pathways:
- Initiation of the pathway
- Formation of C3 convertase
- Formation of C5 convertase
- Formation of membrane attack complex (MAC)
All the three pathways (figure) differ from each other in their initiation till formation of C3 convertase. Then, the remaining stages are identical in all the pathways.
Biological Role of Complement
- Target cell lysis: MAC makes pores or channels in the target cell membrane
- Inflammatory response: Complement by-products such as C3a, C4a and C5a act as anaphylatoxins and chemotactic.
- Opsonization: C3b and C4b act as major opsonins
- Mediate hypersensitivity reaction II and III
- Removes the immune complexes from blood to spleen- by C3b
- Immune adherence: CR2 acts as EBV receptors
- Kinin-like activity (↑ vascular permeability): C2b
- Viral neutralization.
Leave a Reply