Radiation Biology Essay Questions
Question 1. Describe the effects of radiation on various biological systems.
(or)
Describe the biological changes following radiation exposure.
(or)
Write about the radiation-induced changes in different body structures.
Answer: Radiation acts on biological systems through direct and indirect effects and produces free radicals.
Table of Contents
Direct effects: Biological molecules are ionized following radiation. The resulting free radicals alter the original molecules and create biological changes.
- RH (original molecule) + X-ray photon→ R0 + H+ + e–
- R0 = Free radical
Read And Learn More: Oral Medicine and Radiology Question And Answers
Indirect effects: Radiation exposure results in the radiolysis of water leading to the formation of free radicals and oxidizing toxins like peroxyl radicals and hydrogen peroxide which in turn causes biological changes and cellular destructions.
These free radicals and toxins affect:
- Biological molecules
- Intercellular structures
- Cell kinetics
- Tissues and organs.
Effects on Biomolecules:
Nucleic acids: Radiation targets the DNA of nucleic acids and produces:
- Changes or loss of a base
- Disruption of hydrogen bonding
- Breakage of DNA strands
- Cross-linking of DNA strands.
Proteins: Radiation exposure alters the secondary and tertiary structures of proteins leading to denaturation. Enzymes get inactivated and failed to participate in biological reactions. A moderate amount of radiation dose (2-4 Gray) is required to induce protein denaturation.
Effects at the Intracellular Level:
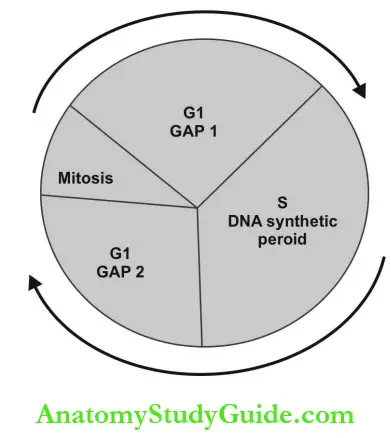
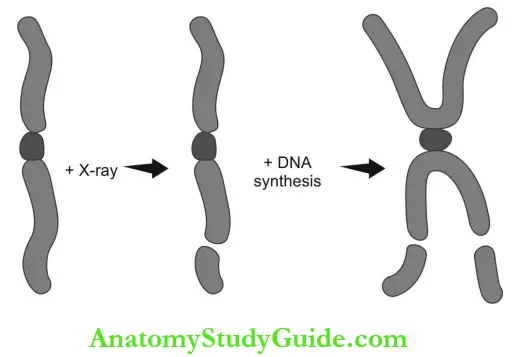
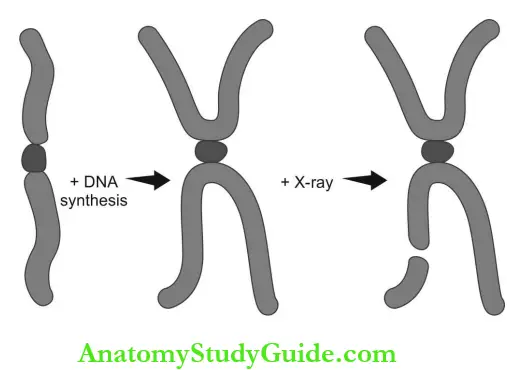
Chromosomal aberrations: During mitosis, DNA condenses to form chromosomes. When radiation exposure occurs after DNA synthesis (in G2, mid and late S—late mitosis), chromatic aberration (single arm breakage) is the result.
Chromosomal aberration (double arm breakage) occurs if exposure happened before DNA synthesis in G1 or early S phase. Chromosomal aberrations are noticeable in peripheral blood lymphocytes and serve as markers to identify the extent of radiation damage.
Cytoplasm: Larger doses of radiation (30-50 Gray) cause mitochondrial damage in rapidly dividing cells.
Changes in Cell Kinetics:
- A mitotic delay occurs on rapidly dividing cells following irradiation.
- A moderate dose causes longer mitotic delay resulting in smaller-sized cells and some cell death. Larger doses produce severe mitotic delay with loss of dividing capacity and cell death.
Effects on Tissues and Organs: Depending on the response to radiation, tissues, and organs are classified as radiosensitive and radioresistant. These results further depend on the dose and quantity of cell death.
Tissues and Organs’ Response to Radiation: Based on their radiation response, various tissues, and organs are classified as highly radiosensitive, intermediate radiosensitive, and radioresistant.

Question 2. Describe the effects of radiation on oral and para oral structures.
(or)
Describe the hazards of therapeutic radiation on oral and para oral structures.
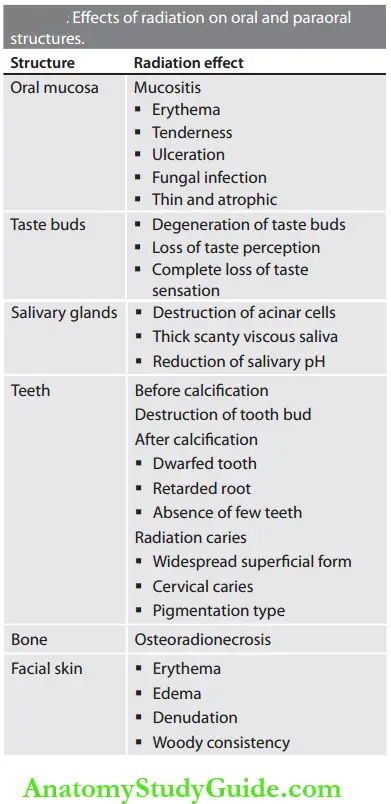
Answer: Radiotherapy induces deterministic effects on the oral cavity. The following hazardous effects are expected for the total dose of 50 Gy over 5 weeks.
Oral Mucosa:
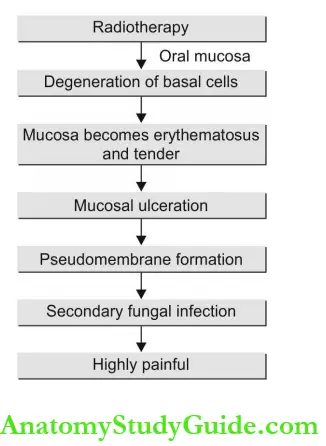
Mucositis: After 2 weeks of radiotherapy, oral mucosa becomes erythematosus and tender. If therapy is continued, the mucous membrane breaks down and forms ulcers, covered by the yellow pseudomembranous slough.
- It is a highly painful condition. Opportunistic local fungal infection is common at this stage.
- Long-term effects occur due to the gradual obliteration of the blood vessels and fibrosis of the connective tissues. The mucosa becomes thin, atrophic, and avascular.
Mucositis Medical Management:
- Pain can be managed with nonopioid anal¬gesics alone or in combination with opioids.
- Topical anesthetic agents like benzydamine hydrochloride and an antifungal lozenge containing polymixin, tobramycin, and am- photericin-b will be effective.
Effects on Oral Mucosa:
Taste Buds:
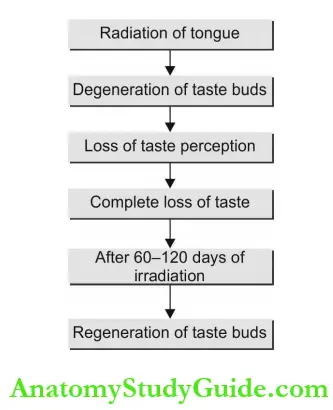
- Radiotherapy causes severe degeneration of the taste buds. Patients experience loss of taste sensation at the second or third week.
- Taste sensitivity may decrease by 1,000-10,000 times that of normal and may lead to a state of near insensitivity. Taste sensation may regain between 60-120 days.
Effects on Taste Buds:
Salivary Glands:
- When major salivary glands are exposed to radiation, progressive reduction in salivary secretion occurs.
- The total dose of 6,000 Gy for 5 weeks causes irreversible effects like necrosis of serous cells, vascular atrophy, and progressive fibrosis of the gland leading to 50% reduction in total secretion.
- Thick, viscous secretion leads to dryness of the mouth. Salivary PH is reduced. After 6-12 months of radiotherapy, the salivary flow rate is improved. Xerostomia persisting for more than a year has less chance for recovery.
Salivary Glands Medical Management: The use of sialagogues like pilocarpine 15 mg/day will stimulate salivary secretion.
Teeth: Radiation effects on teeth vary according to the developmental stage.
- If radiotherapy is indicated.
- Before calcification: It may destroy the tooth bud.
- After calcification: Dwarfed tooth, retarded root or failure to form one or few teeth. Adult teeth are resistant to radiotherapy.
Radiation Caries:
Radiation Definition: Radiation caries develop in patients who have undergone radiotherapy in the head and neck region that includes exposure to salivary glands. Salivary changes like reduced flow, decreased PH, reduced buffering capacity and high viscosity initiates a rampant carious lesion.
Classification of Radiation-Induced Caries:
- Widespread superficial form: Most common type. It affects palatal, lingual, buccal, occlusal, and incisal surfaces.
- Cervical caries: Cementum and dentin in the cervical region get affected. The lesion may progress circumferentially around the teeth resulting in loss of the crown.
- Pigmentation type: Dark pigmentation of the entire crown. The incisal margin may wear out.
Radiation-Induced Caries Management:
- Avoidance of dietary sucrose
- Daily topical application of 1% neutral sodium fluoride gel.
- Good oral hygiene and restorative procedures.
Bone:
- Irradiation of mandible causes:
- Obliteration of periosteal vasculatures
- Destruction of osteoblasts and osteoclasts
- Replacement of marrow with fat and fibrous connective tissues.
- These changes result in:
- Hypovascular, hypocellular, hypoxic marrow tissues
- Endosteal atrophy
- Empty lacunae of compact bone and brittle-ness.
Postradiation osteoradionecrosis (PRON): PRON is the severe complication following irradiation.
Management: Hyperbaric oxygen therapy.
Facial Skin: Erythema is the early sign that fads quickly. Later changes cause progressive fibrosis and give a woody consistency.
Summary:
Radiation produces adverse effects on oral structures which depend on the duration, frequency, and dose of radiation therapy. The response of different oral structures also varies in severity.
Radiation Biology Short Notes
Question 1. Describe the deterministic effects of radiation.
(or)
Describe the nonstochastic radiation effects.
Answer:
The biological effects of ionizing radiation are broadly classified into two forms:
- Deterministic effects (or) nonstochastic effects
- Stochastic effects.
Deterministic outcomes are those in which the radiation dose determines the severity of biological effects and is directionally proportional. The radiation dose has a threshold value.
- The biological effects occur in all patients receiving radiation above the threshold limit.
- When the patient’s radiation dose is less than the threshold limit, no response will occur.
Nonstochastic effects require larger doses to cause savior impairment of health.
Radiation Effects Examples:
- Oral changes following radiotherapy.
- Acute radiation syndrome following whole body irradiation.
- Cataract formation.
Question 2. Describe the stochastic effects of radiation.
Answer: The biological effects of ionizing radiation are broadly classified into two forms.
- Deterministic effects
- Stochastic effects
- In stochastic effects, the radiation dose determines the probability for developing a biological effect rather than the severity of the effects.
- The radiation dose determines the adverse incidence
- Stochastic effects follow all or none law. Following radiation, a person either has or does not have adverse effects.
Stochastic effects of radiation Examples:
- Radiation-induced cancer
- Increased radiation exposure to a person or population increases only the probability of cancer and not its severity.
Question 3. Classify the cell types based on their response to radiation.
(or)
Write the classification of mammalian cells based on radiosensitivity.
(or)
Categorize the radioresponse of different cells.
Answer: Different cells of the same individual respond differently to radiation.
1. Vegetative intermitotic cells:
- These are the most radiosensitive Examples:
- Early precursor cells like spermato- genic or erythroblastic series
- Basal cells of the oral mucous membrane
- They divide at regular intervals.
- They have long mitotic futures.
- They do not differentiate between mitoses.
- These cells retain their primitive properties and replace themselves.
2. Differentiating intermitotic cells:
- These cells are radiosensitive but slightly lesser extent than vegetative intermitotic cells Examples:
- Intermediate dividing and replicating cells of inner enamel epithelium
- Hematopoietic cells in the inter¬mediate stage of differentiation
- Spermatocytes and oocytes.
- They divide regularly but with less frequency.
- These cells undergo some differentiation between mitoses.
3. Multipotent connective tissue cells:
- These cells have intermediate radiosensitivity Examples:
- Vascular endothelial cells
- Fibroblasts
- Mesenchymal cells.
- They divide irregularly and when there is a demand for more cells.
- They undergo a limited amount of differentiation.
4. Reverting postmitotic cells:
- These cells are radioresistant Examples:
- Acinar and ductal cells of salivary glands
- Parenchymal cells of the liver, thyroid, and kidney.
- They divide infrequently.
- These cells are highly specialized in function.
5. Fixed postmitotic cells:
- Most resistant types of cells Example: Neurons, striated muscle cells, squamous epithelial cells.
- These are highly differentiated cells.
- They are incapable of the division following maturation.
Question 4. Classify the radiation response of various tissues.
(or)
Classify the organs and tissues based on their radiation response.
Answer:
- The radiosensitivity of an organ or tissue is measured by its response to irradiation. If radiation induces a small amount of cell death in an organ, they undergo repair, and usually, there will not be any clinical effects.
- If it induces more cell death, there will be strong clinical damage to the organ. The severities of the changes are dose-dependent.
Question 5. What are the factors that modify the radioresponse of cells?
(or)
What are the factors that alter the cellular responses to radiation?
Answer:
The variation in exposure parameters of radiation and cellular environment may alter the radioresponse of cells.
- Dose: The deterministic effects of radiation are dose-dependent.
- If the total dose absorbed by an organ is less than the threshold limit, no adverse effects occur.
- If the total dose exceeds the threshold value, adverse effects occur in proportion to the dose received.
- Dose rate: Dose rate indicates the number of exposures in which the total dose is deli¬vered.
- Exposure of a given dose at a high rate cause more severe biological damage than the same dose if given at a lower rate. A lower dose rate allows for the repair of damage and thereby less total damage.
- Oxygen: When radiation occurs at a hypoxic condition, cellular resistance to radiation increases by two to three times. The presence of oxygen during irradiation leads to the production of toxins and free radicals like hydrogen peroxide and hydroperoxyl radicals.
- Linear energy transfer (LET): LET is the amount of radiation energy transferred to tissues per distance traveled in that tissue. If the radiation has high linear energy like alpha particles, they deposit most of their ionizing energy in the small volume of tissues and induce more biological damage.
The high LET of alpha particles results in greater ionization density and double strand breakage of DNA and so more severe biological damage than X-rays.
Question 6. What is osteoradionecrosis?
Answer:
Osteoradionecrosis is a pathological process of bone necrosis following radiation exposure. The bone becomes devitalized (sequestration) and is complicated by pain and infection. The mandible is affected more commonly than the maxilla due to its sparse vascularity.
Three etiological factors are recognized: Radiation, trauma, and infection.
- Following radiation, the blood vessels are obliterated. The cellular marrow is repla¬ced with fibrous tissues and infiltered by inflammatory cells resulting in hypoxic, hypovascular, and hypocellular marrow. The devitalized bone may undergo sequestration.
- Hypervascularity increases the risk of infection. Microorganisms reach the bone from the radiation-induced breakdown of the oral mucosa. This infection causes a nonhealing wound in the irradiated bone.
- The other possible cause is given by, “ radiation-induced fibro atrophic theory”—the increased formation of fibroblasts and scar tissues at the irradiated bone.
- A dose of radiation less than 6,500 rads reduces the risk of osteoradionecrosis and radiation therapy above 7,500 rads will significantly increase the chance.
Osteoradionecrosis Preventive Metods:
- Avoid irradiation of bone which has been subjected to previous surgery or extraction and the healing is incomplete.
- Avoid irradiation of lesions near the bone.
- Avoid high doses of radiation.
- Surgery in the irradiated area.
- Avoid trauma in the irradiated region.
Osteoradionecrosis Management:
- Good oral hygiene
- Hyperbaric oxygen therapy
- Antibiotics
- Nutritional supplements.
Question 7. What is acute radiation syndrome?
(or)
Write about the effects of whole-body irradiation.
Answer:
Acute radiation syndrome is a group of signs and symptoms experienced by a person after exposure to a high amount of radiation at a short time like atom bomb blast or radiation accident.
Whole body irradiation Prodromal period:
- Whole-body irradiation of about 1.2 Gy produces symptoms within minutes to hours.
- Early symptoms include nausea, vomiting, diarrhea, weakness, and fatigue.
- The autonomous nervous system causes these effects.
- The severity and time of onset of the symp-toms are dose-dependent.
Whole body irradiation Latent period:
- It is the period between the irradiation and the occurrence of biological damage.
- This period extends for hours to days if the dose is above 5 Gy and for a few weeks if the dose is less than 2 Gy.
Hematopoietic syndrome:
- Exposure of 2-7 Gy affects hematopoietic stem cells. There will be a rapid reduction in the circulating granulocytes, platelets, and erythrocytes. The clinical findings include infection, bleeding, and anemia.
- Periodontitis is the associated dental complication.
- Gastrointestinal syndrome: Exposure of 7-15 Gy causes injury to intestinal villi and denudation of mucosal epithelium. This leads to mucosal ulceration, hemorrhaging of the intestine, diarrhea, dehydration, weight loss, and septicemia.
- Cardiovascular and central nervous syndrome: Exposure of 50 Gy cause death in 1-2 days due to collapse of the circulatory system, fall in blood pressure, and necrosis of cardiac muscles. Damage to the nervous system causes disorientation and convulsions. The syndrome is irreversible.
Question 8. Write about the direct effects of radiation on living systems.
Answer:
- Ionization of biomolecules by X-ray photons or secondary electrons is defined as the direct effects of radiation.
- When the biological molecules absorb the energy of X-ray photons, ionization begins, and free radical formation takes place by the production of unpaired electrons.
- These free radicals are highly reactive and highly unstable and hence quickly reforms into a stable form by dissociation or cross¬linkage.
- One-third of biological reactions following radiation is through direct effects.
Radiation on living systems Example:
When a biomolecule RH absorbs the energy of an X-ray photon, free radicals are produced as follows:
- RH + X-ray absorption →R0 + H+ + e–Free radical R undergo either:
- Dissociation: R0 →X + Y0
- Cross-linking: R0 + Y0 → RY
As the altered molecules are differing from the original molecule, there is a biological change in the organism.
Question 9. Write about the indirect effects of radia¬tion on living systems.
Answer:
- During radiation exposure, water molecules of the body absorb energy and undergo ionization. The resulting free radicals react with biomolecules and produce changes. This type of reaction is called the indirect effect of radiation.
- Two-thirds of radiation-induced biological effects occur with indirect effects.
- Radiolysis of water: Interaction of radiation with water causes ionization of water molecules and release of free radicals like hydrogen (H+) and hydroxyl ions (OH–).

- These free radicals produce damage to the biological molecules by either directly interacting with them or by producing toxins like peroxyl radicals and hydrogen peroxide. These products alter the chemical and biological properties of the biomolecule resulting in either death or malignant transformation of these molecules.
Question 10. Write about radiation-induced cancers.
Answer: Radiation-induced cancers occur commonly in a population exposed to high amounts of radiation like atomic bomb survivors. Children are approximately twice as radiosensitive for cancer induction as adults.
The role of radiation on cancer induction is likely to be:
- An irritating that produces changes in the cell differentiation mechanism
- An Inducing agent for gene mutation
- Promoter for cell multiplication.
Susceptibility of Different Organs to Radiation-Induced Cancer: Based on the radiation susceptibility to cancer, the organs are classified as highly susceptible, moderately susceptible, and less susceptible.

Question 11. Hyperbaric oxygen therapy.
Answer:
- Hyperbaric oxygen therapy is employed in the treatment of many conditions like gangrene, osteoradionecrosis, necrotizing fasciitis, and infections like actinomycosis that devitalize the cells and tissues. The patient is placed in a treatment chamber (above 1 atmospheric pressure) and allowed to breathe 100% oxygen.
- The elevated level of oxygen stimulates vaso¬constriction and allows the peripheral blood towards the hypoxic tissues. The increased blood supply enhances new angiogenesis and epithelization which in turn prevents infection and supports healing.
- Hyperbaric oxygen therapy Side effects: Oxygen toxicity can cause seizures, barotrauma (collapse due to alteration in lung pressure), myopia, and fluid leakage from the middle ear.
- Hyperbaric oxygen therapy Contraindications: Diabetes mellitus and thyroid disorders may increase the chances of oxygen toxicity.
Radiation Biology Viva Voce
Question 1. What is the threshold dose?
Answer: The amount of radiation that produces visible biological damage is known as the threshold dose.
Question 2. What is a doubling dose?
Answer:
- This is the amount of radiation required by a population to produce many spontaneous additional mutations in the next generation.
- Doubling the dose helps to measure the genetic exposure risk of radiation.
Question 3. Define radiation caries.
Answer: It is a rampant form of caries with widespread attack and rapid onset. Salivary changes following radiotherapy like reduced flow, decreased pH, increased viscosity, and less cleansing action induce caries.
Question 4. What are the accumulative effects of radiation?
Answer:
- Whenever biological tissues are exposed to radiation, there is some injury and is followed by repair.
- But residual injury may remain within DNA or cytoplasm and each succeeding radiation injury adds a small amount to this residual damage and is known as the accumulative effect of radiation and lead to future health problems.
Question 5. What are the host factors that influence radiation effects?
Answer: Intrinsic resistance, type and sensitivity of tissues exposed, rate of cell division, and phase of the cell cycle.
Question 6. Why radiotherapy is indicated for malignancy.
Answer: The rate of cell division determines the biological effects of radiation. Hence, malignant cells that divide rapidly are destroyed by radiation.
Radiation Biology Highlights
This section enlightens the effects of ionizing radiation on biological molecules, cells, tissues, and organs. The interactions are through the water or organic molecules and result in free radicals formation which causes cell destruction. There is wide variation among different cells and organs regarding their response and effects that may occur either immediately or progressively over a period.
Leave a Reply