Eyeball Anatomy Question With Answers
Question: What is glaucoma?
Table of Contents
Answer: Raised intraocular pressure is called glaucoma. It may be due to Excessive production of aqueous humour, or Lack of its drainage, or Combination of both raises the intraocular pressure.
Structure Of Eye
Question 2: What is lamina fusca of sclera?
Answer: It is thin layer of loose, pigmented cellular connective tissue. It is present in the perichoroidal space. It is delicate tissue.
It is also called suprachoroidal lamina.
Read And Learn More: Face Anatomy Notes And Important Questions
Question 3: What is retinal detachment?
Answer: It is separation of single pigmented layer from remaining layers of retina. It is actually inter-retinal detachment.
Question 4: What is fovea centralis?(Fovea a pit or depression)
Answer: 1. The centre of the macula is depressed to form the fovea centralis.
2. This is the thinnest part of the retina.
3. It contains cones only and is the site of maximum acuity (sharpness of vision).
Question 5: What is blind spot?
Answer:1. The depressed area of the optic disc is called the physiological cup.
2. It contains no rods and cones. It does not have sensory receptors, and is, therefore, insensitive to light.
3. It is the physiological blind spot.
Structure Of Eye
Question 6: What is cataract?
Answer:Increase in opacity of lens is called cataract. It occurs with increase in age.
Cornea Of Eye
Question 7: What is arcus senilis?
Answer:It is a grey or white opaque ring in the corneal margin.
It is present at birth or appears in later part of life. It is common after 50.
It results from cholesterol deposit.
Question 8: Black eye (echymosis of the eye)
Answer:1. Definition: It is small haemorrhagic spot, in the skin or mucous membrane. It is on-elevated, irregular blue or purplish patch.
2. Cause: It is the result of collection of blood in this space. It tends to gravitate in the eyelid.
It is caused
- Due to local violence causing subcutaneous extravasation of blood into th eyelids. This is the most common cause. Haemorrhage occurs soon after the receipt of an injury and black discolouration of eyelids may occur within few hours of injury.
- Fracture of the anterior cranial fossa may cause bleeding.
- Bleeding in the loose areolar tissue of scalp causes generalized swelling of the scalp. The blood may extend anteriorly into the root of the nose and into the eyelids. This is because frontalis muscle has no bony origin.
- A blow to the superciliary arches (e.g. during boxing) may lacerate the skin and cause bleeding.
Structure Of Eye
Question 9: Name the types of glands seen in eyelid. Classify them, state their mode of secretion and give their alternative names. Write the answers in a tabular form.
Answer:
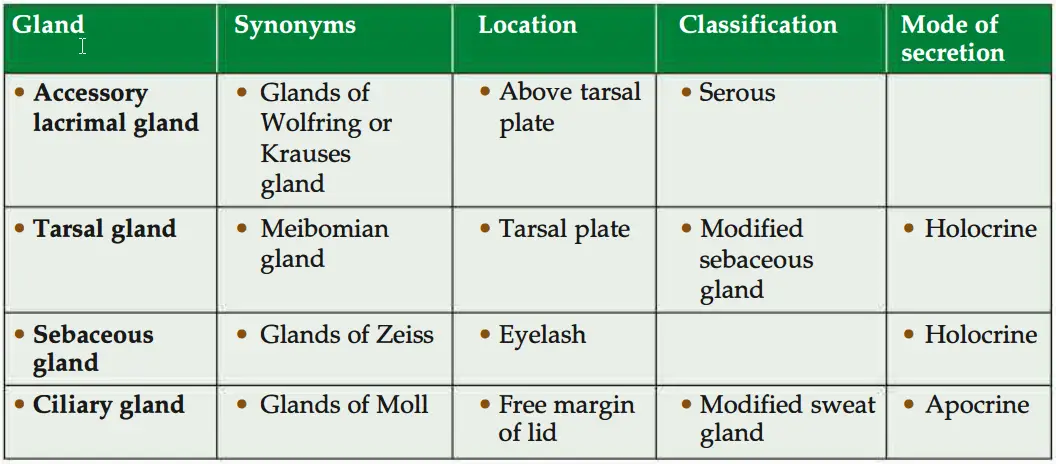
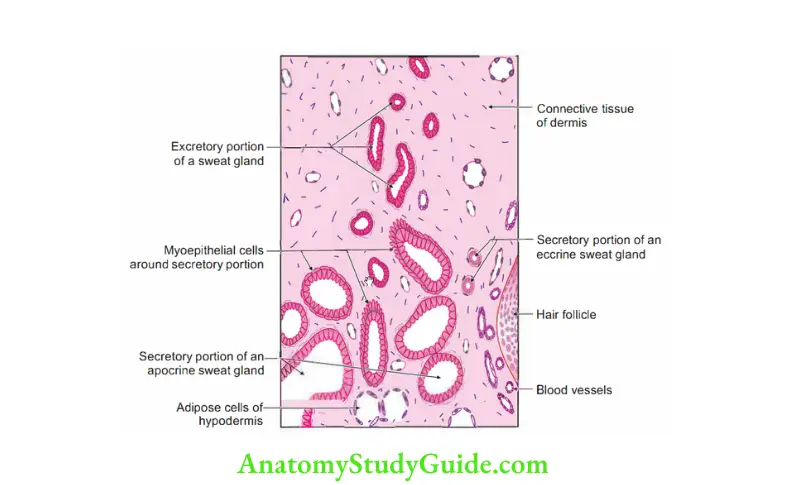
Question 10: Enumerate the types of muscles seen in eyelid.
Answer: Palpebral part of the orbicularis oculi muscle (skeletal muscle).
Orbicularis oculi
(Orbiculus-orbit, oculi-eyeball)
Introduction: It is a muscle of face, the sphincter of orbital fissure.
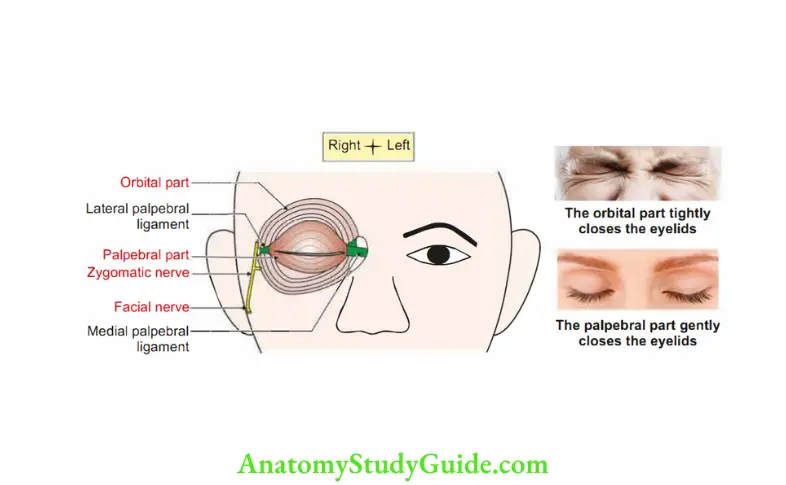
1. Attachment: It has three parts:
1. Palpebral part: It is confined to the lids. It arises from medial palpebral ligament.
It is inserted into lateral palpebral raphe.
Structure Of Eye
2. Orbital part: It extends beyond orbit. It arises from
- Nasal part of frontal bone
- Anterior lacrimal crest
- Frontal process of maxilla
- It forms concentric rings and return to the point of origin.
3. Lacrimal part (deeper part): It is attached medially to the
- Posterior lacrimal crest
- Lacrimal sac
- They are inserted into upper and lower eyelids.
2. Nerve supply
- Mainly by zygomatic branch of facial nerve.
- It is also supplied by temporal branch of facial nerve.
Cornea Of Eye
3. Actions
- Palpebral part closes the eyelid gently.
- Orbital and palpebral part together closes the eyelid forcibly.
- Levator palpebrae superioris is the opponent of upper palpebral fibres of orbicularis oculi.
Occipitofrontalis opposes the orbital part.
4. Development: They are developed from the mesoderm of the 2nd pharyngeal arch.
5. Applied anatomy: Infranuclear lesion to the facial nerve leads to paralysis of orbicularis oculi.
Hence, the patient cannot close the eyelid tightly.
Frequent closure of eyelids is required for the normal drainage of tears through the lacrimal ducts.
Due to paralysis of orbicularis oculi, there is overflowing of tears through the eyelid.
Fascial sheath of eyeball
Introduction: It is a thin fascia! sheath surrounding the eyeball and separating it from the orbital fat.
Synonym: Tenon’scapsule, fascia bulbi.
1. Attachments
- Anteriorly: Sciera just behind the comeoscleral junction.
- Posteriorly: Fused with the dura mater.
2. Structures piercing
- Optic nerve.
- Ciliary vessels, and
- Tendons of
- Four recti and
- Two obliquii
Cornea Of Eye
3. Supports of eyeball
1. Medial and lateral check ligaments: They are thickening of fascia! covering of medial and lateral recti, respectively.
2. Suspensory ligament of Lockwood: It is thickening of inferior rectus with thickening of inferior oblique with the medial and lateral check ligaments. They act as a hammock like support to the eyeball.
4. Applied anatomy
- In case of the fracture of the orbit, the eyeball does not sag, if the suspensory ligament is intact.
- The fracture of the orbit associated with paralysis of inferior rectus manifests as double vision.
Question 11: What is the reason of papilloedema in raised intracranial tension?
Answer: 1. Increased intracranial tension, papilloedema or choked disc is due to acutely obstructed venous return. The causes are the
- Venous engorgement
- Retinal haemorrhages
- 2. Increased intracranial pressure is transmitted to the subarachnoid space around the optic nerve.There is excess of fluid in the subarachnoid space which extends as far as the lamina cribrosa sclerae.
- Venous return is through the central vein of the retina. It is blocked.
- There is leakage of fluid around the
Optic disc, and
Retina. - Ophthalmoscopy examination shows
- Engorged veins,
- Swelling of the disc, and
- Obliteration of th physiological cup.
This is known as papilloedema.
Cornea Of Eye
Question 12: What is the applied importance of cornea?
Answer: Applied importance of cornea
1. Indications of corneal transplant
- Defective cornea interferes with the normal vision.
- Healthy cornea from a dead person (through eye donation).
2. The corneas are most common and successful organ transplants because of following reasons
- Cornea is avascular.
- There is no immunological reaction after corneal transplantation.
3. Protection of cornea by ferritin: Melanin pigment is absent in cornea. Melanin protects from ultraviolet light rays. Since eye is continuously exposed to UV light, it is likely to damage the DNA of nuclei.
4. Ferritin, an iron storage protein, is present in the eye. It prevents the damage of DNA present in nuclei. Therefore, the carcinoma of corneal epithelium is very rare.
Cornea Of Eye
1. It forms anterior l/6th of the outer coat of eyeball. Cornea is transparent because of following reasons:
- Regular arrangement of fibres.
- Refractive index of ground substance and fibres is same.
- Thickness of each fibril is less than wavelength of light.
- Critical level of water is maintained by active absorption of water by endothlium.
- No blood vessels.
2. Peculiarities: Cornea has
- No blood vessels,
- No lymphatics, and
- Rich nerve supply. Nerves are non-myelinated.
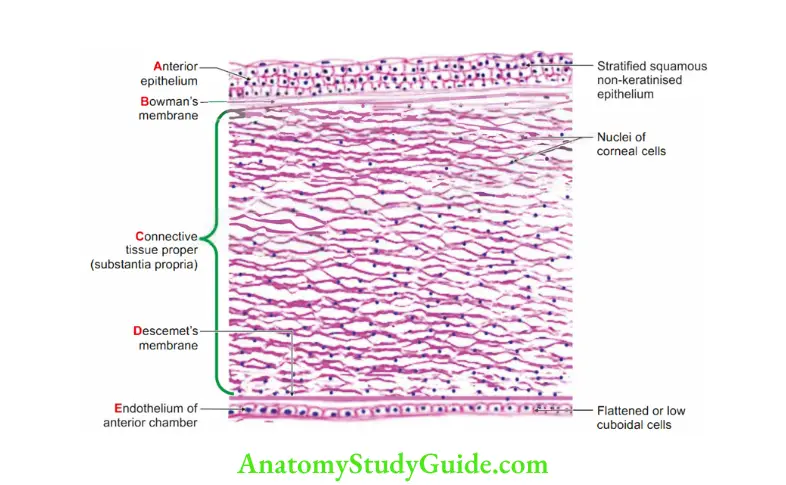
3. Layers: There are 6 layers of the cornea
1. Anterior epithelium (external epithelial layer):
- Stratified, squamous non-keratinised epithelium.
- Superficial cells are squamous and have flat nuclei.
- Deeper cells are columnar and have rod-shaped nuclei
- Cells rest on linear basement membrane.
- Cells never keratinise.
- Contain numerousfre nerve endings; hence, this layer is extremely sensitive.
2. Bowman’s membrane (anterior limiting membrane)
- Epithelium rests on this layer.
- Structure less, transparent and homogenous membrane.
- Contains collagen fibres which are produced by substantia propria.
3. Connective tissue proper (substantia propria)
- Main substance of cornea.
- Present deep to Bowman’s membrane.
- Modified, transparent, flattened connective tissue.
- The connctive tissue contains dens collagen fibres containing corneal spaces.
- It contains 200-250 lamellae and about 2000 fibres. It is embedded in ground substance containing sulphated glycosaminoglycans.
- The collagen fibres are of Type II (diameters 20 nm.)
Arrangement of fibres is very regular. - Fibres within lamellae are parallel to one another and are at obtuse angle to those of fibres adjacent to lamellae.
- Contains fibroblast which is stellate or flat. They are also called keratocytes or corneal corpuscles or corneocytes.
Cornea Of Eye
4. Dua’s layer (Dr Harminder Dua): It is strongest layer measuring 7 to 14 micron.It creates strongest barrier.
5. Descemet’s membrane
- Formed by homogeneous material.
- Membrane breaks at the margin of the cornea into fibres which form inner wall of sinus venous sclera.
- Spaces between these trabeculae are called the spaces ofiridocorneal angle.
6. Edothelium of anterior chamber
- Bathed by aqueous humour. Hence, it is not a true endothelium.
- It is single layer.
- It is metabolically most active.
- Lined by low cuboidal epithelium.
- Adapted for transport of ions.
Question 13: Layer of rods and cones consists of what? cuboidal cells
These are the photoreceptors; they pass through the external limiting membrane. Rods and cones are light receptors of the eye.
1. The cones respond to
- Acuity of vision
- Brightness of vision
- Colour vision.
2. Rods respond to Dim light.
Question 14: Draw pictures of rods and cones
Answer:
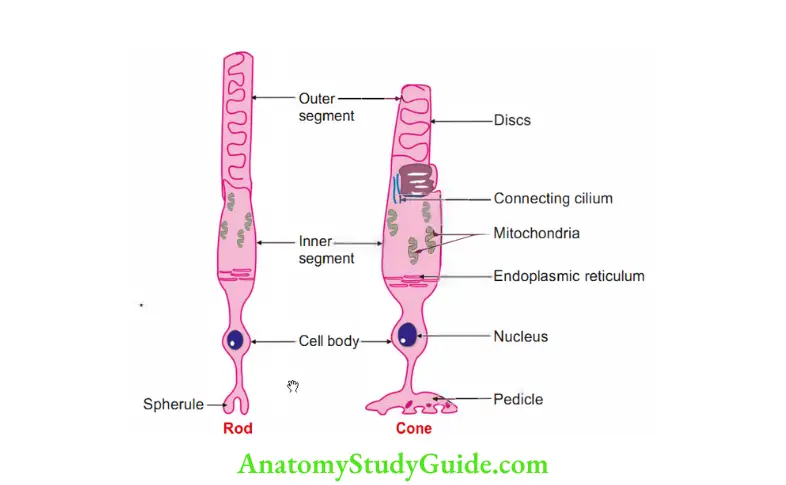
Question 14: What are the functions of Pigment Epithelium of Retina?
Answer: 1. It absorbs excessive light.
2. It prevents reflection of light.
3. It may play a role in regular spacing of rods and cones.
4. It provides mechanical support to rods and cones.
5. It has a phagocytic role. It “eats up” the ends of rods and cones.
6. It produces melanin.
Retinal Pigment Epithelium Detachment
Question 15: Enumerate the neurons seen in retina.
Answer: 1. Rods and cones
2. Bipolar neurons
3. Ganglion
4. Optic nerve
Question 13: What are the cells in outer nuclear layer, inner nuclear layer and ganglion-cell layer?
Answer: 1. Outer nuclear layer: This layer consists of nuclei of photoreceptors.
2. Inner nuclear layer: It contains nuclei of
- Bipolar cells,
- Muller cells,
- Horizontal cells: They establish contact betwen different photoreceptors in the outer plexiform layer.
- Amacrine cells (A-neg. + Gr. makros-long). Having no long processes. They connct ganglion cells and bipolar neurons to each other in the
3. Ganglionic cell plexiform layer: This layers layer consists of large cell bodies of ganglion cells.
Question 14: Plexuses between processes of which cells are formed in outer and innr plexiform layer?
Answer: 1. Outer plexiform layer: The processes of adjoining gliocytes meet to form a thin external limiting membrane.
2. Inner plexiform layer: It is formed by synapse of axons of bipolar cells with the dendrites of ganglion cells.
Question 15: Layer of optic nerve fibres is formed by which processes of which cells?
Answer: Axons of the ganglion cells travel in this layer towards the optic disc.
Question 16: What are outer and inner limiting membranes?
Retinal Pigment Epithelium Detachment
Answer: 1. Outer limiting membrane is a sieve-like membrane.
- It is present between 2nd and 3rd layer of retina.
- It looks like a pink linear marking lamina.
- It is a thin external limiting membrane.
- It is formed by
- Glial cells known as Muller cells with the
- Cell bodies of photoreceptor cells.
2. Inner limiting membrane
- It consists of the processes of Muller cells.
- Internally, the gliocytes extend to the internal surface of the retina and form aninternal limiting membrane.
- This membrane separates the retina from the vitreous.
- The retinal gliocytes are neuroglial in nature.
- They support the neurons of the retina and may ensheath them.
- They probably have a nutritive function as well.
Retina
It has 10 layers.
1. Pigment cell layer: It is single layer of cuboidal cells. The cells have rounded nuclei and the apical cytoplasm contains melanin granules.
2. Layer of rods and cones
1. Rods and cones are light receptors of the eye.
2. The cones respond to.
- Acuity of vision.
- brightness of vision.
- Clour vision.
3. RoDs respond to dim light.
3. Outer limiting membrane: Contains lateral process of radial fibres of nuclear cells.
4. Outer nuclear layer: Contains cell bodies of rods and cones which contain photosensitive process of neurons.
5. Outer plexiform layer: Contains axonal process of rods and cones, dendrites of bipolar.
6. Inner nuclear layer: It contains
- Cell bodies and nuclei of bipolar neurons (2nd order neurons of visual pathway).
- Association neurons
Horizontal cells.
Amacrine cells. - Supporting cells (Muller’s cells)
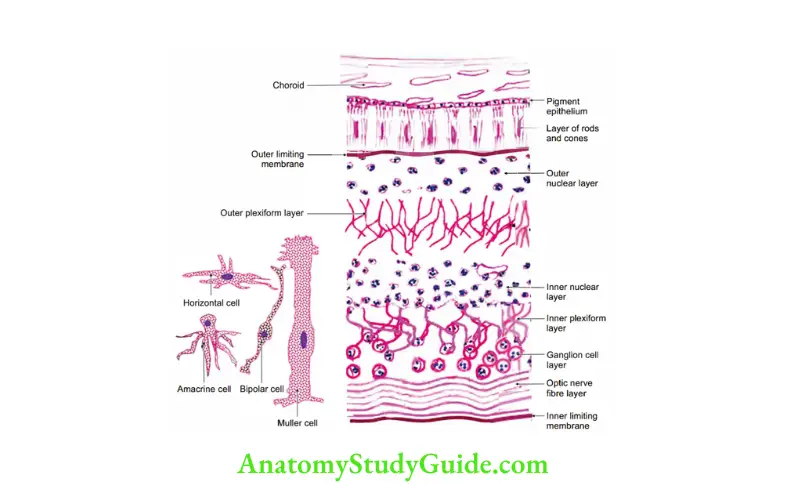
7. Inner plexiform layer: Contains synapse between axons of bipolar cells and also process of association cells or amacrine cells.
8. Ganglion cell layer: Contains cell bodies of ganglion cells. These are large multipolar cells with prominent Nissl’s granules. The axons of ganglion layer form the optic nerve.
9. Optic nerve layer: Contains optic nerve fibres and Muller’s fibres.
10. Inner limiting membrane: The surface facing next layer is thrown into processes which insinate between rods and cones. It prevents diffusion of light. It is innrmost layer of retina and represents a basal lamina formed by the expanded inner ends of Muller cells.
Retinal Pigment Epithelium Detachment
Question 17: Name the different layers of eyelid.
Answer: 1. Skin
- It forms the anterior surface.
- It is hairless except along margins of lid.
- Margins of lid have 3 to 4 rows of hair-eyelashes.
- It has modified sweat glands-the glands of Moll and sebaceous gland of Zeiss. I
2. Muscle layer
- Orbicularis oculi, and
- Levator palpebrae superioris.
3. Tarsal plate
- It is dense connctive tissue.
- It gives support to eyelids.
- It has sebaceous glands called tarsal glands or Meibomian glands.
The ducts of these glands open into free margin of eyelid.
The oily secretion forms a thin layer over tear and prevents evaporation of tears.
4. Conjunctiva
- It forms the posterior layer.
- It is lined by stratified columnar or cuboidal epithelium.
Question 18: What is the nerve supply of eyelid?
Answer: 1. The upper eyelid is supplied by the following nerves (from lateral to medial side).
- Lacrimal nerve, branch of ophthalmic division of trigeminal nerve.
- Supraorbital, branch of frontal nerve.
- Supratrochlear, branch of frontal nerve
- Infratrochlear nerves, smaller terminal branch of nasociliary nerve.
2. The lower eyelid is supplied by the
- Infraorbital nerve: It is the continuation of maxillary nerve, and
- Infratrochlear nerves: These are smaller terminal branches of nasociliary nerve.
Question 19: Why the oedema in nephrotic syndrome appears first on face and eyelids?
Answer: 1. Laxity of the greater part of skin of eyelid and face facilitates spread of oedema. Hence, oedema in nephrotic syndrome appears first in the face.
2. Superficial fascia of the eyelid is devoid of fat and composed of loose tissue. Hence, oedema of the eyelid is very common.
Question 20: What is the advantage of blinking of eyelids?
Answer: Blinking of eyelids helps in uniform spread of tears over the eyeball and keeps the eyeball moist.
Eyelid
Features
1. Both the surfaces of the eyelid are covered by epithelium.
- Skin of the eyelid is covered by stratified squamous keratinised epithelium.
- Mucous membrane of the eyelid is lined by stratified columnar epithelium.
2. Skeleton is formed by a mass of fibrous tissue called tarsus or tarsal plate.
3. Fat cells are absent in the subepithelial connective tissue.
4. Arrector pilorum muscle is absent in the hair follicle.
5. Glands: A To Z
- Accessory lacrimal glands are present. They are also called glands of Wolfring or Krause’s gland. They are serous in nature.
- Tarsal glands (Meibomian gland): It is a modified sebaceous gland.
- Glands of Zeiss: These are sebaceous glands present along the eyelashes.
- Moll’s gland: These are modified sweat glands.
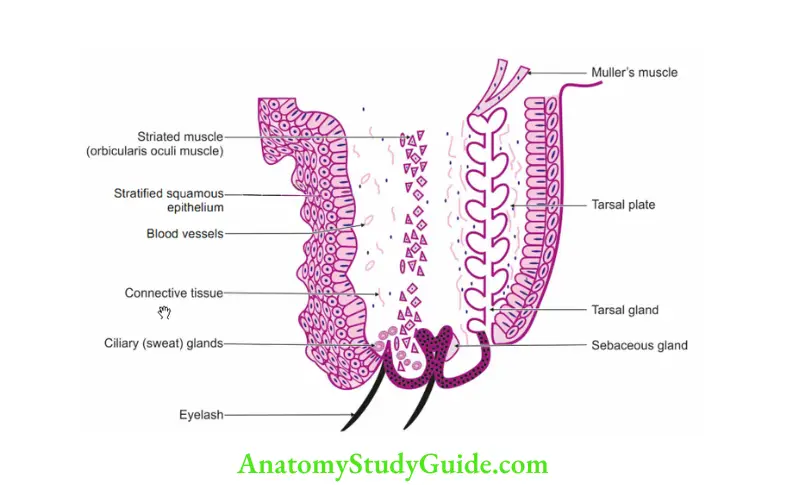
Question 21: What is the significance of colour of conjunctiva?
Answer: 1. The conjunctiva is a moist, transparent membrane.
- The part lining the lids is called palpebral conjunctiva.
The part lining the sclera is called the ocular or bulbar conjunctiva.
2. Significance of conjunctiva
1. The conjunctiva is colourless, except when its vessels are dilated 349
- Eyes inflamed or tinged with blood is called “bloodshot eyes”. It is congested conjunctiva.
- Hyperaemia of the conjunctiva is due to local irritation (e.g. from dust, chlorine, u(or smoke).
- Conjunctivitis (“pink eye”) is contagious infection of the eye.
2. Bulbar conjnctiva
- It is vascular.
- Inflammation of the conjnctiva leads to conjunctivitis.
- It is used to assess the depth of jaundice.
3. Palpebral conjunctiva
- It is normally red and vascular.
The look of palpebral conjunctiva is used to judge haemoglobin level.
It is commonly examined in cases of suspected anaemia, a blood condition commonly manifested by pallor (paleness) of the mucous membranes.
Sclerocorneal junction
1. It is junction of transparent cornea and opaque sclera .
2. At the junction
1. There is change of epithelium to that of conjunctiva.
1. The epithelium of the palpebral conjunctiva is typically two layered
- Superficial columnar cells, and
- Deep flattened cells.
2. The epithelium of the sclera and fomix is three layered
- Superficial columnar,
- Middle polygonal, and
- Deep flattened cells.
3. At sclerocorneal junction: Stratified squamous epithelium.
4. At cornea
- Anterior epithelium is stratified squamous non-keratinised.
- Posterior epithelium-cuboidal.
2. Bowman’s membrane changes into subepithelial layer of connective tissue.
3. Collagenous bundles of the sclera continue as collagenous bundles of cornea.
They become parallel with each other and appear homogenous and transparent.
4. Posterior lip forms a projecting ridge in which the ciliary body is fastened..
5. Descemet’s membrane terminates into trabecular meshwork. It encloses small spaces known as spaces of Fontana.
- They are lined by attenuated epithelium.
- They communicate with the anterior chamber of eye.
- There are several small cavities.
They are lined by epithelium.
They are anterior and lateral to trabecular meshwork.
These cavities are the cross-sections of a circular canal.
The canal is called canal of Schlemm.
They are parallel to the cornea.
The canal communicates with the venous spaces and is usually filled with clear aqueous humour.
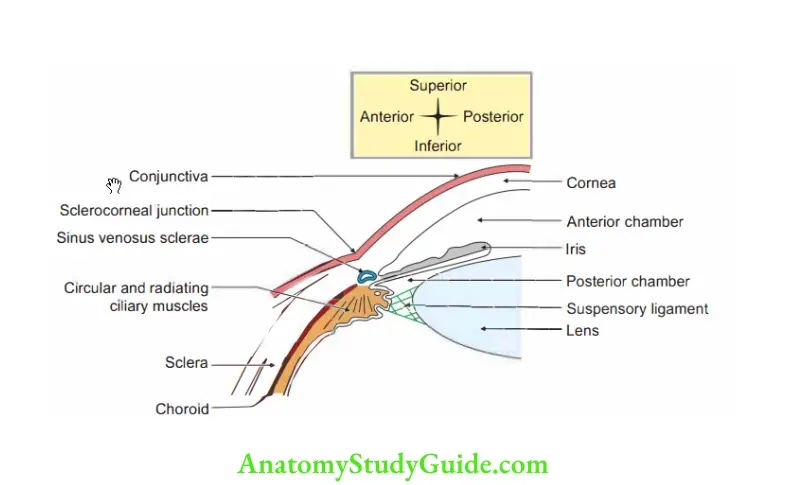
Give the nerve supply of iris
1. Nerv supply of iris
- The long ciliary nerves convey the sensory fibres.
- Motor fibres to
- Dilator pupillae are derived from sympathetic nerves.
- Sphincter pupillae are derived from parasympathetic nerve.
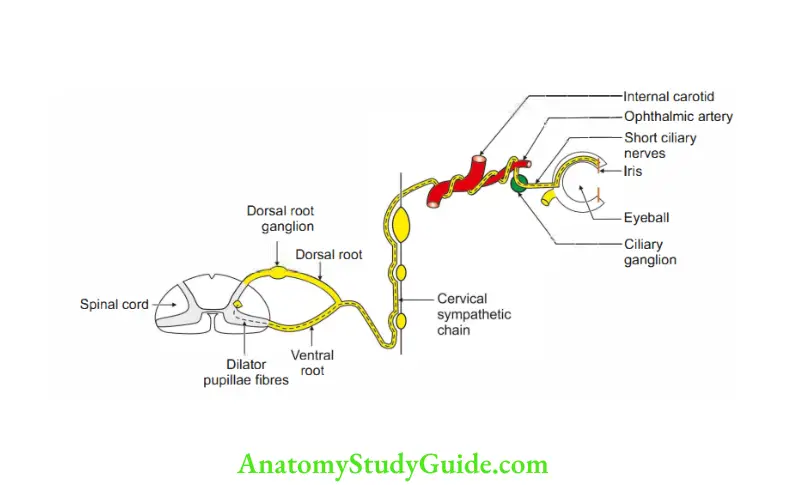
2. Applied anatomy
- The injury to the cervical cord produces pupillary changes.
- Injury distal to the lowest trunk of brachial plexus does not produce pupillary changes.
- Constriction of pupil is one of the manifestations of Homer’s syndrome. It results from paralysis of cervical sympathetic nerves (Tl fibres).
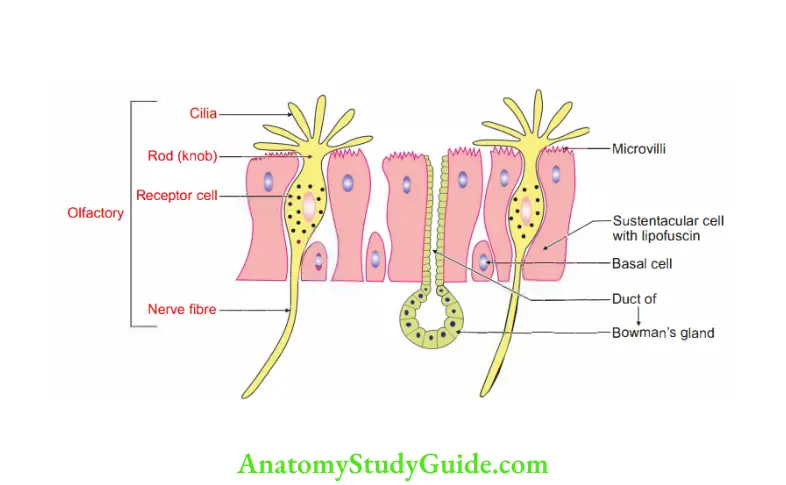
Give the histology feature of olfactory epithelium.
1. The olfactory epithelium is pseudostratified. It is much thicker than the epithelium lining the respiratory system. There are three types of cells.
1. Olfactory cells: These are modified neurons. It has
- Central part containing a rounded nucleus. The nuclei lie at various levels inmbasal two-thirds of the epithelium.
- Two processes
- Proximal process represents the axon.
Distal process ends in a thickening called the rod or knob. Rods give rise to cilia. - Olfactory cells have short life. They are replaced by new cells produced by division of basal cells. This is the only example of regeneration of neuronsin mammals.
2. Sustentacular cells: They support olfactory cells.
- The nuclei are oval and lie on the free surface of the epithelium.
- The cytoplasm contains yellow pigment. It gives yellow colour to olfactory mucosa.
- Basal cells: They are placed deep. They do not reach the luminal surface. They
divide to form new olfactory cells to replace dead.
Development of eye
1. Chronological age: Fourth week of intrauterine life.
2. Germ layers
1. Surface ectoderm gives rise to
1. Lens
2. Lacrimal apparatus
- Lacrimal gland
- Lacrimal sac
- Lacrimal duct
3. Lid and its gland
4. Epithelium of the
- Conjunctiva! sac
- Cornea.
2. Mesoderm
1. Choroid
2. Hyaloid artery. It regresses it before birth. Remnant or hyaloid artery
- Muscae volitantes: Incomplete regression
- Mittendorf’s dot: Posterior pole at end.
- Bergemeister’s papilla: Attachments at optic disc
- Persistent hyaline artery
- Tunica vasculosa lentis
- Persistent pupillary membrane: Remnant of mesoderm.
- Persistent hyprplastic primary vitreous
3. Temporal part of sclera
4. Fleshy belly of extraocular muscles.
3. Neuroectoderm gives rise to
- RPE: Retinal pigment epithelium develops from outer lip of optic cup
- Inner lip of optic cup: Neurosensory retina-all layers of retina
- Ciliary epithelium
- Iris epithelium
- Sphincter pupillae
- Dilator pupillae
- Zonule: Tertiary vitreous
- Vitreous gel: Secondary vitreous
- Subretinal space
- Optic stalk gives optic nerve.
4. Neural crest cells. They migrate to final destination.
- Corneal endothelium
- Trabecular meshwork
- Descemet’s membrane
- Corneal stroma
- Bowman’s membrane
- Iris stroma
- Ciliary muscle
- Ciliary storma
- Sclera
- Tendon of the extraocular muscle
- Tenon’s capsule
- Oligodendrocytes
- Meninges of optic nerve
- Ciliary ganglion
- Orbital bones
- Melanocytes of iris.
5. Arrest or failure of neural cell migration
- Congenital Homer’s syndrome.
- Neurocristopathy:
- Congenital aniridia
- Axenfeld-Rieger syndrome
3. Source
1. Forebrain vesicle gives rise to
- Retina, and
- Optic nerve,
4. Anomalies
1. Coloboma (mutilation, defect): Defective closure of optic fissure, siteventromedial segment.
- Coloboma of optic disc: It is congenital. Morning glory flower: Vessels come straight.
- Chorioretinal coloboma: It favours retinal detachment.
- Iris coloboma: Most commonly located.
- It is incomplete coloboma.
- Pear or tear shaped
- It is associated with lens coloboma.
2. The causes of congenital cataract may be
- Hereditary
- Infection by rubella virus.
3. Astigmatism: Faulty curvature of cornea or lens produces astigmatism.
4. Rare anomalies are
- Anophthalmos: Absence of eye.
- Aphakia: Absence of lens.
- Aniridia: Absence of iris.
- Synophthalmia: Fusion of eyes.
- Cydopia: Median eye.
- Microphthalmia: Too small eye.
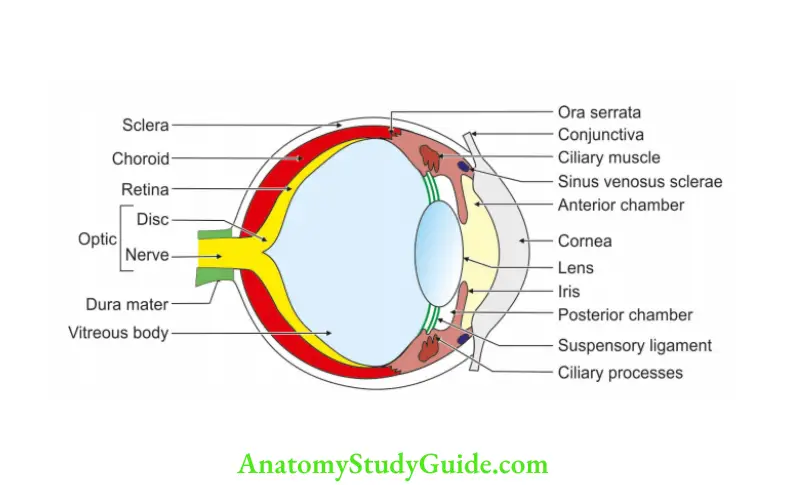
Question 22: Describe eyeball under the following heads:
Answer: 1. Outer coat,
2. Middle coat, and
3. Inner coat Coats: Eyeball has three coats
1. Outer coat
- Sciera
- Cornea
2. Middle coat
- Choroid
- Ciliary body
- Iris
3. Inner coat:
- Retina
- Lens
- Aqueous humour.
1. Outer coat
1. Sciera (hard)
1. External features
- It is smooth and white in colour. It forms 5/6th of the fibrous layer.
- It receives insertion of
- Four recti muscles in front of the equator, and
- Two obliques-behind the equator.
2. Ends
- Anterior end continues with cornea at the sclerocorneal junction.
- Posterior end continues with dura mater of the optic nerve.
3. Surfaces
- Outer surfa is covered by a Tenon’s fascia. The space between Tenon’s fascia and sclera is called episcleral space or sub-Tenon’s space. It is _ traversed by fibrous strands.
- Inner surface is covered by perichoroidal space.It is traversed by connctive Z tissue that contains pigment cells. It is brown and has grooves for ciliary -o vessels and nerves.
4. Perforating structures
- Optic nerve-3 mm medial to centre of the posterior aspect of sclera.
- Ciliary vessels and nerves-around the exit of the optic nerve.
- 2 or 5 venae vorticosae.
5. Lamina cribrosa (cribrum-L. sieve): Posterior part of the sclera is perforated by structures. It gives the appearance of a sieve. The structures piercing are
- Optic nerve
Central artery, and
Vein of the retina. - Applied anatomy: The lamina cribrosa is weak. In glaucoma, there is increased intraocular pressure. This results in bulging of the lamina
outwards.
6. Sinus venosus sclerae:
- There is an important venous structure at the sclerocorneal junction called sinus venosus sclerae (canal of Schlemm).
- It is lined by endothelium.
- Between canal of Schlemm and the anterior chamber, there is only a meshwork. It is formed by trabeculated (partitioned) tissue.
The aqueous humour (liquid) > anterior chamber> trabeculated tissue> venous system. - Applied anatomy: Any form of obstruction to this drainage may lead to rise in intraocular pressure (glaucoma).
2. Cornea
1. Features
1. It forms anterior 1 /6th of the outer coat of eyeball. It is transparent because of the following reasons. Cornea ART
- Critical level of water is maintained. It is done by active absorption of water by endothelium.
- Arrangement of fibres is regular.
- Refractive index of ground substance and fibres is same.
- Thickness of each fibril is less than wavelength of light.
2. Peculiarities: It has
- No blood vessels. Nutrition is by aqueous humour.
- No lymphatics
- Therefore, cornea can be easily transplanted.
- Rich nerve supply. Nerves are non-myelinated.
3. Layers: There are 6 layers of the cornea.I –
- Anterior epithelium, Bowman’s membrane (anterior limiting membrane),
- Connective tissue proper (substantia propria),
- Descemet’s membrane (true basement membrane)
- Dua’s layer
- Endothelium of anterior chamber
2. Middle coat: It is also called uveal tract (uvea-grape) or pigmented layer of eye. It consists of
1. Choroid (pigmented vascular layer of eyeball) Fig. 19.11)
1. Features
- It is present in the posterior 5 /6th of the eyeball.
- It is thin pigmented layer that lines the posterior part of sclera.
- It is a vascular membrane of dark brown colour.
- It lines the inner surface of the sclera.
- It can be readily stripped up.
- It is brown in man and black in many animals.
2. Surfaces: It has two surfaces-outer and innr. u..
- The outer surface is loosely conncted with the sclera by suprachoroid membrane. It is also called lamina fusca of the sclera. C
- The inner surface is attached to the pigment layer of the retina.
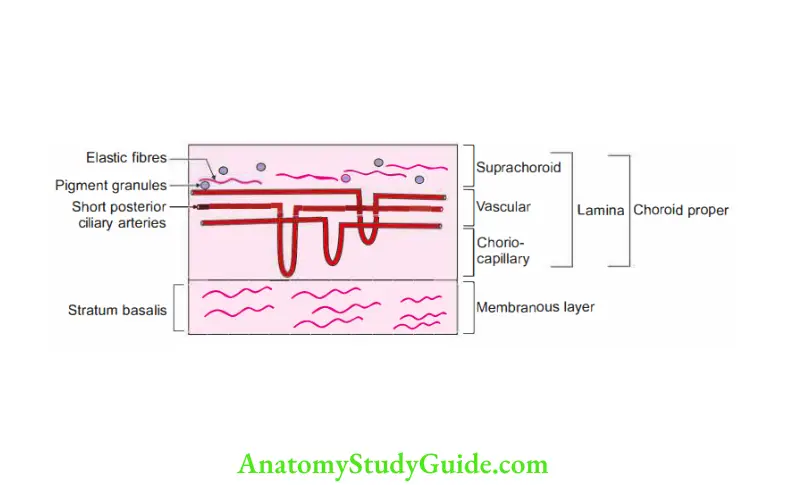
3. Histology of choroid: It consists of masses of blood vessels sandwiched between two avascular membranes. From external to internal, they are:
1. Suprachoroid lamina
- It is a non-vascular lamina of vascular coat.
- It consists of elastic fibres having pigment granules.
- Between the suprachoroid lamina and choroid proper, there is a thinlayer of connctive tissue called the stratum intermedium.
2. Choroid proper: It consists of two layers
1. The outer layer is called the vascular lamina or stratum vasculosum. It consists of larger arteries and veins, namely
- Branches of short posterior ciliary arteries and
- Veins which unite to form 4 to 5 large veins called venae vorticosae, and
- Pigment cells.
2. The inner layer is called the choriocapillary lamina.
- It is formed by capillary plexuses derived from branches of short posterior ciliary arteries.
3. Stratum basalis
- It is a membranous layer of elastic fibres.
- It lies on the outer surface of the pigmented layer of the retina.
- It consists of cells or fibres deep to the choriocapillary lamina.
4. Tapetum
- In many animals, e.g. in bullock’s eye, the back part of the choroid presents tapetum.
It reflects light and gives it a greenish appearance. - Uveitis: It is inflammation of vascular layer of the eyeball. It may progress to severe visual impairment and blindness.
2. Ciliary body: The anterior end of the middle vascular coat is dilated and called ciliary body. It consists of the following structures.
- Ciliary ring
- It is a circular ring of 4 mm breadth.
It is marked with ridges.
Posteriorly, it is continuous with the choroid. - Ciliary processes
- These are formed by infoldings of the layers of the choroid.
- They are 60 to 80 in number.
- Types of fibre: Short and long.
- Ends
Peripheral end of the process is attached to the ciliary ring.
Central ends of the processes are free. They are directed towards the posterior chamber of the eyeball and circumference of the lens. - Surfaces
Its anterior surface is continuous with the iris at its periphery.
Its posterior surface is connected with the suspensory ligament of the lens. - Function: The ciliary processes secrete the aqueous humour,
3. Ciliary muscles
- Types of muscle. It consists of two sets:
- Radiating, and Circular.
- Radiating fibres:
- They lie outside. They are attached Anteriorly to scleral spur.Posteriorly to ciliary ring and ciliary processes.
1. Circular fibres
- These lie on the inner side of the radiating fibres.
They are arranged as a circular ring behind the iridocorneal angle.
It is close to the circumference of the iris. - Circular fibres are well-developed in the hypermetropic and more or less absent in the myopic.
- Action of ciliary muscles: Accommodation of eye for near objects.
This is done by changing the curvature of the lens.
As the ciliary muscles contract, they draw the ciliary processes forwards.
This causes the relaxation of the suspensory ligament of the lens.
So, the anterior aspect of the lens will be more convex.
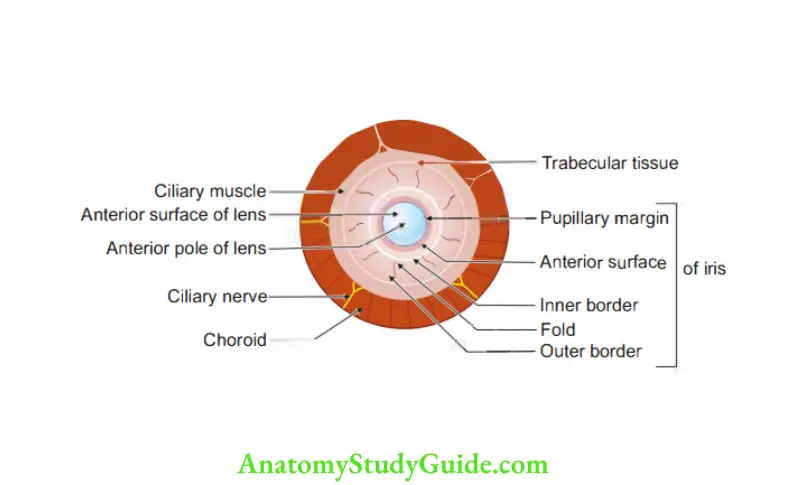
3. Iris (diaphragm)
- Definition: It is a musculovascular contractile diaphragm between the cornea and the lens.
- Shape and situation: It is a thn circular disc suspended in the aqueous humour between the cornea and lens.
- Pupil: It is a circular aperture in the iris.
1. Surfaces
- Anterior surface: It is convex and forms the posterior boundary of the anterior chamber of the eyeball.
- Posterior surface: It is concave and forms the anterior boundary of the posterior chamber of the eyeball.
2. Colour: It is produced by the reflection of light from the pigment cells and varies from individual to individual.
- White eyes: It is due to absence of pigments.
- black : Pigments lie in the stroma of the iris.
- blue eyes: Pigments lying on the posterior surface of the iris.
3. Muscles of iris: They are involuntary and consist of circular and radiating fibres.
1. Circular fibres (sphincter pupillae)
- They form a circular band about 1 mm wide.
- It is around the margin of the pupil towards the posterior surface of the iris.
- Nerve supply: Parasympathetic via the oculomotor nerve.
- Action: Constriction of the pupil.
2. Radiating fibres (dilator pupillae): These lie close to the posterior surface of the iris. These converge from the circumference to the margin of the iris.
- Nerve supply: Sympathetic via the superior cervical sympathetic ganglion.
- Action: Dilation of the pupil.
4. Development of the muscles of iris
- Germ layer: Ectoderm
- Source: Outer cells of the optic cup.
- The lower division of oculomotor nerve supplies sphincter papillae.
It may get compressed in the cavernous sinus. The 1stsign is ipsilateral slowness of the pupillary””esponse to light.
3. Inner coat
1. Retina
1. Definition:
It is the nervous coat, lying deep to the choroid. It is meant for the reception of the light stimuli.
2. Fate
- Anteriorly: It ends in a free serrated margin just behind the ciliary body.
- Posteriorly: It is continuous with the optic nerve.
3. Parts of retina:
- Optic part: It is the part from the optic disc up to the ora serrata. This part consists of all the functioning layers, i.e. nervous and pigmented layers.
- Ciliary part of the retina.
- Iridial part of the retin called pars iridica retinae. The last two layers are the prolongations of the pigmented layer. They are present only on the posterior surface of the ciliary processes and iris, respectively.
4. Surfaces
- Outer surface: It is in contact with the choroid.
- Inner surface: The following features are found:
1. Macula (spot) lutea (yellow): It is an oval yellowish area near the centre of the posterior part of the retina. Here, the visual sense is most perfe.
A depression at its centre is called fovea centralis where the retina is very thin.
2. Optic disc It is the area which is pierced by the optic nerve.
- The diameter is about 1-5 mm.
- It is situated 3 mm medial to the macula lutea.
- The central part of the disc is perforated by the central artery and vein of the retina.
- This optic disc is insensitive to light and is called the blind spot.
3. On ophthalmoscopic examination,
- Normally optic disc looks pink due to presence of th capillary vessels.
- In optic atrophy, the disc looks white as the capillary vessels disappear.
- In hyprtension or thrombosis of central retinal veins, there is oedema of optic disc called papilloedema (chocked disc or oedema of disc).
4. Arterial supply of retina
1. Up to the outer nuclear layer from outside,
- The retina has no direct arterial supply.
- It gets its nutrition by diffsion from the choriocapillary layer of the choroid.
- The remaining layers:
- By central artery of the retina, a branch of the ophthalmic artery.
It is a classic example of an end artery. - Rupture of central artery of retina results in blindness of an individual.
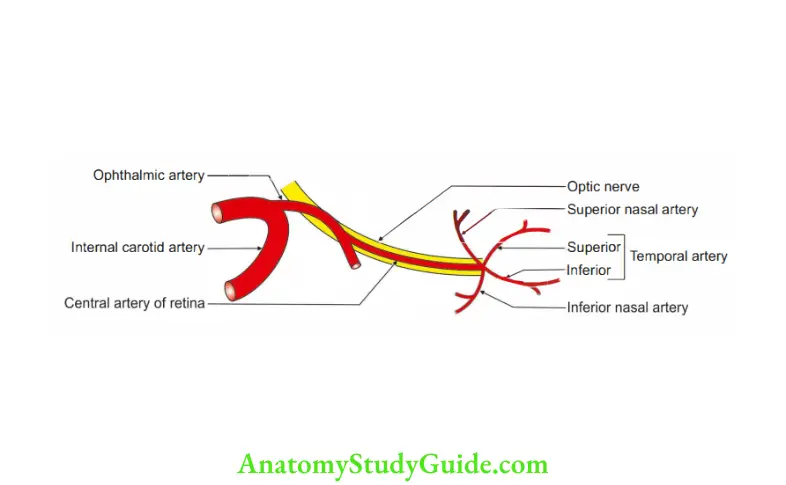
5. Venous drainage of retina
- The retinal veins end in the central vein of the retina.
- The central vein ends in the cavernous sinus or superior ophthalmic -o
vein.
Contents of eyeball
1. Aqueous humour
2. Lens
3. Vitreous body.
1. Aqueous humour
1. Formation: It is secreted from the capillaries of the ciliary processes into the posterior chamber of the eyeball.
2. Circulation: From the posterior chamber pupil- anterior chamber-
3. It drains into space of the iridocomeal angle. (Here it is filtered by the lining membrane of the endothelial cells covering those spaces)- sinus venosus sclerae (canal of Schlemm) anterior ciliary veins- ophthalmic vein.
- Accessory route: A portion of th aqueous humour may be absorbed as follows:
- Via the blood vessels of the iris.
Via the lymph spaces of the iris. - Fluid from the posterior chamber- zonular space- hyaloid fossa
- Hyaloid canal- optic disc- perineural spaces around the nerve filaments of the optic nerve.
4. Intraocular tension: Normal is 15-20 mm Hg.
If there is interference in the absorption of the aqueous humour into the sinus venosus sclerae; there will be an increase in the tension which results in the formation of glaucoma.
2. The lens
- Definition: The lens is a transparent biconvex body, situated behind the iris and in front of the vitreous body .
- Capsule: Lens is enclosed in a capsule which is a transparent elastic membrane.
3. Features
1. The anterior surface is less convex than the posterior surface.
- Its central part is in contact with the pupillary membrane till it disappears.
- After that, it forms the posterior boundary of the anterior chamber of the eyeball.
- Its periphery is separated from the iris by the aqueous humour of the posterior chamber.
- Its curvature is regulated by the ciliary muscles for focusing the near or distant objects.
- These muscles are called muscles of accommodation.
2. Posterior surface: It is more convex and occupies the hyaloid fossa on the anterior aspect of the vitreous body.
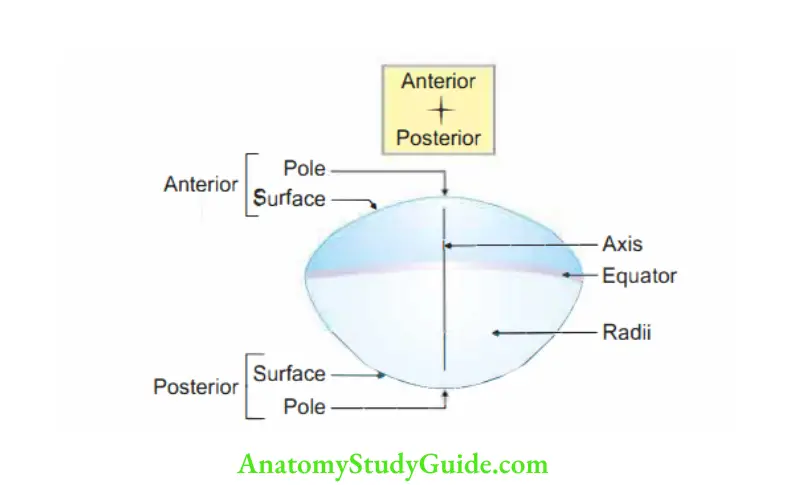
3. Poles: The central points of the surfaces are called anterior and posterior poles.
4. Axis: It is the line joining the two poles.
5. Equator: The peripheral circumference of the lens is the equator.
6. Dimensions:
- Axis: 4 mm.
- Transverse diameter: 9 to 10 mm.
- Refractile index: 1.43.
- Power of lens: 20 to 300
7. Nutrition:
It is avascular. In foetal life, the posterior part of the lens capsule is supplied by hyaloid artery. It is a branch of the central artery of the retina.
8. Structure
- Capsule: The lens is composed of a series of more or less concentrically arranged fibres around a firm central part called the lens nucleus. So, the periphery is soft and the centre is hard.
- Deep to the anterior part of the capsule, the lens is lined by epithelium.
- It isformed by transparent, nucleated columnar cells.
- These cells grow and fill the cavity of the lens vesicle.
- These elongated cells are called lensfires.
- These fibres run from periphery to the centre but never from pole to pole.
2. 1Applied:
- In foetus, lens is soft but in old age, it becomes harder and flattened, thereby reducing the focusing power. This condition is called presbyopia.
- In old age and also sometimes in early life, lens becomes opaque; this condition is called cataract.
3. The vitreous body
- Definition: It is a colourless, transparent jelly-like substance, situated behind the lens and on the innr surface of the retina.
It occupies the posterior 4/Sth of the eyeball.
2. Composition: It consists of
- 90% water,
- Salts,
- Mucoprotein, and
- Hyaluronic acid.
3. Hyaloid canal: It is traversed by a canal called hyaloid canal. In foetal life, it contains the hyaloid artery.
4. Hyaloid fossa: It is a fossa on the anterior surface of which lies the posterior surface of the lens.
5. Hyaloid membrane: Vitreous body is surrounded by its membrane. It is adherent to the retina in two places:
- At optic disc: Immediately in front of the ora serrata, it is thickened by radial fibres called ciliary zonulae.
- Ciliary processes.
6. Nutrition: No blood vessels pierce it. Nutrition is carried by vessels of the retina and ciliary processes.
7. Suspensory ligament of the lens: The ciliary zonule splits into two layers enclosing the lens:
- One layer is thin; it lines the hyaloid fossa.
- The other layer is thick and it is called the suspensory ligament.
- Its periphery is attached to the ciliary process and ora serrata.
- Centrally, it is attached to the lens slightly in front of its margin.
8. Function: In rest position, it keeps the anterior surface of the lens flattened under tension.
When the ciliary muscles contract, this ligament is relaxed and causes the anterior surface to become convex thereby accommodating to focus near objects.
Applied anatomy :
- The zonular fibres constituting the suspensory ligament of lens are very tough structures.
- Hence, cataract extraction in immature state is not usually done because of the tough zonule. In immatue state, it is removed by zonulysis.
Compartments of eyeball
1. Chambers of the eyeball: The eyeball is divided into two compartments by the lens and suspensory ligament
- Anterior compartment
- Posterior compartment
1. Anterior compartment: It is further divided by the iris into
- Anterior chamber
- Posterior chamber
1. Anterior chamber: It is 3 mm deep centrally.
1. Boundary
- Anteriorly: Posterior surface of the cornea.
- Posteriorly: Anterior surface of the iris and central part of the lens opposite the pupil.
- At periphery: It is limited by the angle between the cornea and iris, called the iridocomeal angle.
This angle is traversed by fibres called pectinte ligament.
The spaces though this ligament drai ino canal of Schlemm. Obliteration of this angle prevents the absorption of the aqueous humour, thereby increasing the interocular tension, i.e. glaucoma.
2. Contents: Aqueous humour coming from posterior chamber though the pupil.
2. Posterior chambers
1. Boundary:
- Anteriorly: Posterior surface of the iris.
- Posteriorly: Anterior surface of the lens and suspensory ligament.
Triangular in cross-section, i.e. pupil and lens coming in contact form the apex, ciliary processes form the base.
2. Communication: With the anterior chamber through the pupil.
2. Posterior compartment: It contains the vitreous body.
1. Definition: It is a colourless, transparent jelly-like substance, situated behind the lens and on the inner surface of the retina.
It occupies the posterior 4/Sth of the eyeball.
2. Composition: It consists of
- 90% water,
- Salts,
- Mucoprotein, and
- Hyaluronic acid.
3. Hyaloid canal: It is traversed by a canal called hyaloid canal. In foetal life, it contains the hyaloid artery.
4. Hyaloid fossa: It is a fossa on the anterior surface of the vitreous body. The lens is logged in the fossa. It is also called lenticular fossa or patellar fossa.
5. Hyaloid membrane:
- Vitreous body is surrounded by its membrane. It is adherent to the retina in two places:
- At optic disc: Immediately in front of the ora serrata, it is thickened by radial fibres called ciliary zonulae, Ciliary processes.
7. Nutrition: No blood vessels pierce it. Nutrition is carried by vessels of the retina and ciliary processes.
8. Suspensory ligament of the lens: The ciliary zonule splits into two layers enclosing the lens:
- One layer is thin; it lines the hyaloid fossa.
- The other layer is thick, and it is called the suspensory ligament.
- Its periphery is attached to the ciliary process and ora serrata.
- Centrally, it is attached to the lens slightly in front of its margin.
9. Function:
- In resting position, it keeps the anterior surface of the lens flattened under tension.
- When the ciliary muscles contract, this ligament is relaxed and causes the anterior surface to become convex thereby accommodating to focus
Applied anatomy :
- The zonular fibres constituting the suspensory ligament of lens are very tough structures.
- Hence, cataract extraction in immature state is not usually done because of the tough zonule.
- In immature state, it is removed by zonulysis.
- Zonulysis causes melting of zonular fibres. The lens floats up and is removed.
Leave a Reply