Micturition
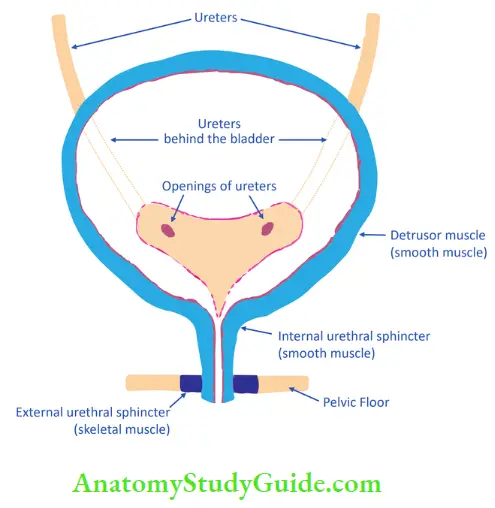
Table of Contents
The urinary bladder collects and stores urine till urination. Urine enters the bladder through the ureters and exits via the urethra. Urethra has two sphincters internal and external.
Micturition is controlled by 3 muscles
- Depressor muscles – Muscles of the bladder
- Internal urethral sphincter
- External urethral sphincter
During bladder filling phase derisory muscles relaxes and sphincters are contracted
During micturition, detrusory muscles contract, and sphincters are relaxed

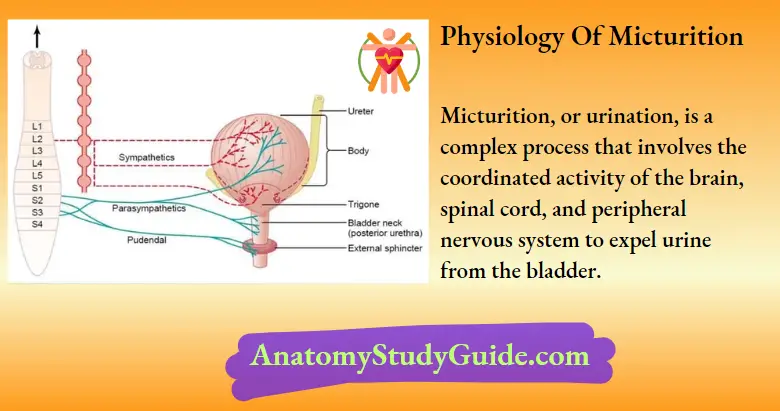
Physiology of Micturition
It is the process of emptying a filled bladder. It can be studied under two headings.
Filling of bladder
- Transport of urine through ureters- Urine flow from collecting ducts into renal calyces. Stretching of calyces stimulates pacemaker activity and initiates peristaltic contractions, which move along the ureters and carry urine in the bladder. Peristaltic contractions are stimulated by parasympathetic and inhibited by sympathetic stimulations. The peristaltic wave travels at a rate of 3 cm/second and occurs at intervals of 2-3 minutes.
- Bladder capacity
- Physiological capacity: 600 ml in adults
- Anatomical Capacity > 1000 ml in adults (Capacity beyond which bladder ruptures)
- Volume and pressure changes in the bladder
At rest, empty bladder pressure equals to intra-abdominal pressure. As the bladder starts filling, bladder tone decreases, and to accommodate urine without increasing pressure. It is because of the proper of plasticity of smooth muscles. The intravesical pressure and volume are studied by the process of cytometry and the graph is known as cystometogram. The x-axis is the volume of urine in ml and the y-axis is the intravesical pressure in cm of H2O. Cystometric analysis is used to assess the bladder’s capacity to contract and void urine.
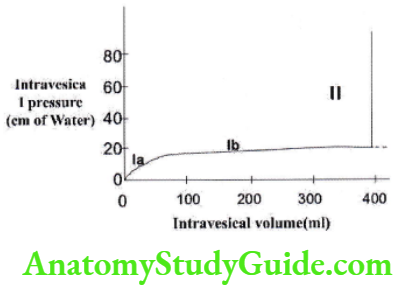

Phase 1a:– bladder volume increases till 50 ml with minimal rise of Pressure up to 5 cm H2O.
Phase 1b:- This part or graph elicits the property of plasticity of smooth muscle. It follows Laplace Laws, which state that, pressure in a hollow organ ls inversely proportional to the radius of the organ. Pressure = Tension /Radius. In a bladder as volume increases, the radius also increases, therefore the pressure decreases or remains constant. So in this phase, volume increases significantly till 400m1, with minimal rise of pressure of 10cm H2O.
Phase 2:- in this phase bladder has reached its maximum capacity and then pressure starts to rise sharply, triggering the Micturition reflex.
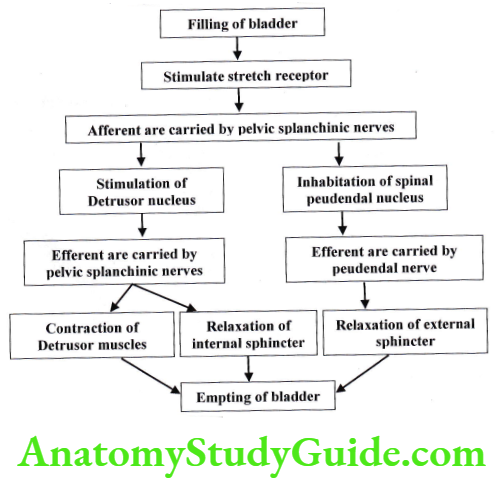
Emptying of bladder
Micturition Reflex:
If is a spinal reflex. It is controlled by a supra spinal center. The micturition reflex is self-regenerative. It repeats till the reflex fatigue and bladder relax. The reflex remains inhibited for few minutes to 1 hour. As bladder pressure increases, the reflex becomes more powerful, and then it stimulates another reflex that passes through the pudendal to the external sphincter to inhibit it.
- Inhibition to external sphincter > voluntary control = Micturition occurs
- Inhibition to external sphincter < voluntary control = Micturition doesn’t occur and the cycle repeats till urination.
Role of supra spinal centers:-
- Co-ordination center:- Barrington Center in pons, which coordinates bladder contraction with external sphincter relaxation. Its lesion leads to detrusor sphincter dyssynergia.
- Facilitator centers:- It is present in the Limbic system and superior frontal gyrus
- Inhibitory centers:- It is present in basal ganglia, so in Parkinsonism, detrusor function deteriorates.
Role of abdominal and Perineal muscles – at the onset of micturition
- Abdominal muscles contracts
- Diaphragm descends
- Levator ani and perianal muscles relax
Voluntary urination:-

Leave a Reply