Temporomandibular Joint – Structure – Function
Question. Describe the anatomy of TMJ in brief and add a note on the components of TMJ in detail.
Anatomy of TMJ Introduction
The temporomandibular joint (TMJ) or Craniomandibular joint found only in mammals is formed by the articulation of the mandibular condyle at the base of the cranium with the squamous part of the temporal bone.
Anatomy of TMJ Synonyms
- Ginglymoid joint As it provides hinging movement in forward and backward direction Biarthrodial joint As it provides gliding movement.
- Ginglymo arthrodial joint As it provides both hinging and gliding movement.
Read And Learn More: Complete Dentures Question and Answers
- Modified ball and socket joint As it allows movements in three planes (sagittal, transverse, and coronal).
- Compound joint As the articular disc functionally serves as a non-ossified bone that permits the complex movements of the joints.
Functions of TMJ
Voluntary movements such as mastication, deglutition, phonation, and reflex actions such as grasping and yawning.
Development of TMJ
- The TMJ begins to develop by the 10th week of gestation from two separate blastemas –one for the temporal bone component and one for the condyle.
- Superior to the condylar blastema a band of mesenchymal cells develops that will eventually differentiate into the disc.
- Temporal condylar mesenchymal cells differentiate into osteoblasts which lay down membrane bone, from 12–32 weeks of gestation and there is a high degree of calcification of the condylar head.
- The developing TMJ shows all components of the mature joint by the 14th week of gestation.
Histology of the articular surfaces composed of 4 distinct layers of zones:
- Articular zone Superficial layer adjacent to the joint cavity made of dense fibrous connective tissue
- Proliferative zone Undifferentiated mesenchymal tissue is responsible for the proliferation of articular cartilage in response to functional demands placed on the articular surfaces during loading.
- Fibrocartilaginous zone Collagen fibers are arranged in bundles in a crossing pattern.
- Calcified cartilage zone Deepest zone composed of chondrocytes and chondroblasts
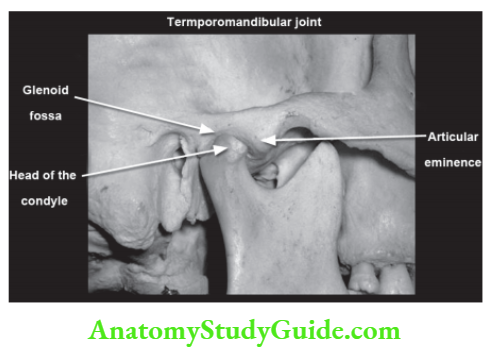
Articular eminence This is a small prominence on the zygomatic arch.
The postglenoid tubercle Separates the articular surface of the fossa laterally from a tympanic plate.
The glenoid fossa Is the anterior articular area formed by the inferior aspect of the squamous part of the temporal bone. It acts as a partition between the middle cranial fossa and the joint lined by dense avascular fibrocartilage. The posterior wall of the glenoid fossa is formed by a tympanic plate, separated by squamotympanic fissure.
Components of TMJ
- Cranial component
- Mandibular component.
Cranial Component
Are bounded anteriorly by Articular eminence and posteriorly by post-glenoid tubercle.
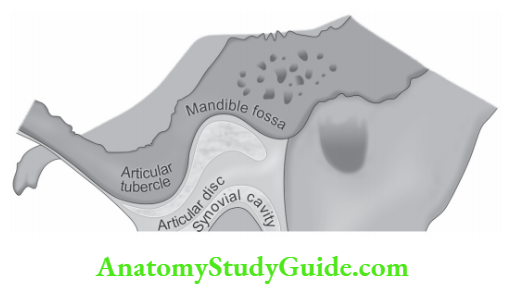
Mandibular Component
Condyle which is ovoid in shape with a narrow neck forms the articular part of the mandible. It is broad laterally and narrows medially with a mediolateral width of 13–25 mm and anteroposterior width of 5.5–16 mm. It is convex in all directions and covered by fibrocartilaginous tissue.
Clinical Anatomy of TMJ Components
- Capsule
- Ligaments of TMJ
- Glenoid fossa
- Condyle
- Articular disc (meniscus)
- Synovial membrane
- Vascular supply and innervation
- Musculature.

1. Capsule
- Fibroelastic, highly vascular, and highly innervated dense connective tissue
- Funnel-shaped, blends with the periosteum of the mandibular neck and envelops meniscus
- Laterally zygomatic tubercle, a lateral rim of glenoid fossa, post glenoid tubercle
- The medially medial rim of the glenoid fossa (closely related to the spine of sphenoid
- Sphenomandibular ligament, middle meningeal artery passing through foramen spinosum
- Anteriorly anterior border of the articular eminence
- Posteriorly squamotympanic fissure and fuses with a superior stratum of the post-bilaminar zone (b/w post-capsule and post-glenoid tubercle-highly vascular tissue)
- Superiorly circumference of the cranial articulating surface
- Inferiorly neck of the condyle
- Inside lined by silky synovial membrane.
2. Ligaments
- These are composed of collagenous connective tissue and act predominantly as restraints to the motion of the condyle and the disc.
- The three functional ligaments are Collateral ligaments, Capsular ligaments, and Temporomandibular ligaments. The two accessory ligaments are the Sphenomandibular ligament and the Stylomandibular ligament.
3. Articular Disc
- Dense, non-vascular, non-innervated fibrous connective tissue
- Biconcave in sagittal section
- Anatomically divided into three zones
- Anterior band.
- Central intermediate zone (Thinnest)
- Posterior band (Thicker)
- The intermediate zone is the area of function between the mandibular condyle and temporal bone.
- The articular disc is attached to the capsular ligament anteriorly, posteriorly, medially, and laterally. Anterior attachment of the meniscus is contiguous with the lateral pterygoid muscle
- Retrodiscal tissue Posteriorly tissues are highly vascularized and innervated – bilaminar zone (involved in the production of synovial fluid).
4. The articular disc divides the joint into the superior and inferior compartment
Superior compartment (temporodiscal complex)
- Permits translational movements
- Larger of the two compartments but less reinforced
- Extends further anteriorly than lower joint space
- Has a synovial fluid volume of 1.2 ml.
5. Inferior compartment (condylodiscal complex)
- Permits rotatory movements
- Smaller, more tightly reinforced by disc attachments
- Has a synovial fluid volume of 0.9 ml.
6. Synovial membrane
- Lines the joint spaces
- Responsible for secreting synovial fluid (nutrition and lubrication)
- Extremely thin, smooth connective tissue membrane
- Cells in the synovial membrane have the ability to differentiate into chondrocytes.
The synovial fluid serves two purposes
- Synovial fluid acts as a medium for providing metabolic requirements.
- Serves as a lubricant between articular surfaces by Boundary lubrication which is the primary mechanism of joint lubrication that prevents friction in the moving joint.
- The other mechanism is weeping lubrication by which metabolic exchange occurs and eliminates friction in the compressed but not moving joint.
7. Nerve supply
- The mandibular nerve innervates the joint.
- Three branches from the mandibular nerve send terminals to the joint capsule.
- Auriculotemporal nerve (largest) posterior, medial, and lateral part of the joint
- A branch from the posterior deep temporal nerve
- Masseteric nerve anterior part of the joint.
Leave a Reply