Male ♂ Reproductive Organs Median Lobe Of Prostate
Median or middle lobe
Table of Contents
1. It lies behind the upper part of the urethra and is present in front of the ejaculatory duct.
2. It is closely related to the neck of the urinary bladder.
3. It produces an elevation in the lower part of the trigone of the bladder, known as the uvula vesicle.
Read And Learn More: General Histology Questions and Answers
Question – 1: Describe the prostate under following heads
1. Gross anatomy
2. Histology
3. Age changes, and
4. Applied anatomy.
Answer:
Male ♂ Reproductive Organs Introduction:
It is a fibro musculo glandular organ. It has fibrous, muscular and glandular parts. It is an accessory organ of the male ♂ reproductive system. It adds 30% of bulk to the seminal fluid. There is no counterpart in the female ♀.
1. Male ♂ Reproductive Organs Gross Anatomy
1. Situation: It is situated in the lower pelvis.
2. Dimension: Breadth is more than the length.
-
-
- Anteroposterior: 2 cm.
- Vertical: 3 cm.
- Transverse: 4 cm.
- Weight: 8 g (The word “prostate” has 8 letters which is equal to the weight.)
- Shape: It resembles an inverted cone

-
3. External features:
1. It has a base, an apex and three surfaces. The surfaces are
- Anterior
- Posterior, and
- Inferolateral.
2. The base is fused with the neck of the bladder. Apex is blunt. The urethra travels from base to apex. It is called the prostatic part of the urethra. It continues as the membranous urethra.
3. Consistency: It is firm in consistency and is formed by fibromuscular stroma.
4. Lobes: It has five lobes
Anterior lobe (Absence of glandular tissue): It is present in front of the prostatic urethra. There is no glandular tissue in the anterior lobe.
Posterior lobe: It is the part of the prostate present behind the prostatic urethra and connects two lateral lobes. It is a common site of the beginning of Primary carcinoma.
Median or Middle lobe: It lies behind the upper part of the urethra and is present in front of the ejaculatory duct. It is closely related to the neck of the bladder.
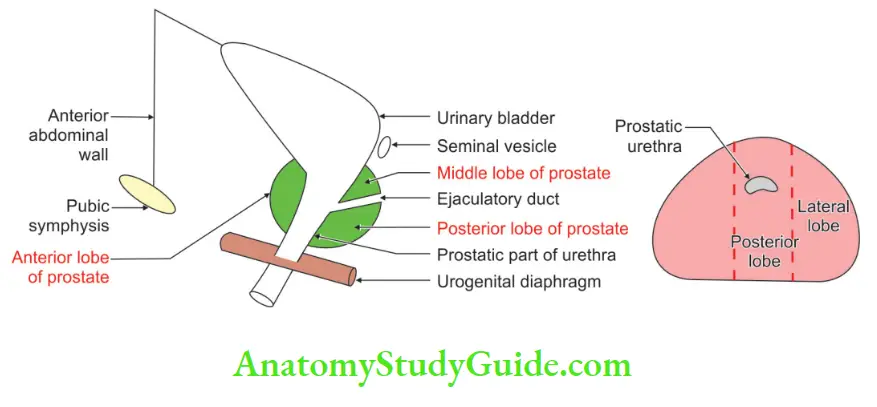
It produces an elevation in the lower part of the trigone of the bladder, known as the uvula vesicae. middle-aged tumour arises from the Median lobe.
Lateral lobes lie: Lateral lobes lie one on each side of the urethra.
5. Capsules: It has anatomical and pathological capsules.
Anatomical:
True capsule: It is a condensation of the fibrous connective tissue around the peripheral part of the gland. It contains no venous plexus.
False capsule: It lies outside the true capsule and is derived from the pelvic fascia. The prostatic venous plexus is embedded in it. Posteriorly, it is vascular and is formed by the rectovesical fascia of Denonvilliers) prostate-peritoneal fascia).
Pathological: In benign prostatic hyperplasia, the peripheral part of the gland gets compressed and is called a pathological capsule.
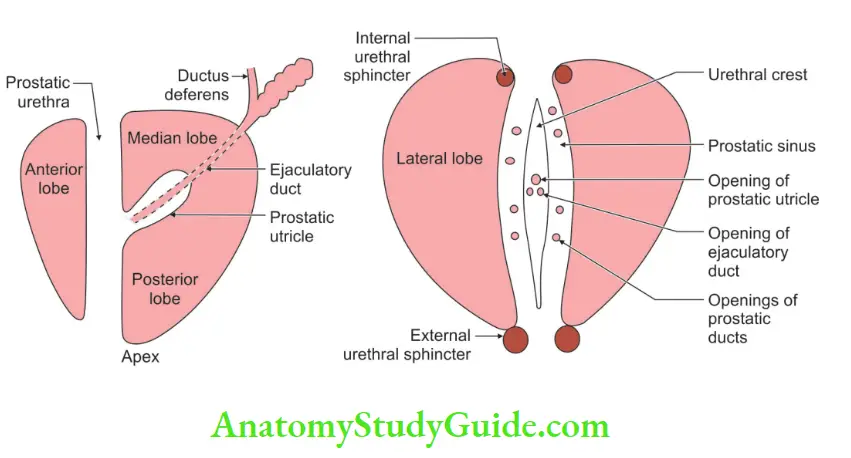
Structures within the prostate: The prostatic urethra is present at the junction of the anterior one-third and posterior two-thirds of the prostate.
- The prostatic utricle is a blind sac, one end of which opens into the urethra.
- The ejaculatory ducts open into the prostatic urethra on each side of the opening of the prostatic utricles.
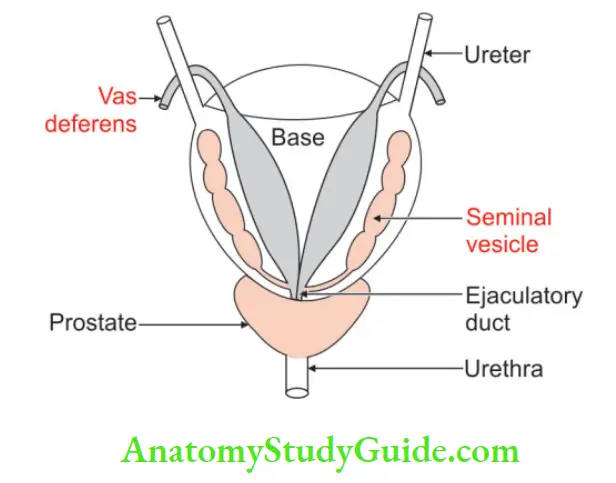
4. Relations:
Visceral relations are
Anteriorly:
- Retropubic space, and
- Pubic symphysis.
Superiorly: Neck of the urinary bladder.
Posteriorly: Rectum.
Inferiorly: Urogenital diaphragm and pelvic diaphragm.
Laterally: It is clasped by the levator prostate.
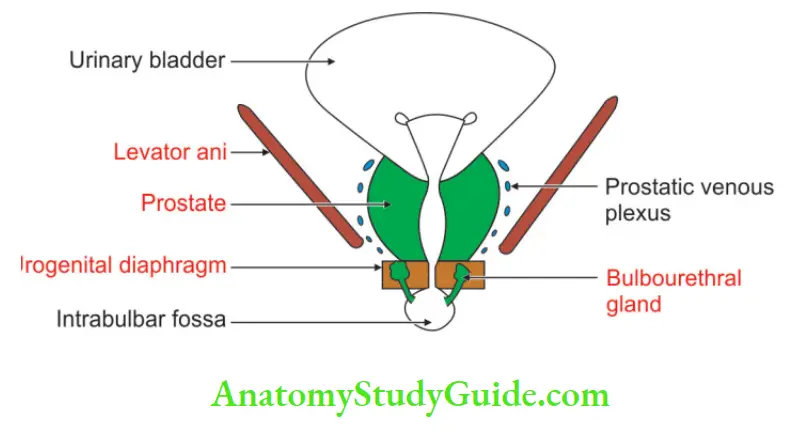
5. Blood supply:
Arterial supply: The prostate is supplied by
1. Prostatic branch of the inferior vesical artery which is the main artery of the prostate.
2. Small branches of
1. Middle rectal artery.
2. Internal pudendal arteries.
3. Branches of these arteries form two plexuses
- A large outer or subcapsular plexus, and
- Small inner or periurethral plexus. The greater part of the gland is supplied by the subcapsular plexus.
Venous drainage:
- The veins form a rich plexus around the sides and the base of the gland.
- They lie between true and false capsules.
- The plexus receives the deep dorsal vein of the penis.
- It communicates with the vesical plexus and forms the vesicoprostatic plexus.
- It is situated between the bladder and the prostate.
- There are no valves in these veins. There is free communication between the prostatic and vertebral venous plexuses.
- The malignant cells of the prostate spread to the vertebral column, skull and central nervous system.
6. Never supply:
1. The sympathetic nerve is derived from the inferior hypogastric plexus.
2. The parasympathetic nerve is derived from the pelvic splanchnic nerve.
- It contains thick nerves and numerous large ganglia.
- The plexus contains sympathetic and parasympathetic nerves.
The secretions of the prostate are produced by the sympathetic and discharged by the parasympathetic nerve (pelvic splanchnic nerve).
7. Lymphatic drainage :
The lymphatics of the prostate pass across the pelvic floor to the nodes on the side wall of the pelvis. They pass along the internal iliac vessels.
They mainly drain into:
- Internal iliac lymph node, and
- Sacral group of lymph nodes
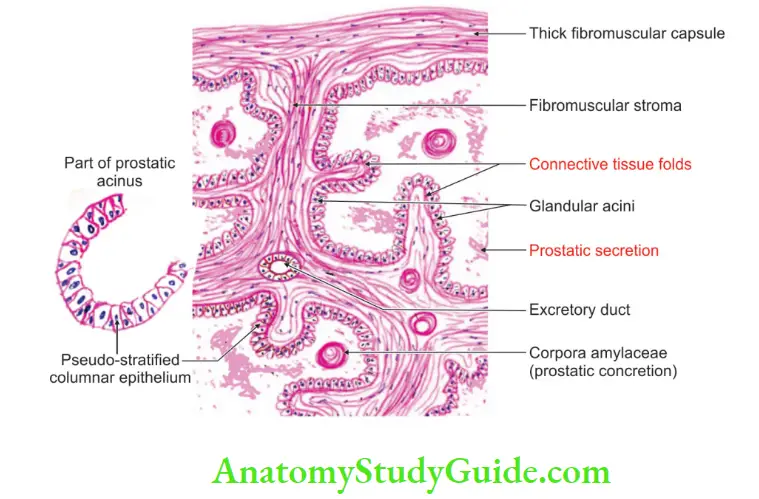
2. Male ♂ Reproductive Organs Histology
It is fibromuscular glandular tissue.It contains
1. Fibrous stroma
2. Smooth muscle, and
3. The acini of varying shapes and sizes.
It contains large cavities which are lined by columnar epithelium. There are infoldings of the epithelium which is a distinguishing feature. It is divided into
Outer larger zone: It contains large branched glands with ducts which curve backwards and open into the prostatic utricle.
Inner smaller zone: It contains
- Submucous glands opening in prostatic sinuses.
- Simple mucosal glands are thrown into folds.
4. Small rounded masses of uniform or laminated structures are found within the lumen of the follicles.
They are called amyloid bodies or corpora amylacea. These are more abundant in older individuals.
This consists of a condensed glycoprotein. They are often calcified.
5. The fibromuscular tissue forms a conspicuous feature of the section of the prostate.
3. Male ♂ Reproductive Organs Age Changes In Prostate
At birth: Prostate is made up mainly of stroma which consists of simple ducts.
1. During the first 6 weeks, the epithelium of the duct and of the prostatic utricle undergoes hyperplasia and squamous metaplasia.
2. Between 9 and 14 years, there is a proliferation of the duct system and the glands slowly increase in size.
At puberty: It becomes double in size. The stroma is condensed and markedly reduced.
- From 20 to 30 years, there is a proliferation of glandular elements and the infolding of the glandular epithelium.
- From 30 to 45 years, size remains constant.
- After 45 to 50 years, the prostate is either enlarged or reduced in size.
4. Male ♂ Reproductive Organs Applied anatomy
1. Prostatitis: It is an inflammation of the prostate gland.
2. About tumours of the prostate:
1. Benign hypertrophy of the prostate (Middle age adenoma) occurs in the Median lobe.
2. It is a local proliferation of the internal zone or central region, the region of the mucosal or periurethral gland.
3. Anterior lobe of the prostate has an absence of glandular tissue. Hence, benign hypertrophy never occurs in the anterior lobe.
4. The prostate is a common site of carcinoma.
5. It can spread to the vertebral column and skull because of the communication of prostatic and vertebral venous plexuses.
6. Primary carcinoma occurs in the peripheral zone (Posterior lobe).
7. The spread of cancer of the prostate to the rectum is prevented by Denonvilliers’ fascia.
3. An approach to the prostatectomy:
Transvesically: Across the bladder
Retropubically: The approach of the prostate is from behind the pubis. It is through the prostatic capsule.
Perineal approach: Across the perineum, dissecting in front of the rectum and reaching the prostate through Denonvilliers’ fascia.
Transurethral: The obstructed mass of prostatic tissue is removed by operating a cystoscope.
- In transurethral resection, the verumontanum (colliculus seminalis) is an important landmark.
- The surgeon keeps proximal to this point in order not to damage the urethral sphincter mechanism.
- An abdominal suprapubic incision into the retropubic space gives a wide exposure to the organ.
4. About prostatectomy:
1. Prostatectomy is the enucleation of a hyperplastic mass of glandular tissue of the prostate gland.
2. In performing enucleation of the prostate, the surgeon enters the plane between the pathological capsule and the true capsule.
3. The tumour is enucleated and a pathological capsule is left behind.
4. The prostatic venous plexus, lying external to the pathological capsule and internal to the false capsule, is thus undisturbed.
5. In chronic obstruction due to an enlarged prostate, the bladder walls show a typical trabeculated open weave appearance. It is seen through a cystoscope.
Benign Prostatic Hypertrophy
Benign hypertrophy of the prostate (middle-age adenoma):
It occurs in the median lobe. The median lobe surrounds the urethra. There is the local proliferation of the internal zone or central region.
1. It occurs in 45 to 50 years of age.
2. It causes retention of urine due to distortion of the urethra.
- Enlargement of the prostate projects into the urinary bladder.
- It acts as a valve over the internal urethral orifice. The blockage is proportionate to strain.
- The more patient strains, the more it obstructs the passage.
3. Prostatectomy is done to relieve the symptoms.
4. It is removed through
- Transurethral prostatectomy
- Retropubic prostatectomy
- Perineal prostatectomy
Leave a Reply