Structure And Function Of Kidney Introduction
The excretory system plays an important role in the elimination of waste products from the body and maintaining homeostasis. It includes various organs.
Table of Contents
- Kidney – It removes waste from the bloodstream in the form of urine.
- Liver – It detoxifies and breaks down chemicals, poisons, and other toxins that enter the body.
- Intestine – It expels the indigestible parts of food.
- Skin – It excretes sweat through sweat glands.
- Lungs – It diffuse gaseous wastes, like carbon dioxide.
In this unit we are going to learn about kidneys in detail.
Functions of kidney
The mnemonic GOA WET BED helps to memorize kidneys functions.
- G – Gluconeogenesis
- O – Maintain Osmolarity
- A – Maintain ACID-base balance
- W – Maintain water balance /Extracellular Fluid volume
- E – Electrolyte balance
- T – TOXIN removal/ urea/uric acid/ creatinine/ bilirubin/hormones
- B – BLOOD Pressure regulation
- E – ERYTHROPOIETIN synthesis
- D – Vitamin D metabolism.
Functional Anatomy of Kidney
The kidney is a bean shape, retroperitoneal organ, that lies at the T12-L1 Level. The right kidney is slightly interior to the left kidney. Weight of each kidney is 150 mg approximately. It has two poles – superior and inferior. From the central part of the kidney which is known as the hilum arises ureters and renal vein. The renal artery also enters through the hilum. Ureters originate from the funnel pelvis.
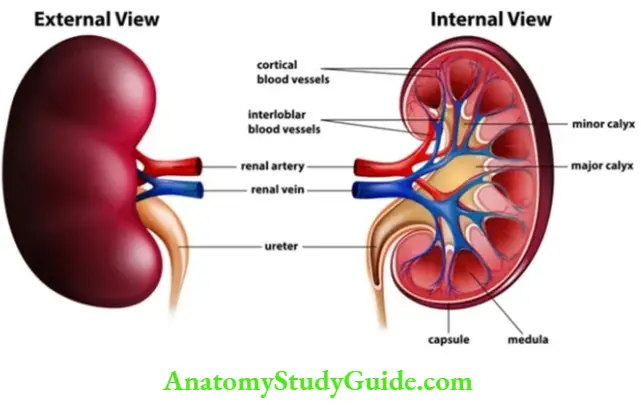
Longitudinal Section of Kidney
It shows two part of the kidney, outer part is known as the cortex and the inner part is known as the medulla. Medulla has multiple pyramidal structures known as renal pyramids. Renal pyramids terminate in renal papilla, which opens in the minor calyx. Two to three Minor calyxes terminate in the major calyx. Major calyxes open into the funnel-shaped renal pelvis, from which arises the ureter.
Each kidney has 1.3 million nephrons. The functional unit of the kidney is the nephron. It can be divided as.
- Renal / Malphagian corpuscle
- Bowmen capsule
- Glomerulus
- Renal tubule
- Proximal convoluted tubule
- Loop of Henle
- Thin descending limb (TDL)
- Ascending Thin limb (ATL)
- Thick ascending limb (TAL)
- Distal convoluted tubule
- Collecting tubule
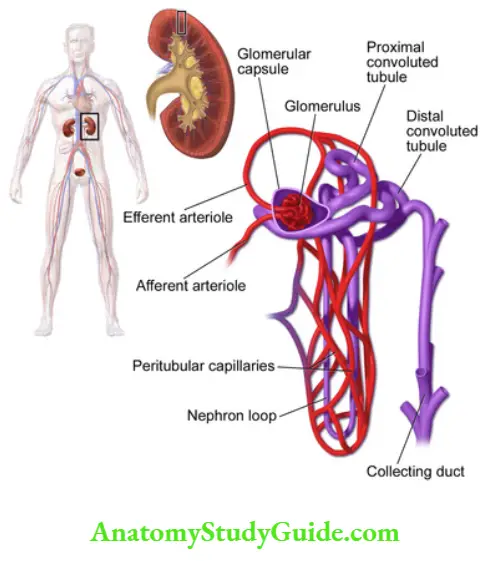
Filtration of membrane:
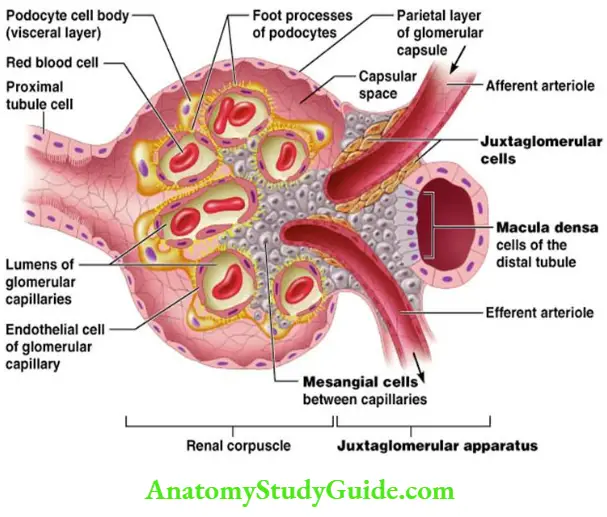
Renal corpuscles comprise of two parts bowmen capsule and glomerulus.
The Bowmen capsule is the dilated blind end of the nephron. It has two layers, visceral and parietal. The inner layer or layer near to glomerulus is called as visceral and the outer layer is known as parietal layer. The space between the visceral and parietal layers is known as bowmen’s space.
Glomerulus is a tuft of capillaries which lies in the center of the Bowmen capsule. It receives blood from afferent arterioles and blood is carried by efferent arterioles. The diameter of afferent arterioles is greater than efferent arterioles.
Ultrastructure Of Glomerular Membrane
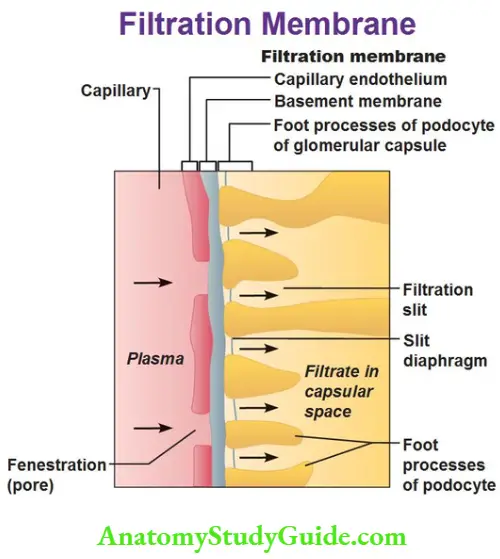
It is the membrane that separates blood of Glomerular capillaries from filtrate present in bowmen space. It is also known as filtration barrier. It has three layers.
- Capillary endothelium
- Basement membrane
- Visceral layer of bowmen capsule
capillary endothelium – It is fenestrated, with pores size 70-90nm. It is freely permeable to water, solutes, and proteins. The total area of Glomerular capillary endothelium across which filtration occurs is about 0.8m2. Sialoprotein in Glomerular capillary walls are negatively charged which inhibit the filtration of negative substances like albumin which have a diameter of 7nm.
Basement membrane / basal lamina – Its thickness is 250-400nm made of type 4 collagen. It has no pores but allow permeability of 8nm. It has three layers.
- Lamina rara external
- Lamina densa
- Lamina rara interna
Stellate cells / Mesangial cells
- They lies between the Capillary endothelium and the Basement membrane.
- They are contractile cells. They are stimulated by angiotensin 2 and relaxed by cAMP. Thus help to regulate the Glomerular filtration rate.
- They secrete an extracellular matrix which provides structural support to the Glomerular tuft.
- They are capable of proliferating.
- They remove immune complexes from blood.
- They show phagocytic activity.
Visceral layer of bowmen capsule/podocytes
They have numerous pseudopods which encircle the outer surface of capillaries. Pseudopodia interdigitates to form filtration slits of 25 nm wide along the capillaries. There foot processes have glycocalyx which is negatively charged which controls the filtration of proteins. In pathological conditions, when this negative charge is lost then protein get filtered and lost in urine.
Summary of Glomerular Membrane:
- It permits free passage of neutral substances up to 4nm.
- Filtration of cationic substance > neutral substance>anionic substance.
- Filtration is inversely proportional to diameter.
Renal tubule:
Its length varies between 45-65 mm. Cell membrane toward the tubular lumen is known as a luminal membrane. The cell membrane toward the basement membrane is known as a basal membrane. The membrane between cells is known as a lateral membrane. Basal and lateral membranes are together known as basolateral membranes.
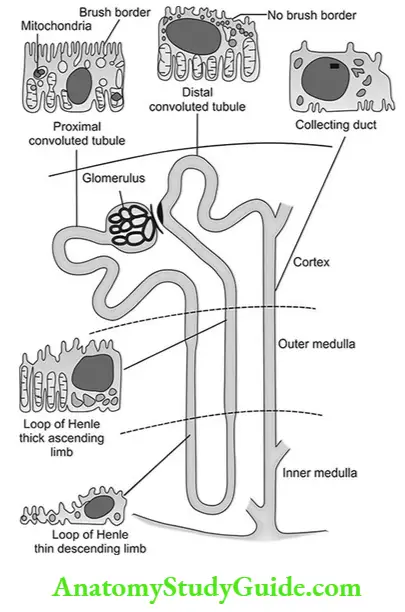
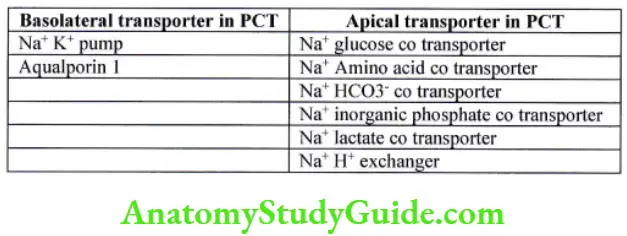
Proximal convoluted tubule/ pars recta – (PCT)
- It is initial part of the nephron, its length is 15 mm and its diameter is 55pm.
- It has a single layer of columnar epithelial cells interdigitated with each other.
- Cells are united at the apex with the leaky type of tight junction which allows water and solute to diffuse. Between cells lies lateral intercellular space.
- The luminal membrane has an extensive brush border which increases surface area up to 20 fold. It is loaded with protein carriers which help in absorption.
- Energy supply is maintained by large no of mitochondria.
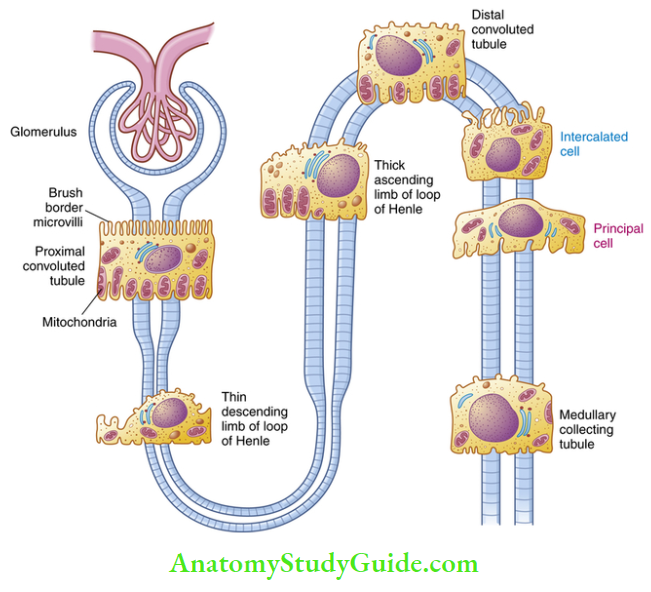
Loop of henle – It is hairpin loop which has three parts:
- Thin descending limb (TDL) – It is made up of thin permeable columnar epithelial cells
- Ascending Thin limb (ATL) – It is made up of thin permeable squamous epithelial cells
- Thick ascending limb (TAL) It is made up of thick cuboidal cells having many mitochondria. Thick ascending limb ascend to reach glomerulus of nephron between afferent and efferent arteriole, there it have specialized cells known as macula densa. It has tightly packed columnar cells which may monitor the osmolarity of blood.

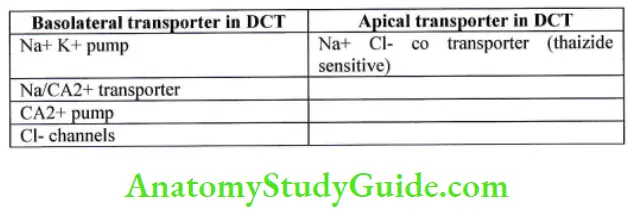
Distal convoluted tubule (DCT)
It is 5mm long, made up of Cuboidal cells. It starts at macular densa. It has no brush border. It has intercalated cells (I cells) which are concerned with acid secretion and Hco3 – transport.
Collecting tubule
DCT coalesce to form a collecting tubule, which transports the urine via the renal papillae into the renal calyx. It is 20mm long. Collecting ducts are lined with Cuboidal epithelium containing two cell types: the principle cells (P cells) and intercalated cells (I cells).
Principal cells
The principal cell in the collecting ducts plays a role in sodium reabsorption via sodium channels located on the apical membrane. Aldosterone increase sodium absorption by acting on principal cells. It also determines the expression of sodium channels.
Intercalated cells
The intercalated cells participate in acid-base balance’ They are of two types – Type A / α B/ β.

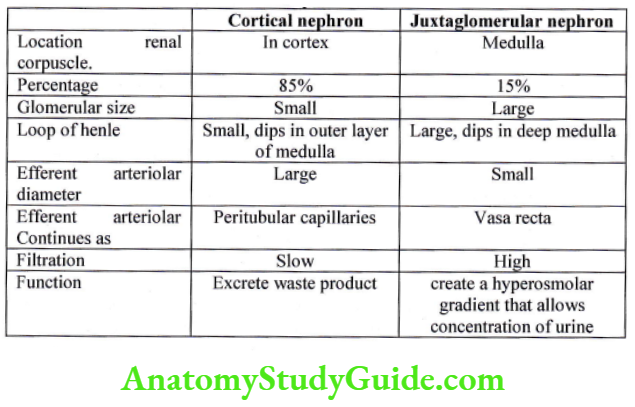
Types of nephron
Nephron are classified according to the length of loop of Henle and the location of the renal corpuscle into cortical nephron and juxtaglomerular nephron.
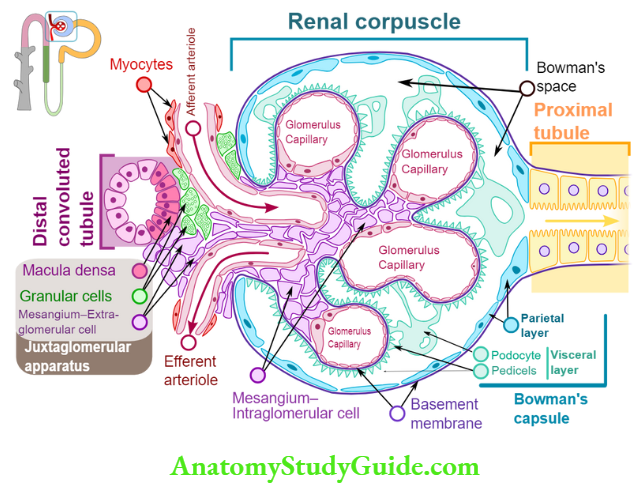
Juxtaglomerular apparatus
It consist of
- Macula densa cells of the thick ascending limb of the loop of Henle.
- Mesangial or lasic cells.
- Juxtaglomerular cells of afferent arteriole.
Macula densa cells of the thick ascending limb of the loop of Henle
when the thick ascending limb of the loop of the Henle passes between the afferent and efferent arteriole, the renal epithelial cells near the afferent arteriole get modified to form Macula densa cells. They lie adjacent to the juxtaglomerular cells of afferent arteriole. They act as a chemoreceptor. They sense a decrease in Na+ and Cl-‘ By sensing sodium and chloride levels in filtrate, they regulate Glomerular filtration rate via the tubuloglomerular feedback (TGF).
Extra glomerular Mesangial or lasic cells
They are supporting cells, lie between macula densa and JG cells’ They relay signal from macula densa to juxtaglomerular cells’
Juxtaglomerular cells of afferent arteriole
They ire rennin secreting granular myoepithelium cells. They are modified smooth muscle cells. They synthesize, store and release rehin, and activate angiotensin and angiotensin system, thus playing an important role in auto-regulation of the kidney. They act as baroreceptors – tension receptors and vascular volume receptors.
The juxtaglomerular cells secrete renin in response to:
Stimulation of the β1 adrenergic receptor when stimulated by epinephrine or norepinephrine.
Decrease in renal perfusion pressure (detected directly by the granular cells).
Decrease in NaCl concentration at the macula densa, often due to a decrease in glomerular filtration rate’
Leave a Reply