Endodontic Microbiology Introduction
For many years, the interrelationship of microorganisms and root canal systems has been proven. Leeuwenhoek observed an infected root canal of a tooth and found “cavorting beasties.” After this, it took 200 years for WD Miller to make the correlation between microorganisms and pulpal or periradicular pathologies.
Table of Contents
Read And Learn More: Endodontics Notes
In 1965, Kakehashi et al. found that bacteria are the main etiological factors in the development of pulpal and periradicular diseases. Kakehashi et al. proved that without bacterial involvement, only minor inflammation occurred in the exposed pulp.
All the surfaces of the human body are colonized by microorganisms. Colonization is the establishment of bacteria in a living host. It occurs if biochemical and physical conditions are available for growth. Permanent colonization in a symbiotic relationship with host tissue results in the establishment of normal flora.
Microbiology In Endodontics
Infection results if microorganisms damage the host and produce clinical signs and symptoms. The degree of pathogenicity produced by microorganisms is called virulence.
History of microbiology in association to endodontics:
1. 17th century:
AV Leeuwenhoek first described oral microflora.
2. 1890:
WD Miller (Father of oral microbiology) authorized the book “Microorganisms of human mouth”.
3. 1904:
F Billings described the theory of focal infection as a circumscribed area of tissue with pathognomic microorganisms 1909: EC Rosenow described the theory of focal infection as localized or generalized infection caused by bacteria traveling via the bloodstream from a distant focus of infection.
4. 1939:
Fish observed four distinct zones of periapical reaction in response to infection.
5. 1965:
Kakehashi et al. proved that bacteria are responsible for the pulpal and periapical disease.
6. 1976:
Sundqvist used different culturing techniques for the identification of both aerobic and anaerobic organisms and concluded that root canal infections are multifactorial.
Microbiology In Endodontics
Portals Of Entry For Microorganisms
Microorganisms may gain entry into pulp through several routes.
Entry through Open Cavity:
This is the most common way of entry of microorganisms into the dental pulp. When protective layers of a tooth (enamel and dentin) get destroyed by caries, traumatic injuries, fractures, cracks, or restorative procedures, microorganisms can gain access to the pulp.
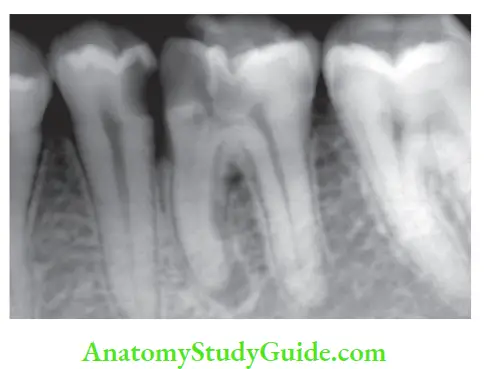
Through Open Dentinal Tubules:
Microorganisms can pass into the dentinal tubules and subsequently to the pulp. Bacteria are preceded in the course of tubules by their breakdown products which may act as pulp irritants.
Through the Periodontal Ligament or the Gingival Sulcus:
Periodontal pathology or treatment can remove cementum and exposes dentinal tubules to oral flares through which microorganisms gain entry into pulp via accessory and lateral canals.
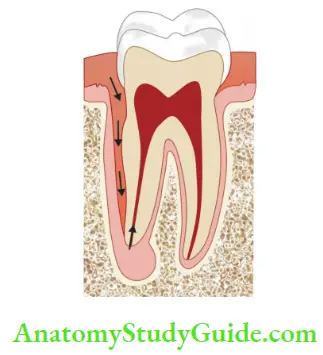
Anachoresis:
Anachoresis is a process by which microorganisms are transported in the blood to an area of inflammation where they establish an infection.
Microbiology In Endodontics
Through Faulty Restoration:
Faulty restoration with marginal leakage can result in contamination of the pulp space by bacteria.
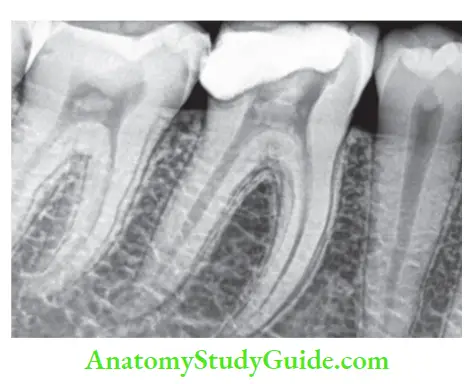
Classification Of Microorganisms
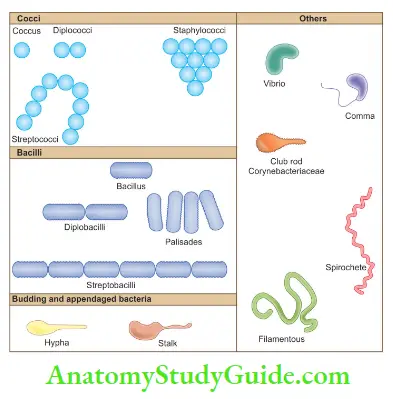
Microbial flora can be classified on the basis of Gram-positive organisms, for example, Streptococcus, Enterococcus, Treponema, Candida, Actinomyces, and Lactobacillus. Gram-negative organisms, for example, Fusobacterium, Campylobacter, Bacteroides, Veillonella, and Neisseria.
1. Obligate aerobes:
These organisms require oxygen for their growth because they can’t ferment or respire anaerobically, for example, tubercle bacilli.
2. Facultative anaerobes:
These organisms can grow in the presence or absence of oxygen, for example, Staphylococcus.
3. Microaerophilic:
These organisms grow in an oxygen environment but derive their energy only from fermentative pathways that occur in the absence of oxygen, for example, Streptococcus.
4. Obligate anaerobes:
These bacteria can grow only in the absence of oxygen, for example, Bacteroides, and Fusobacterium.
Microbiology In Endodontics
Microbial Virulence And Pathogenicity
- Pathogenicity is the ability of microorganisms to produce a disease.
- Virulence is the degree of pathogenicity of a microorganism.
In 1965, Hobson gave an equation showing the relation of the number of microorganisms, their virulence, the resistance of the host, and the severity of the disease.

Microbiology Of Endodontic Diseases
Virulent factors:
- Lipopolysaccharides (LPS)
- Extracellular vesicles
- Enzymes
- Fatty acids
- Polyamines
- Capsule
- Pilli
Lipopolysaccharides:
- LPS are present on the surface of Gram-negative bacteria.
- LPS have non-specific antigens which are not neutralized by antibodies.
- They exert numerous biologic functions when released from cells in the form of endotoxins. Endotoxins have the capability to diffuse into dentin.
Extracellular Vesicles.
- Extracellular vesicles are produced by Gram-negative bacteria in form of endotoxins, outer membrane fragments, or blebs. Vesicles contain enzymes and toxic products which are responsible for hemagglutination, hemolysis, and bacterial adhesion.
- They have trilaminar structure similar to the outer membrane of the parent bacteria. Since they have antigenic properties similar to the parent bacteria, they may protect bacteria by neutralizing specific antibodies.
Enzymes:
- Enzymes produced by bacteria can result in the spread of the infection, neutralization of immunoglobulin, and complement components.
- PMN (Polymorphonucleocytes) leukocytes release hydrolytic enzymes which degenerate and lyse to form purulent exudates and have adverse effects on the surrounding tissues.
Fatty Acids:
Various short-chain fatty acids like propionic acid, butyric acid, etc. are produced by anaerobic bacteria. These cause neutrophil chemotaxis, degranulation, and phagocytosis, and stimulate interleukin-1 production which further causes bone resorption and periradicular diseases
Microbiology Of Endodontic Diseases
Polyamines.
- These are biologically active chemicals found in the infected canals.
- Some of polyamines such as cadaverine, putrescine, and spermidine help in regulation of the cell growth, regeneration of tissues, and modulation of inflammation.
- Other virulent factors, like capsules present in Gram-negative black-pigmented bacteria, enable them to resist phagocytosis. Pilli may play an important role in the attachment of bacteria to surfaces and interaction with other bacteria.
Factors Influencing The Growth And Colonization Of Microorganisms
Influence of Oxygen:
- A factor highly selective for the microbial flora of root canals is the low availability of oxygen in infected root canals.
- In the initial stages, there is a predominance of facultative organisms, but later they are replaced by anaerobic bacteria.
Nutritional Factors:
Bacteria obtain their nutrition from tissue fluid and the breakdown products of the necrotic pulp tissue. Another source of nutrition for bacteria is inflammatory exudates containing serum and blood factors discharged from related inflammatory processes in the remaining pulp or the periapical tissues.
Bacteriocins:
Some bacteria produce bacteriocins, which are antibiotics-like proteins produced by one species of bacteria to inhibit another species of bacteria.
Coaggregation:
It is the existence of a “symbiotic relationship” between some bacteria which may result in an increase in virulence by the organisms in that ecosystem.
Bacterial Interrelationships:
Interrelationships between certain bacteria can be commensal or antagonistic which affects their survival.
Microbiology Of Endodontic Diseases
Microbial Ecosystem Of The Root Canal
- Microorganisms which can survive in an environment of low oxygen tension and can survive the rigors of limited pabulums are found in root canals.
- On average, 103–108 bacteria are found in endodontic infections accounting >700 species.
- The most commonly seen bacteria in root canals is streptococci (Gram-positive facultative anaerobic), especially in the coronal part of a root canal, others can be Staphylococcus, Gram-negative, and anaerobic bacteria.
- A new nomenclature is given to the species Bacteroides.
- In necrotic pulp, there is a lack of circulation with compromised host defense mechanisms; this makes pulp a reservoir for invading microbes.
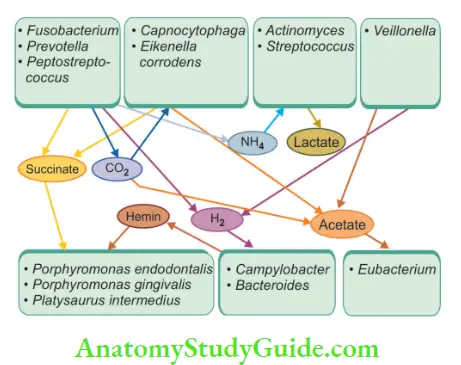
Here, tissue fluids and disintegrated cells from necrotic tissue, low oxygen tension, and bacterial interactions determine predominance of a particular type of bacteria. The growth of one bacterial species is dependent on other bacterial species which supply the essential nutrients.
In a similar way, antagonistic relationships may occur in bacteria, that is, by-products of some bacterial species may kill or retard the growth of other species.
New nomenclature of Bac teroides species:
1. Porphyromonas—Dark-pigmented (asaccharolytic Bacteroides species)
- Porphyromonas saccharolytic
- Porphyromonas gingivalis
- Porphyromonas endodontalis
2. Prevotella—Dark-pigmented (saccharolytic Bacteroides species)
- Prevotella melaninogenica
- Prevotella denticola
- Prevotella intermedia
- Prevotella nigrescens
- Prevotella corporis
- Prevotella tanneries
3. Prevotella—Nonpigmented (saccharolytic Bacteroides species)
- Prevotella buccae
- Prevotella bivia
- Prevotella oralis
Naidorf summarized the following generalizations in relation to organisms isolated from the root canals:
- Mixed infections are more common than single organism.
- Pulp contains flares almost similar to that of oral cavity.
- Approximately 25% of isolated organisms are anaerobes.
- Organisms isolated from fire-up as well as asymptomatic cases are almost similar.
- Various researchers have identified wide variety of microorganisms in the root canals which is partially related to personal interest and cultural techniques used by them.
Microbiology Of Endodontic Diseases
Types Of Endodontic Infections
According to the location of the infection in relation to a root canal, it can be classified as intraarticular or extraarticular.
Intraradicular Infections:
In intraarticular infections, microorganisms are present within the root canal system. These can be primary, secondary, and persistent infections according to the time of organisms’ entry into the canal.
Primary Intraradicular Infections (Virgin Infection):
- These are those microorganisms which initially invade the pulp tissue, resulting in inflammation and then necrosis.
- These are characterized by the presence of mixed habitats, mainly dominated by Gram-negative obligate anaerobes like Porphyromonas, Prevotella, Fusobacterium, Dialister, Campylobacter, and Treponema.
- Gram-positive anaerobes like Peptostreptococcus, Eubacterium, Actinomyces, and Streptococcus are also seen in primary intraarticular infections.
Secondary Intraradicular Infections:
- These infections are introduced during or after the treatment.
- In these infections, those organisms are present which were not prevalent during primary endodontic infections
1. Sources of microbes during treatment can be:
-
- Remnants of caries, plaque or calculus
- Leakage of rubber dam
- Contamination of instruments and irrigation solutions
2. Sources of microbes between the appointments
-
- Leakage of restorative materials
- The tooth opened for drainage
- Fracture of tooth/teeth
3. Sources of microbes after root canal treatment
-
- Leakage of restorative materials
- No use of rubber dam
- Fracture of teeth
- Secondary dental caries
4. Commonly found microorganisms in these infections can be Pseudomonas aeruginosa, Staphylococcus, Escherichia coli, Enterococcus faecalis, and Candida sp.
Persistent Intraradicular Infections:
- These are those microorganisms which survive in the root canal after intracanal antimicrobial procedures. Gram-positive are the most common persistent bacteria.
- In these infections, E. faecalis is the most commonly found organism.
- E. faecalis is considered to be most common reason for failed root canals and in canals with persistent infection.
- It is a Gram-positive cocci and is a facultative anaerobe.
- Because of the following features, E. faecalis can survive in root canals even in adverse conditions:
- It can persist in the poor nutrient environment of root canal-treated teeth.
- It can survive in the presence of medicaments like calcium hydroxide.
- It can stay alive in the presence of irritants like sodium hypochlorite.
- It can convert into a viable but nonculturable state (VBNC).
- It can form biofilm in medicated canals.
- It can penetrate and utilize fluid present in dentinal tubules.
- It can survive in prolonged periods of starvation and utilize tissue fluid that flows from the periodontal ligament.
- It can survive in low pH and high temperatures.
- It can acquire gene-encoding resistance combined with natural resistance to antibiotics.
- It can establish mono infections in medicated root canals.
- Its main virulent factors are hemolysin, gelatinase, aggregation substance, and extracellular superoxide.
Microbiology Of Endodontic Diseases
Extraradicular Infections:
- These are characterized by microbial invasion and proliferation in the inflamed periradicular tissues as a result of intraarticular infections, for example, acute alveolar abscess.
- Extraradicular infections can be caused by intraarticular bacteria or bacteria from the outer side.
- Commonly found microorganisms in extraarticular infections are Actinomyces sp., Treponema sp., P. gingivalis, Fusobacterium nucleatum, and P. endodontalis Other microorganisms found in endodontic infections are.
- Fungi
- HIV in the vital pulp of HIV/AIDS patient
- The virus can’t survive in necrotic pulp cases because they require living cells for their growth Available nutrients utilized by bacteria in root canal:
- Necrotic pulp tissue.
- Salivary components.
- Proteins and glycol proteins from tissue fluid.
- By-products of bacteria.
Microbiology of Endodontic Infections
The pathogenicity of Bacteroides is related to the presence of LPS and peptidoglycans. These:
- Induce cytokinins which play an important role in inflammation.
- Stimulate B-lymphocytes.
- Activate complement cascade.
- Release various enzymes like collagenase.
- Enhance the production of various pain mediators like bradykinin, histamine, and prostaglandins.
- LPS once released (as endotoxin) causes biological effects including inflammation and bone resorption.
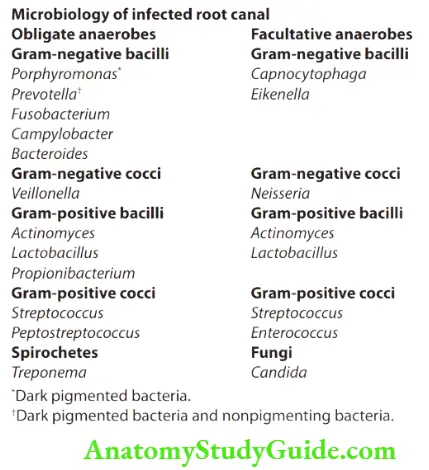
Identification Of The Bacteria
Following tests can be done to detect microorganisms and their sensitivity to a particular antibiotic.
Gram’s Stain:
- It was developed by Christian Gram in 1884.
- It helps in differentiating bacteria in Gram-positive and Gram-negative organisms.
Culture:
Culture taking method though done less these days still holds its importance because of a wide range of bacteria found in endodontic infections.
Microbiology of Endodontic Infections
Principle of Culturing:
Culturing of root canals is done for two main reasons:
- In the cases of persistent infection, to grow and isolate the microbial flora for antibiotic sensitivity and resistance profiles.
- To assess the bacteriologic status of the root canal system before obturation and determine the effectiveness of the debridement procedure.
Types of tissue cultures
1. Cell culture:
It is an in vitro growth of cells; although the cells proliferate, they do not organize into tissue.
2. Anaerobic culture:
This culture is carried out in the absence of air.
3. Pure culture:
This culture consists of a single-cell species, without the presence of any contaminants.
4. Primary culture:
Refers to cultures prepared from tissues taken directly from animals.
5. Secondary culture:
It refers to a subculture derived from a primary culture.
6. Plate culture:
This culture is grown on a medium, usually agar or gelatin, on a petri dish.
7. Streak culture:
In this culture, the medium is inoculated by drawing an infected wire across it.
8. Suspension culture:
It refers to a culture in which cells multiply while suspended in a suitable medium.
9. Slant culture:
This culture is made on the surface of solidified medium in a tube which has been tilted to provide a greater surface area for growth.
10. Stab culture:
In this culture, the medium is inoculated by thrusting a needle deep into its substance.
11. Tissue culture:
It refers to the culture in which maintenance or growth of tissue, organ primordia, or whole or part of an organ in vitro is done so as to preserve its architecture and function.
Types of Culture Medium:
- Liquid (broth)
- Solid (agar)
- Semisolid
Microbiology of Endodontic Infections
Liquid culture medium:
- The original liquid media developed by Louis Pasteur contained wine or meat broth.
- In liquid media, nutrients are dissolved in water, and bacterial growth is indicated by a change in the broth’s appearance from clear to turbid.
- A minimum of 10 6 bacteria per milliliter of broth are required for turbidity to be detected with the unaided eye.
- The formation of turbidity is directly proportional to bacterial growth.
Solid media:
- It was developed by Robert Koch in 1881. It contained pieces of potato, gelatin, and meat extract.
- Since gelatin is used to liquefy at 24°C, so he substituted it with agar.
Bacteriological media:
It consists of water, agar, growth-enriching constituents like yeast extract and blood.
Anaerobic Culture Method:
- An anaerobic bacteria culture is a method used to grow anaerobes from a clinical specimen.
- Anaerobic bacterial culture is performed to identify bacteria that grow only in the absence of oxygen.
Culture Technique:
For culturing, samples can be obtained either from an infected root canal or from a periradicular abscess.
Sample from draining root canal:
- Isolate the tooth with a rubber dam. Disinfect the surface of the tooth and surrounding area with betadine, chlorhexidine, or sodium hypochlorite.
- Gain access in the root canal using sterile burs and instruments. If there is drainage, collect the sample using a sterile needle and syringe or sterile absorbent paper points. Place the aspirate in anaerobic transport media
Sample from the dry canal.
- To sample a dry canal, use a sterile syringe to place transport media into the canal.
- Take the sample using a syringe or paper points and place the aspirate in anaerobic media.
Microbiology of Endodontic Infections
Sample from the abscess:
- Palpate the fluctuant abscess and determine the most dependent part of swelling.
- Disinfect the surface of mucosa with alcohol or iodophor
- Penetrate a sterile 16–20 gauge needle in the surface and aspirate the exudates
- Inject this aspirate into anaerobic transport media.
Culture Reversal
- Sometimes negative culture becomes positive after 24–48 hours
- So it is advised to allow >48 h between taking culture and obturation
Advantages of culturing method
- Culture helps to determine the bacteriological status of the root canal
- It helps to isolate microbial flares for resistant profiles and for antibiotic sensitivity.
- Helps in the identification of a broad range of microorganisms.
Disadvantages of culturing method:
- Unable to grow several microorganisms which can give false negative results.
- Strictly depend on the mode of sample transport which must allow the growth of anaerobic bacteria.
- Low sensitivity and specificity
- Time-consuming
- Expensive and laborious
Molecular Diagnostic Methods:
Advantages of molecular methods
- Helpful in the detection of both cultivable and uncultivable microbial species
- Higher sensitivity
- Have greater specificity
- Less time-consuming
- Do not need special control for anaerobic bacteria
- Are useful when a large number of samples are needed to be analyzed for epidemiologic studies
- Do not require cultivation
- Can be identifid even when they are viable
- Can be used during antimicrobial treatment
- A large number of samples can be stored at low temperatures and surveyed at once
3. To overcome the disadvantages of the culturing method, various molecular diagnostic methods have been developed.
4. Molecular diagnostic methods identify the microorganisms using genes as a target which are unique for each species. These are classified into four categories:
- Hybridization
- Amplification
- Sequencing
- Enzyme digestion of nucleic acid
Microbiology of Endodontic Infections
DNA–DNA Hybridization Method:
- This method uses DNA probes which target genomic DNA or individual genes.
- It helps in the simultaneous determination of the presence of a multitude of bacterial species in single or multiple clinical samples and is especially useful for large-scale epidemiologic research.
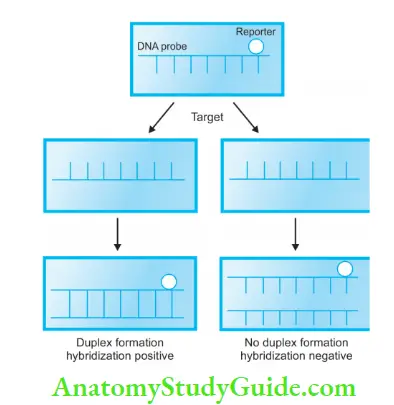
- It employs the use of DNA probes, single-stranded DNA, labeled with an enzyme or radioactive isotope, which locates and binds to complementary nucleic acids sequence of known identity to form a double-stranded molecule or hybrid.
- Since hybridization requires nucleic acid sequence homology, a positive hybridization reaction between two nucleic acid strands, each from a different source, indicates a genetic relationship the between two organisms that were formed.
Advantages of DNA–DNA hybridization method:
- It can be used for large-scale epidemiological research
- Allows simultaneous detection of multiple species
- Microbial contaminants are not cultivated, and their DNA is not amplified.
Disadvantages of DNA–DNA hybridization method
- Cross-reaction can occur on nontarget microorganisms
- Identifies only cultivable microorganisms
- Does not detect unexpected
- Detects only target microorganisms
Microbiology of Endodontic Infections
Amplification/Polymerase Chain Reaction Method
Though hybridization methods are highly specific for the detection of microorganisms and identification, they have less sensitivity. So, if sufficient target nucleic acid in the reaction is not present, false-negative results occur. Hence, hybridization methods necessitate the “amplification” of target nucleic acid by multiplying the target organisms to bigger numbers in the culture.
The three strategies for molecular amplification are target nucleic acid amplification, nucleic acid probe amplification, and amplification of the probe “signal.” The polymerase chain reaction (PCR) method involves in vitro replication of DNA; therefore, it is also called the “genetic xeroxing” method.
Here, multiple copies of specific regions of DNA are made by
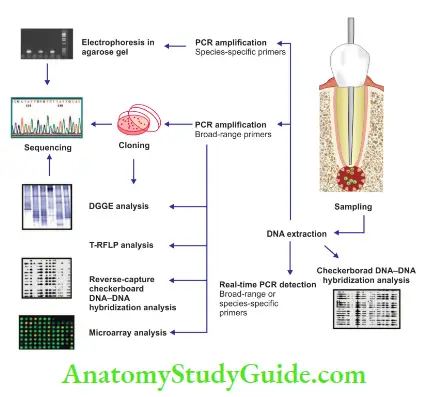
repeated cycles or heating and cooling. Then this amplified target formed is detected by different methods like:
- Electrophoresis in agarose gel
- Cloning and sequencing
- Microarray analysis
- Reverse capture checkerboard analysis
- DGGE (Denaturing Gradient Gel Electrophoresis)
Advantages of the PCR method:
- PCR has remarkable sensitivity and specificity because each distinct microbial species has unique DNA sequences.
- PCR can be used to detect virtually all bacterial species in a sample.
- It is also used to investigate microbial diversity in a given environment. Clonal analysis of microorganisms can also be done by PCR method.
Disadvantages of PCR method
- Identify microorganisms qualitatively not quantitatively
- Detect only target microorganisms
- Diffilt in microorganisms with thick walls like fungi
- Possibility of false positive and negative results
Microbiology of Endodontic Infections
How To Combat Microbes In The Endodontic Therapy
The microbial ecosystem of an infected root canal system and the inflammatory response caused by it will persist until the source of irritation is completely removed. The main factor which is needed for successful treatment of pulp and periradicular inflammation is the complete removal of the source of infection such as microorganisms and their by-products.
The following measures should be taken to completely get rid of these irritants.
Thorough Cleaning and Shaping of the Root Canal System:
Cleaning and shaping followed by three-dimensional obturation of the root canals have been shown to produce complete healing of periradicular tissue.
Complete debridement of the canal should be done with adjunctive use of irrigants like sodium hypochlorite which efficiently removes bacteria as well as their substrate from irregularities of the canal system where instruments cannot reach such as fis, indentations, cul-de-sacs, etc.
Oxygenating a Canal:
Oxygenating a canal simply by opening it is detrimental to anaerobes. The use of oxygenating agents as glycoside can be of great help, but care should be taken to avoid inoculation of these oxygenating agents into periapical tissues.
Drain:
A tooth with serous or purulent or hemorrhagic exudate should be allowed to drain with a rubber dam in place for a time under supervision. An abscess, which is a potent irritant, has an elevated osmotic pressure. This attracts more tissue flid and thus more edema and pain. Drainage by canal or by soft tissues decrease discomfort caused by
inflammatory mediators.
Antibiotics:
Antibiotics should also be considered as adjunctive in severe infections. The choice of antibiotic agent should be done on the knowledge of microorganisms associated with endodontic infections.
Intracanal Medicaments:
Intracanal medicaments play an important role in combating microorganisms.
Microbiology of Endodontic Infections
Use of Calcium Hydroxide in Canals:
Use of calcium hydroxide in canals with necrotic pulps after instrumentation has been shown to provide the beneficial results. Intracranial use of calcium hydroxide has shown to increase the efficiency of sodium hypochlorite and also the effectiveness of antimicrobial agents.
Calcium hydroxide powder is mixed with water or glycerin to form a thick paste which is placed in a pulp chamber with an amalgam carrier or a syringe. This paste is covered with a sterile cotton pellet, and access is sealed with a temporary restoration.
Endodontic Microbiology Conclusion
For a successful endodontic outcome, one must have an awareness of the close relationship between endodontic infections and microorganisms. The type of microbial flora develops according to the surrounding environment.
Microorganisms which are present in the untreated root canal have plenty of nutritional diversity, whereas microbial flora of root canal treated tooth is in dry space devoid of nutrition, so as per the environment the type of flora changes.
Therefore, we should obtain a better understanding of the characteristics and properties of bacteria along with environmental changes so as to increase the success of endodontic treatment.
Leave a Reply