Parotid Region Anatomy Notes And Important Questions With Answers
Question: Why does opening of the jaw cause pain in mumps?
Table of Contents
Answer: The investing layer of deep fascia is modified over the parotid gland.
It forms parotid fascia.
It is dense and firmly attached to parotid gland.
In mumps, the parotid gland is inflamed.
There is no space for the expansion of the gland.
As the gland enlarges, it irritates the nerves and causes pain while opening the mouth.
| Body Fluids | Muscle Physiology | Digestive System |
| Endocrinology | Face Anatomy | Neck Anatomy |
| Lower Limb | Upper Limb | Nervous System |
Read And Learn More: Face Anatomy Notes And Important Questions
Question 2: How is the parotid gland is removed surgically?
Answer: Facial paralysis is one of the complications of removal of parotid gland.
Hence, identification of the facial nerve is essential during surgery.
The facial nerve is most distinct as it emerges from the stylomastoid foramen.
In doubtful cases, electrical stimulation may be used for confirmation.
The plane of clevage is defined by tracing the nerve behind forwards.
Question 3: Describe parotid gland under the following headings:
Answer: 1. Morphology,
2. Relations,
3. Blood supply,
4. Lymphatics,
5. Nerve supply, and
6. Applied anatomy
Morphology: It is the largest salivary gland.
- Weight: 25 g.
- Shape is like an inverted pyramid 8.
- Covering: Consists of innr true capsule, formed by condensation of peripheral part of fibrous stroma of gland. It is fibrous tissue.
- Outer false capsule: Formed by investing layer of deep cervical fascia.
It gets thickened and form stylomandibular ligament.
It extends from angle of mandible to styloid process.
It divides submandibular and parotid glands. - Presenting parts
- Apex
- Base
- Borders: Anterior, medial and posterior.
- Surface: Superficial, anteromedial and posteromedial.
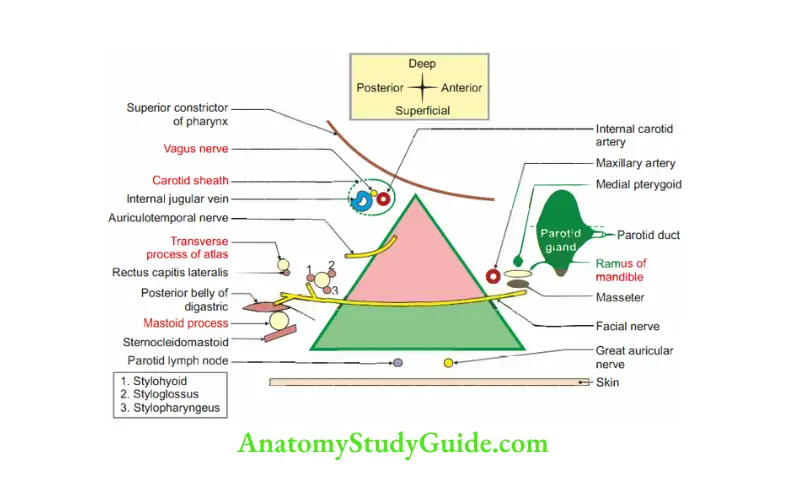
2. Relations
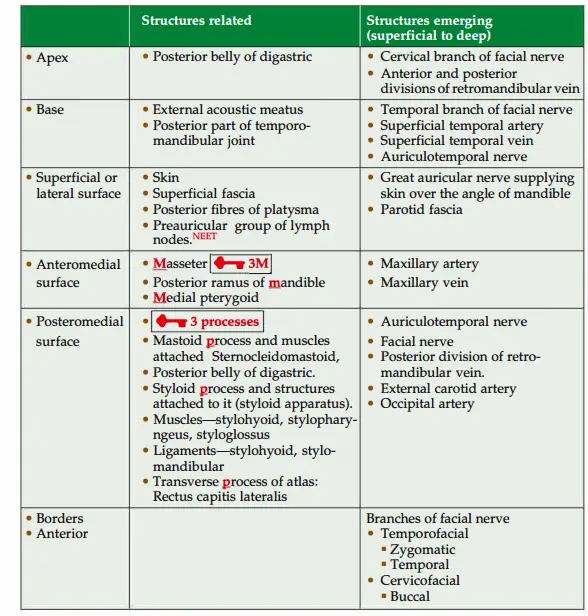
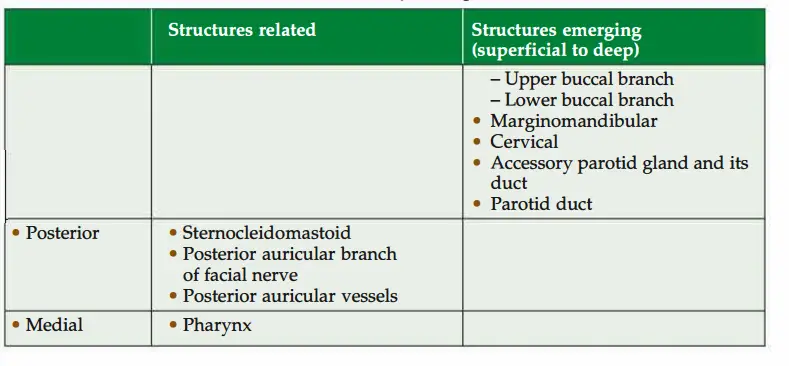
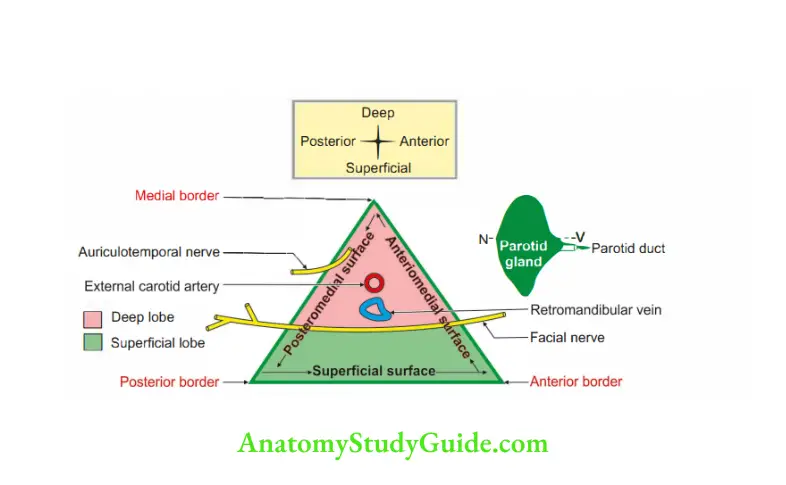
3. Blood supply
- Arterial: Branches from external carotid artery(E C A).
- Venous: Tributaries of external jugular vein(EJ V).
4. Lymphatics
- Afferent lymphatics drain into parotid group of lymph nodes.
- Efferent lymphatics drain to jugulodigastric group of deep cervical lymph nodes.
5. Nerve supply
Gland
Sensory:
- Gland: Auriculotemporal nerve, a branch of mandibular nerve.
- Parotid fascia: Great auricular nerve(C2, C3).
Motor
- Secretomotor:(parasympathetic):
- Preganglionic fires arise from inferior salivatory nucleus. It travels via glossopharyngeal nerve-tympanic branch of glossopharyngeal nerve tympanic plexus-lesser petrosal nerve-otic ganglion-fires relay.
- Postganglionic: Auriculotemporal nerve-parotid gland.
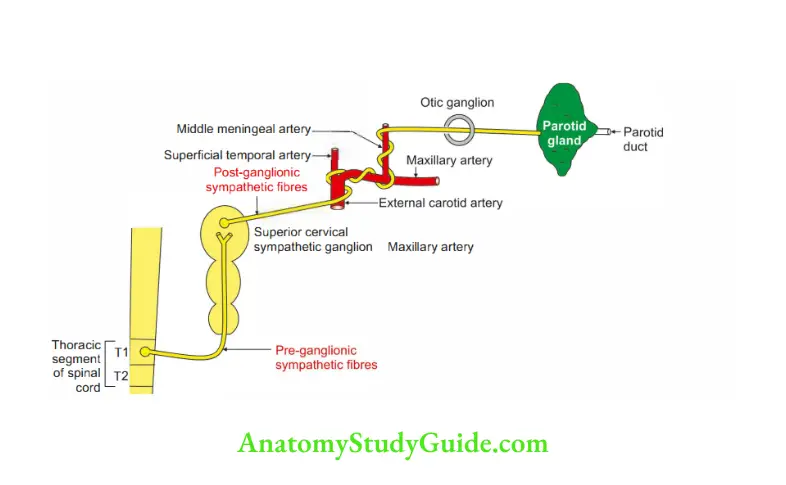
2. Vasomotor (sympathetic)
- Preganglionic fibres arise from thoracic segment of spinal cord>Superior cervical sympathetic ganglion.
- Postganglionic: Plexus around external carotid artery > middle meningeal artery to parotid gland.
Pes anserinus (pes-a foot, anser-goose): Branches of the facial nerve in the substance of parotid gland form a network called pes anserinus.
This divides the parotid gland into superficial and deep parts.
6. Applied anatomy
- Parotitis: Inflammation of parotid gland is very painful due to unyielding nature of parotid fascia. Mumps is a viral infection of parotid gland, which is usually bilateral and self-limiting.
There are no complications in children because gonads are not developed i children.
If it occurs in adult, the complications are oophoritis in females. orchitis in males C ‘and pancreatitis in both sexes. - Parotid abscess is drained by taking transverse incision over parotid gland to avoid injury to the branches of facial nerve (Hilton’s method).
- Mixed parotid tumour: It is most common neoplasm of parotid gland. It is slow growing, benign painless tumour and does not involve facial nerve.
- Frey’s syndrome: Sometimes penetrating wound of parotid gland damages auriculotemporal nerve and great auricular nerve.
During regeneration, auriculotemporal nerve joins with great auricular nerve.
Therefore, stimulation of auricular temporal nerve stimulates great auricular nerve.
This results into sweating over the parotid region. The condition is called Frey’s syndrome. - During partial parotidectomy, the pes anserinus helps to distinguish between superficial and deep parts of gland.
- Most common neoplasm of the parotid is a benign tumour called mixed parotid tumour. It is present in the superficial lobe and consequently may be excised by superficial lobectomy.
- Malignant parotid tumours are usually present in the deep lobe and involve facial nerve.
- In removing a benign mixed salivary tumour of the parotid, the facial nerve is exposed. It is exposed posteriorly in the wedge-shaped space.
The space is present between the bony canal of the external auditory meatus and the mastoid process.
The facial nerve is traced into the gland.
The mai divisions are identified and the tumour is excised with a wide margin of normal gland. The care should (be taken to preserve the exposed nerves). - It is interesting that giant mixed tumours can be excised with an adequate margin without even seeing the facial nerve.
Parotid duct (Stenson’s duct)
Introduction: It is thick-walled tube, which carries secretion of parotid gland to -o’
vestibule of mouth.
1. Formation: By union of two vertical ducts (formed by ductules).
2. Shape of crow quill.
3. Length: 5 cm, width: 3 mm.
4. Course
Begins from middle of anterior border of parotid gland.
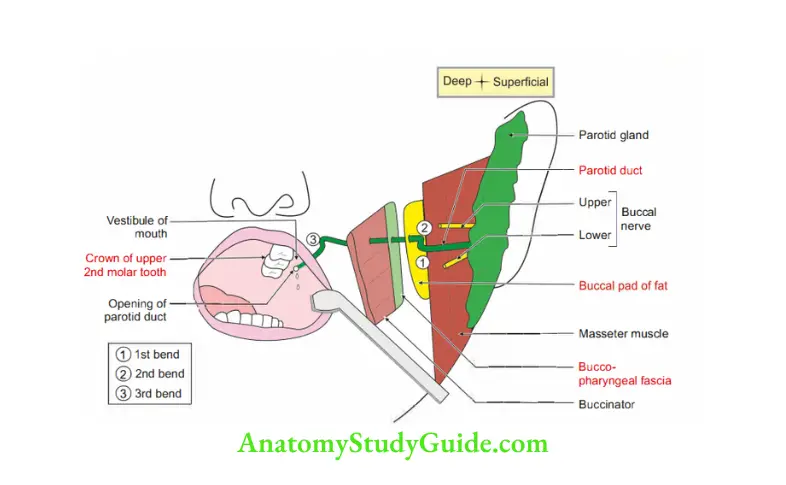
- Runs on masseter muscle. It has three bends.
- 1st bend: It directs medially at the anterior border of masseter and pierces (3B) Buccal pad of fat, Buccopharyngeal fascia and Buccinator muscle.
Structures piercing buccinator are
1. Parotid duct
2. Buccal nerve, branch of mandibular nerve-sensory to the skin over buccinator
- 2nd bend: It is between Buccinator and Buccal mucous membrane of oral cavity.
- 3rd bend: It pierces mucous membrane and enters vestibule of mouth.
Ends by opening on the
- Summit of raised papilla.
- Opposite the crown of upper 2nd molar tooth.
- Within vestibule of mouth.
Associate memory: Events at upper 2nd molar teeth
1. Opening of parotid duct, and
2. Modiolus.
5. Structure
Outer fibroelastic coat and smooth muscle.
Inner mucous membrane which is lined by stratified cuboidal epithelium.
6. Blood supply:
1. Arterial supply:
- Glandular branches of transverse facial artery, a branch of superficial temporal artery.
- Glandular branches of posterior auricular artery.
2. Venous drainage: Veins draining parotid gland drain into
- External jugular vein, and
- Internal jugular vein.
7. Lymphatics: Superficial and deep cervical group of lymph nodes.
8. Nerve supply: Auriculotemporal nerve, branch of posterior division of mandibular nerve.
9. Development
- Genn layer: Ectoderm
- Source: Stomodeum.
- Site: Furrow between the mandibular and maxillary arches at the site of future angle of mouth.
10. Applied anatomy
- Oblique passage of duct between mucous membrane and the buccinator serves as a valve-like mechanism and prevents inflation of the duct during violent blowing.
- Parotid duct is palpated and rolled on the firm anterior edge of masseter muscle.
Leave a Reply