Coagulants And Anticoagulants
Coagulants Introduction
Coagulation or blood clotting is the process in which blood loses its fluidity and becomes a jelly like mass and it is a multistep process. Coagulation of blood is much more complicated and occurs through a series of reactions due to the activation of a group of substances. The substances necessary for clotting are called clotting factors or procoagulants. Although vitamin K is not directly involved in coagulation, this fat- soluble vitamin is required for the synthesis of four of the procoagulants made by the liver.
Table of Contents
The procoagulants are numbered 1 to 13 according to the order of their discovery; hence the numerical order does not reflect the reaction sequence. Tissue factor (3) and Ca2+ (4) are usually indicated by their names, rather than by numerals. Most of these factors are plasma proteins made by the liver that circulate in an inactive form in blood until mobilized.
Clotting may be initiated either by intrinsic or extrinsic pathway. Although both pathways are initiated by different mechanisms, the two converge on a common pathway that leads to clot formation. Both pathways are complex and involve numerous different proteins termed clotting factors. Intrinsic pathway is relatively a slow process and whereas extrinsic pathway is much faster.
When blood is removed from the body and placed in a glass test tube, it clots quickly. Calcium ions are required for this process. Addition of EDTA or citrate prevents clotting by binding with calcium. Clotting can be initiated in vitro at a later time by adding back an excess of calcium ions recalcified plasma will clot in 2-4min. The clotting time after recalcification can be shortened by adding an emulsion of negatively-charged phospholipids. The clotting time is further shortened to 21-32 sec by preincubation of the plasma with particulate substances such as kaolin (insoluble aluminum silicate).
The reaction initiated by kaolin, PL, and calcium is termed the activated partial thromboplastin time (aPTT) test. Alternatively, the clotting time of recalcified plasma can be shortened to 11-12 sec by adding “thromboplastin” (a saline brain extract containing tissue factor, a lipoprotein described below). The reaction initiated by thromboplastin and calcium is termed the prothrombin time (PT) test.
Many patients with inherited bleeding disorders have prolongation of the aPTT, the PT, or both. Thus, two pathways for coagulation were proposed. A patient with a prolonged aPTT and a normal PT is considered to have a defect in the “intrinsic” coagulation pathway. The name indicates that all of the components of the aPTT test, except kaolin, are “intrinsic” to the plasma.
On the other hand, a patient with a prolonged PT and a normal aPTT has a defect in the “extrinsic” coagulation pathway (tissue factor is “extrinsic” to the plasma). Prolongation of both the aPTT and the PT suggests that the defect lies in a common pathway.
Each pathway requires ionic calcium and involves the activation of a series of procoagulants, each functioning as an enzyme to activate the next procoagulant in the sequence. The intrinsic cascade (which has less in vivo significance in normal physiological circumstances than the extrinsic cascade) is initiated when contact is made between blood and exposed negatively charged surfaces.
The extrinsic pathway is initiated upon vascular injury which leads to exposure of tissue factor (TF), a sub- endothelial cell-surface glycoprotein that binds phospholipid. The two pathways converge at the activation of factor 10 to 11. Factor 11 has a role in the further activation of factor 7 to 8.
Active factor 11 hydrolyzes and activates prothrombin to thrombin. Thrombin can then activate factors 9, 8 and 5 furthering the cascade. Ultimately the role of thrombin is to convert fibrinogen to fibrin and to activate factor 13 to 14. Factor 14 (also termed transglutaminase) cross-links fibrin polymers solidifying the clot.
Anticoagulants Introduction
Anticoagulants prevent the process of clotting, but do not break a clot that has formed already. Anti coagulants are usually administered to patient with acute myocardial infarction, long term therapy after acute myocardial infarction and prophylaxis and treatment of pulmonary and venous thrombosis.
Anticoagulants Mechanism of Action
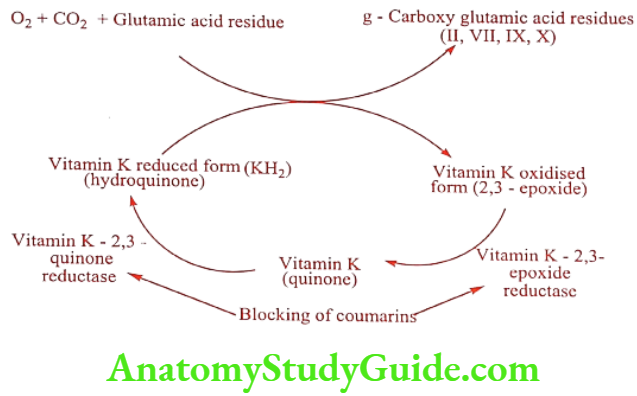
The coagulation of blood depends upon the cyclic inter conversion of Vitamin K and Vitamin K-2, 3-epoxide. Vitamin K is a co-factor necessary for the post-ribosomal synthesis of several clotting factors including 2, 7, 9 and 10. The Vitamin K sensitive step in this process involves the carboxylation of 10 or more glutamate residues on the N-terminal portions of important precursor proteins.
This carboxylation results in a new amino acid, y-carboxy glutamate, which through chelation of calcium ions causes the proteins to undergo a conformational change. This change in tertiary structure allows the four Vitamin K dependent clotting factors to bind to phospholipid membranes during clotting cascade activation.
The specific enzyme that carboxylates Vitamin K dependent coagulation factors requires reduced Vitamin K (Vitamin K hydroquinone, KH2), molecular oxygen and carbon dioxide as cofactors. In the process of this reaction, KH2, is oxidized to Vitamin K-2, 3-epoxide. The return of the epoxide to the active KH2 form is the result of a two step reduction.
First, the epoxide is reduced to Vitamin K quinone by Vitamin- K-2,3-epoxide reductase in the presence of NADH. This quinone intermediate is then further reduced back to KH2 by Vitamin K quinone reductase.
The Warfarin- like anticoagulants (i.e., Vitamin K antagonists) exert their anticoagulant activity through the inhibition of Vitamin K-2,3-epoxide reductase and possibly through inhibition of Vitamin K quinone reductase which results in inhibition of the activation of the four affected coagulation factors. In other words, the clotting factors affected are structurally incomplete and incapable of promoting the coagulation cascade.
Anticoagulants Classification
- In vivo anticoagulants: Parenteral : eg. Heparin, Danaparoid, Lepirudin.
- Oral:
- Coumarin derivatives: eg. Warfarin, Dicoumarol, Phenprocoumon.
- Indandiones : eg. Phenindione, Anisindione
- In vitro anticoagulants :eg. Heparin, Sodium oxalate, Sodium citrate, Sodium edetate.
In vivo anticoagulants
Parenteral
Heparin (Heparin sodium, Celparin)
Heparin is a naturally occurring substance in mast cell and is mainly present in lungs and liver. For therapeutic purpose it is obtained from animals like pigs and ox. It is composed of a heterogeneous mixture of sulfated mucopolysaccharides of molecular weight ranging from 5.30 KD. Heparin is an acidic molecule similar to chondroitin and hyaluronic acid. The polysaccharide polymer chains are composed of two alternating sugar unit, N-acetyl-D-glucosamine and D-glucuronic acid, linked by a 1 → 4 bonds.
Heparin inhibits blood coagulation at a different site within the coagulation cascade than the Vitamin K antagonist. Specially, Heparin accelerates binding of anti- thrombin – III to thrombin, as well as other serine protease necessary for normal blood coagulation.
ADR: Slight fever, head ache, chills, constipation and skin necrosis in case of s.c injection.
Dose: 5000U.
Use: It is used in the treatment of venous thrombosis and pulmonary embolism.
Danaparoid (Orgaran)
Danaparoid is a mixture of 84% heparin sulphate, 12% Dermatan sulphate and 4% Chondroitin sulphate. It is considered as low molecular weight heparin.
ADR: Bleeding, low platelet count and severe cases asthma exacerbation.
Dose: Administered subcutaneously at a dose of 750units twice daily.
Use: It is used for the treatment of deep venous thrombosis and for patients with heparin induced thrombocytopenia.
Oral
Coumarin derivatives
Dicoumarol (Acadyl)
Dicoumarol is a natural chemical substance obtained from both plant and fungal origin. It is a derivative of coumarin a bitter substance that does not itself affect coagulation but transformed in mouldy feeds or silages by a number of species of fungi into active Dicoumarol does affect coagulation.
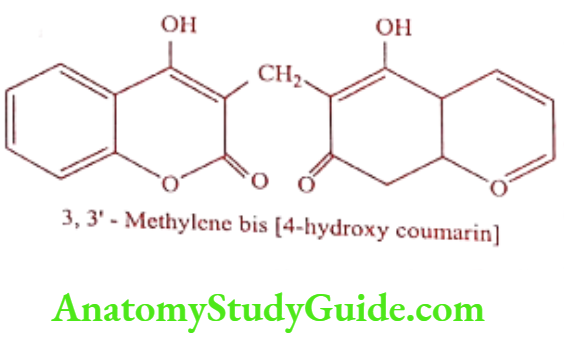
Synthesis
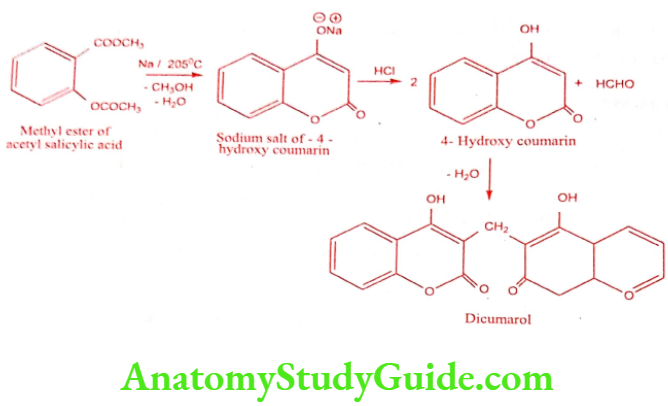
Mechanism of Action: It is not Vitamin K analogues in the classic sense. They appear to act by interfering with function of Vitamin K in liver cell, which are site of synthesis of clotting factor, including prothrombin.
ADR: Hemolysis, hematochezia, menorrhagia and clotting factor dysfunction.
Dose: 25 to 200mg/day titrated to prothrombin time.
Use: It is used alone or as an adjunct to Heparin in the prophylaxis and treatment of intravascular clotting. It is used in post operative thrombophlebitis, pulmonary embolus, and acute embolic and thrombotic occlusion of peripheral arteries.
Warfarin (Warf, Uniwarfin)
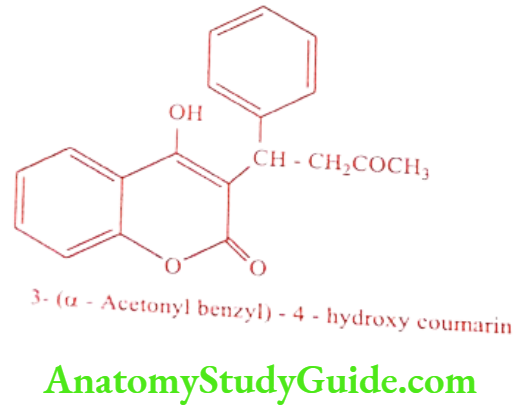
Warfarin forms a water soluble derivative in the alkalis. Warfarin sodium (Coumandin) and Warfarin potassium (Athrombin-K) they act by interfering with Vitamin K metabolism. The (-) S isomer of Warfarin is five to eight times more active than (+) R enantiomer.
Synthesis
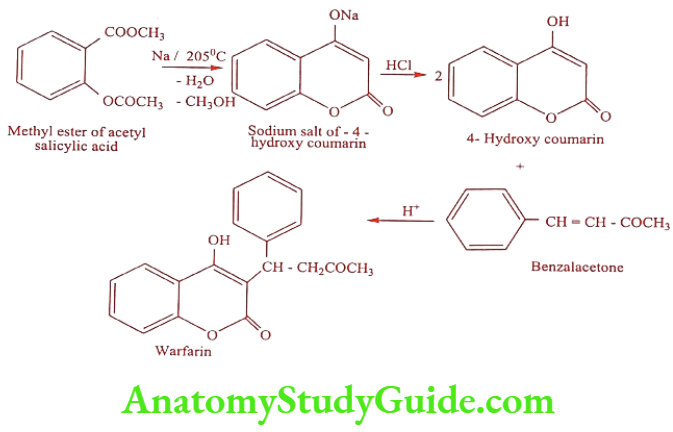
ADR: Hypersensitivity reactions, rash, alopecia and diarrhea.
Dose: 5mg daily.
Use: It is a synthetic anticoagulant and may also be used as rodenticides.
Phenprocoumon (Marcoumar, Falithrom)
Phenprocoumon is a long acting oral anticoagulant drug which is a derivative of coumarin called 4-Hydroxy coumarin. It is a Vitamin K antagonist inhibits the coagulation by blocking the synthesis of coagulation factor II, VII, IX and X.
Synthesis
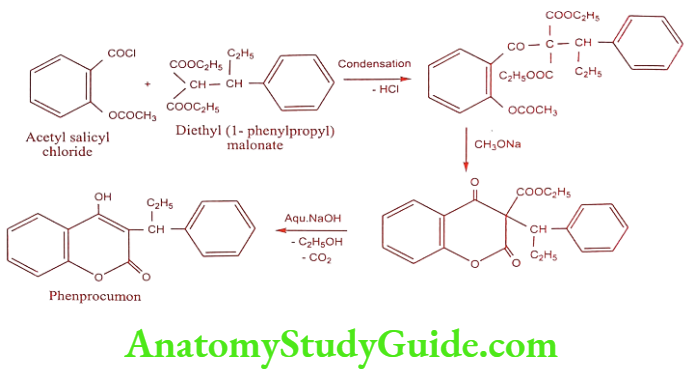
ADR: Hemorrhage, skin necrosis and hematoma.
Dose: 1.5 to 4.5mg.
Use: It is used as an oral anticoagulant.
Indandiones
Anisindione (Miradon)
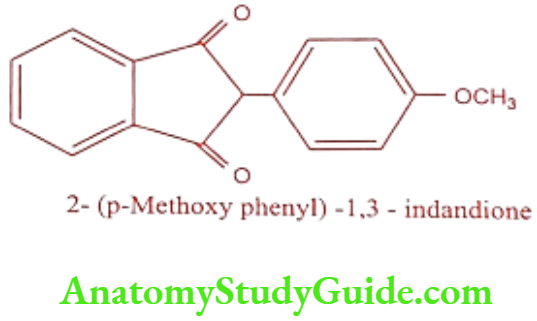
Anisindione is a synthetic anticoagulant and an indandione derivative. It prevents the formation of active procoagulation factors II, VII, IX, and X, as well as the anticoagulant proteins C and S, in the liver by inhibiting the vitamin K-mediated gamma-carboxylation of precursor proteins.
ADR: Necrosis, diarrhea and dermatitis.
Dose: 25 to 250mg/day.
Use: It is an orally active anticoagulant.
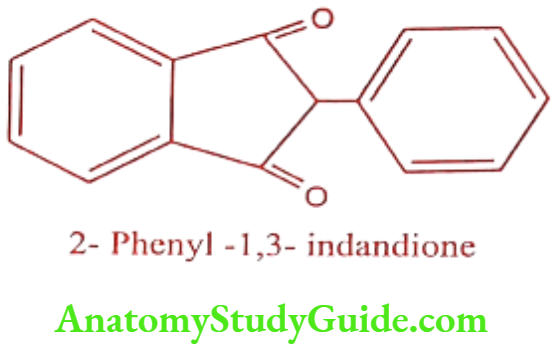
Phenindione (Pindione, Pindan)
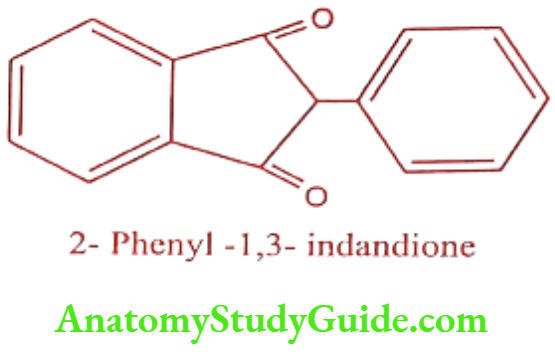
ADR: Orange urine, rash, fever and hepatitis.
Dose: Initially 200mg in two equal doses on day one followed by 100mg on day two.
Use: It is used as an oral anticoagulant.
Leave a Reply